Manual Lymphatic Drainage vs Machine-Based vs Medical Lymphatic Drainage: What's the Difference?
When people talk about “lymphatic drainage” these days, they may be thinking of three quite different things: Manual Lymphatic Drainage (MLD) performed by a trained therapist, machine-based lymphatic treatments, such as pressotherapy suits or compression devices, and medical lymphatic drainage carried out under clinical supervision as part of a prescribed treatment plan.
All three approaches aim to support the lymphatic system– the body’s natural waste and fluid management network– but they work in different ways, have different training requirements, and are best suited to different situations.
My aim isn’t to say that one is “better” than the other, but to help you understand when and why each might be used.
Swelling can feel confusing, frustrating, and at times overwhelming.
And when you start looking for support, you’ll often come across two common options:
- Manual Lymphatic Drainage (MLD)
- Machine-based treatments (often called pneumatic compression devices)
At first glance, they can sound like they do the same thing.
But in reality, they work in very different ways — and understanding that difference matters more than people realise.
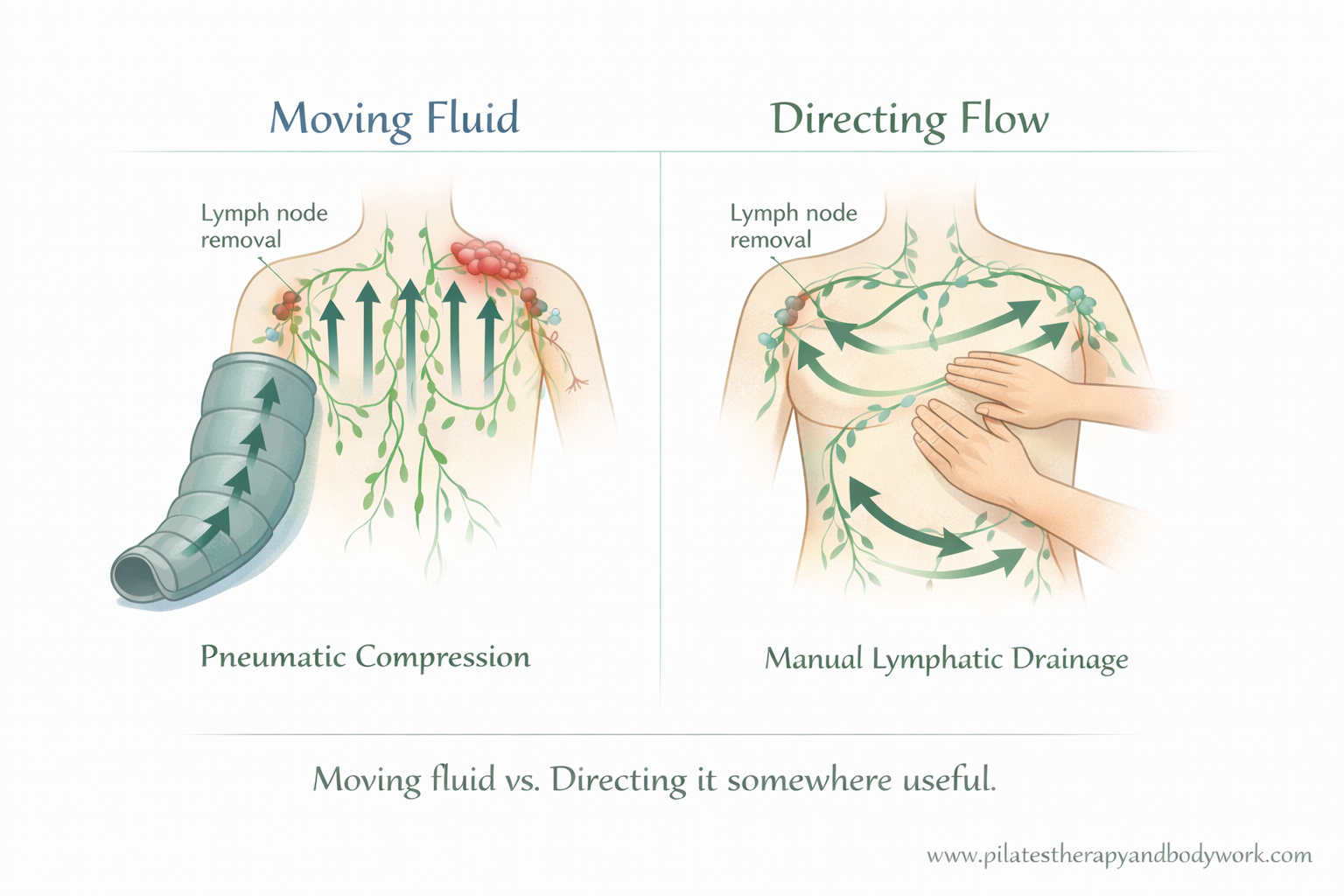
What is Manual Lymphatic Drainage (MLD)?
Manual Lymphatic Drainage is a very gentle, hands-on therapy that works with the body’s lymphatic system.
Using light, rhythmic movements, it aims to support the movement of lymph fluid through the body and encourage drainage through healthy pathways.
It’s widely used as part of Complete Decongestive Therapy (CDT) — the gold standard approach for managing lymphoedema within the NHS and internationally.
Research consistently shows that MLD can:
- Support lymphatic flow
- Reduce swelling
- Improve comfort and tissue quality
- Support relaxation and nervous system regulation
(International Society of Lymphology, 2020; NHS guidance on lymphoedema management)
What are machine-based treatments?
Machine-based treatments, often called pneumatic compression devices, use inflatable sleeves that rhythmically inflate and deflate.
These devices:
- Apply pressure to the limb
- Encourage fluid movement proximally
- Can be used in clinics or at home
There is good evidence that compression (including these devices) can help reduce limb volume — particularly when used as part of a wider management plan.
(NHS, 2023; systematic reviews on compression therapy in lymphoedema management)
What is medical lymphatic drainage?
Medical lymphatic drainage is a broader, clinical approach prescribed and monitored by specialist trained practitioners or nurses– usually for patients with a diagnosed condition sych as lymphoedema.
It may include:
• Manual lymphatic drainage techniques, performed by a specialist trained therapist within a medical team
• Medical-grade pneumatic compression devices (higher grade versions of the machines used in wellness or sports settings)
• Compression bandaging or garments as part of a wider programme
• Prescribed exercise programme
Together these for part of Decongestive Lymphatic Therapy (DLT)usually known as Complete Decongestive Therapy (CDT), the gold standard in lymphoedema management.
Medical lymphatic drainage is particularly helpful for:
• Cancer-related or secondary lymphoedema
• Severe or complex swelling
• Post-cancer surgery recovery where swelling is persistent
• Cases requiring long-term management and monitoring
Access can be limited (for example, via the NHS or specialist private clinics), and sessions may feel more clinical than a relaxation-focused MLD appointment. However, they are evidence-based and integrated into wider medical care, which makes them essential for many patients.
Why “moving fluid” isn’t always the full story
This is where things start to matter a little more.
One of the biggest misconceptions I see in clinic is this idea:
– If we move the fluid, we fix the problem
But the lymphatic system isn’t just a set of tubes to be emptied.

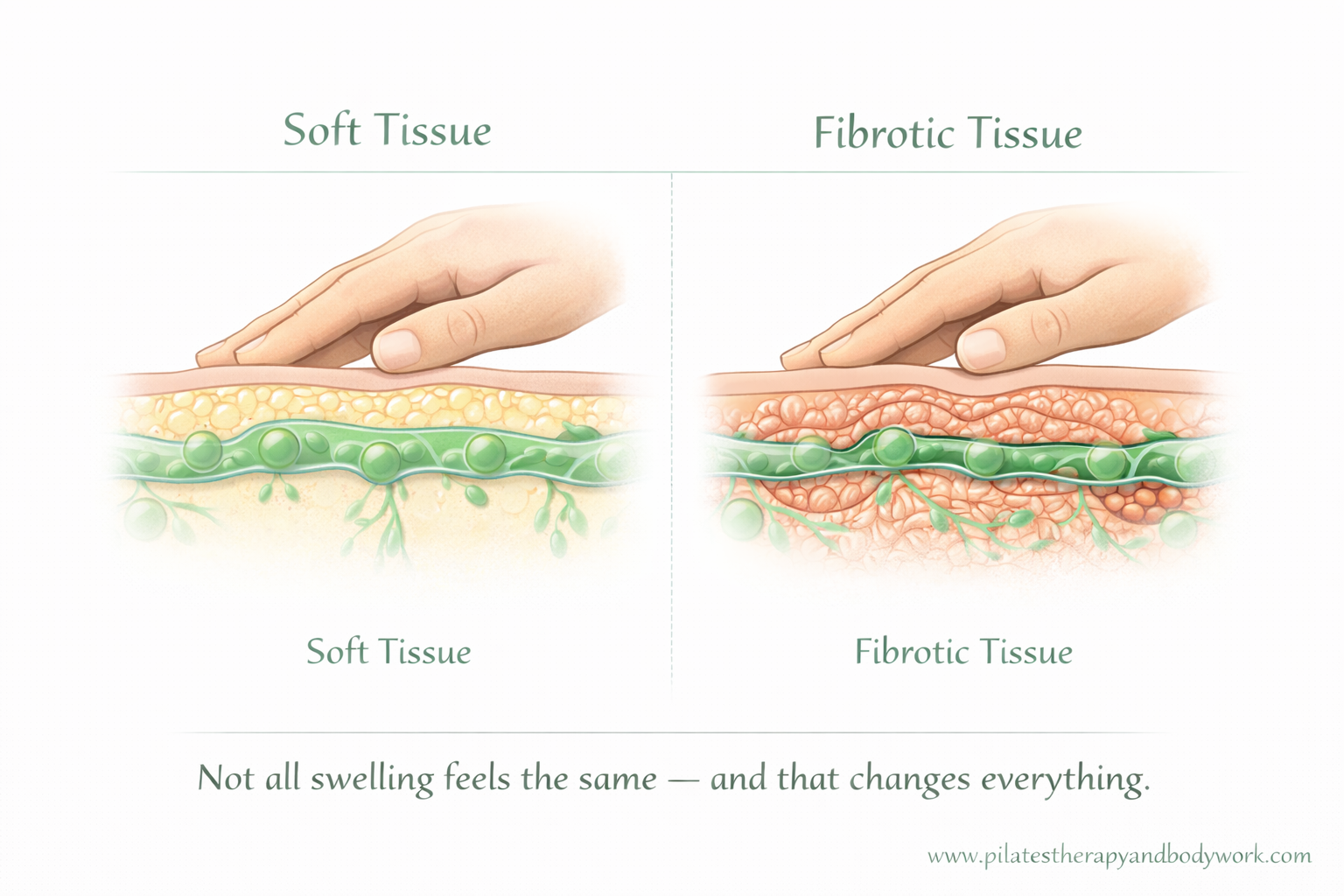
It’s a responsive, adaptive system, and swelling can happen for different reasons:
- Increased fluid load (dynamic insufficiency)
- Reduced transport capacity (mechanical insufficiency)
- Surgical disruption
- Fibrosis or tissue change
- Inflammation
So the real question isn’t just:
– Can we move fluid?
It’s:
– Where should that fluid go, and can the system cope when it gets there?
Research and clinical guidelines highlight that effective lymphatic treatment relies on redirecting fluid to functioning lymphatic territories, not simply pushing it along existing pathways (International Society of Lymphology, 2020).
Not all “drainage” is the same
Both MLD and compression can move fluid.
But they do it in very different ways.
Manual Lymphatic Drainage:
- Works with lymphatic anatomy and watersheds
- Clears proximal areas (terminus) first
- Redirects fluid to healthy, available pathways
- Adapts in real time to the person in front of you
Machine-based compression:
- Follows a preset sequence
- Applies pressure from distal to proximal
- Assumes pathways are open and functioning
- Cannot adapt to tissue changes or surgical disruption
– This is the key difference:
Moving fluid is not the same as improving lymphatic drainage.
When might you choose one over the other?
. • After surgery (including cancer surgery, cosmetic surgery, or orthopeadics)– MLD is generally recommended, because it is gentle, precise, and safe when delivered by a properly trained therapist. It also addresses scar tissue and pain sensitivity, which machines cannot.
• For sports recovery or mild swelling– A machine-based treatment might be convenient, accessible, and cost-effective, particularly for people without complex medical needs.
• For ongoing medical conditions (like lymphoedema)– MLD is often the cornerstone, with machines sometimes used as an adjunct to support long-term management, but usually under professional guidance.
• For relaxation and nervous system support– nothing quite replaces the human touch of MLD– its calming, parasympathetic effect is one of its greatest benefits.
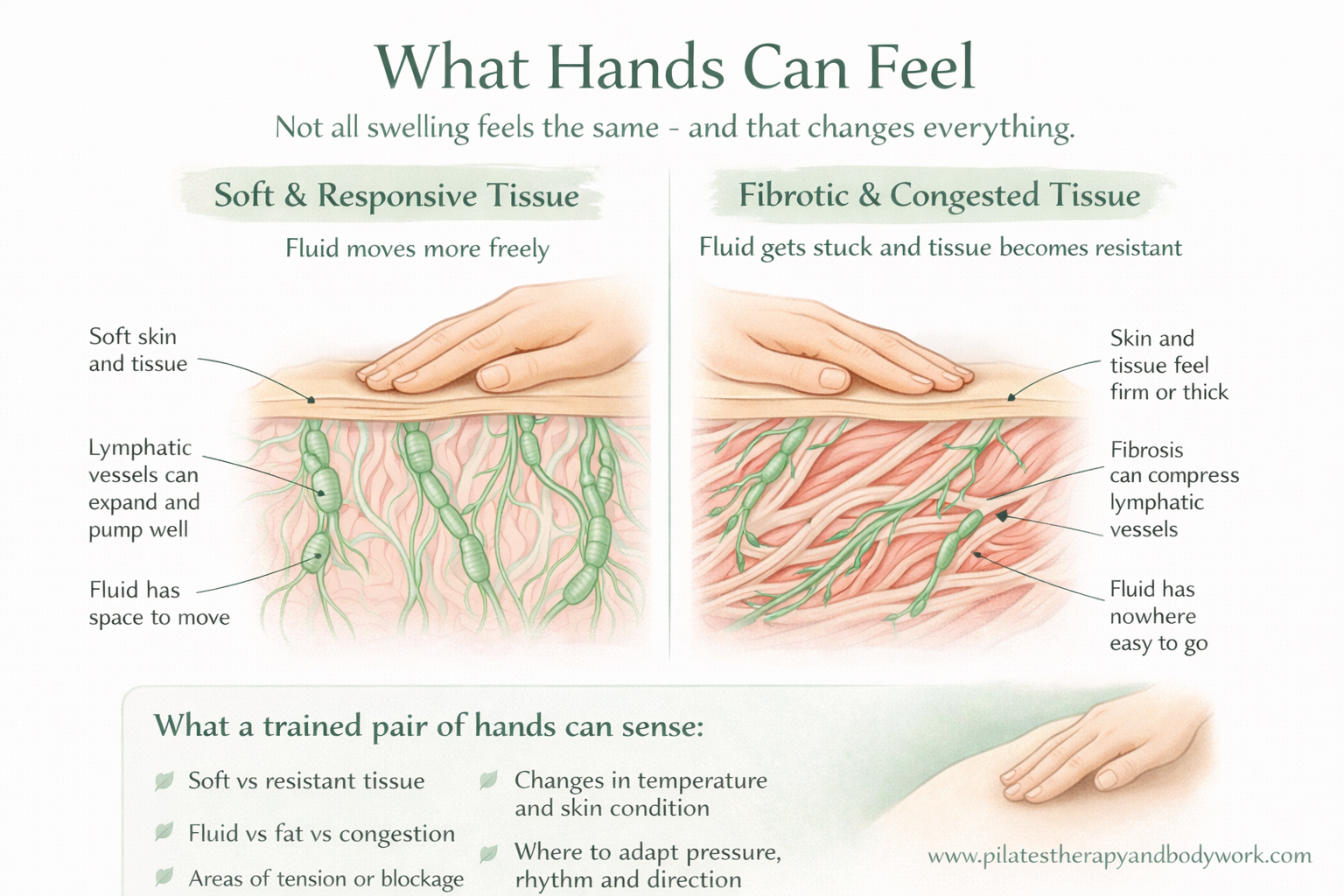
What a trained pair of hands can feel and respond to
In clinic, treatment isn’t a routine — it’s a constant decision-making process.
A trained practitioner can assess:
- Tissue softness vs fibrosis
- Fluid vs fat vs congestion
- Areas of resistance or blockage
- Skin condition and inflammation
- Surgical pathways and scar influence
And then adjust:
- Direction (using watersheds)
- Pressure (to support lymphangion activity without overload)
- Rhythm (stimulating or calming)
- Sequence (always working proximal before distal)
This level of responsiveness is what allows treatment to be both effective and safe.

Where machines can be helpful — and where guidance matters
Compression devices absolutely have a place.
Research shows compression is often more effective at reducing limb volume than MLD alone, which is why it forms a core part of CDT.
(Systematic reviews in lymphoedema management literature)
They can be helpful:
- As part of a structured programme
- For ongoing management
- When pathways are already supported and open
But used in isolation, without clinical reasoning, they can:
- Increase pressure in already overloaded areas
- Push fluid into regions with reduced capacity
- Miss underlying tissue changes such as fibrosis
– It’s not that they are wrong —
– it’s that they are non-specific
— it’s not either/or
This isn’t about choosing one over the other.
In many cases, the most effective approach includes:
- Manual Lymphatic Drainage
- Compression (bandaging or garments)
- Movement and breathing
- Skin care
- Education and long-term management
This combined approach is what forms Complete Decongestive Therapy (CDT).
A simple way to think about it
If I were to simplify it for my clients, I’d say:
- MLD helps create space and guide flow
- Compression helps maintain and support that movement
Both are valuable.
But without understanding the system underneath, we risk doing more… rather than doing what’s needed.
If you’re dealing with swelling, the most important thing isn’t choosing a treatment…
It’s understanding why the swelling is there in the first place.
Because that’s what guides the right approach.
If you’re unsure about your swelling, or you’ve been trying different approaches without clear results, you’re very welcome to get in touch.
I offer specialist Manual Lymphatic Drainage, reflexology, and gentle movement support in:
- Clacton-on-Sea
- Bury St Edmunds
- Across Essex and Suffolk
This work is about understanding your body — not just treating symptoms.

To book a Manual Lymphatic Drainage Session or ask me about it, call 07767 384983 or email me fi@therapyinmotion.co
