
Surgery is a huge event for the body.
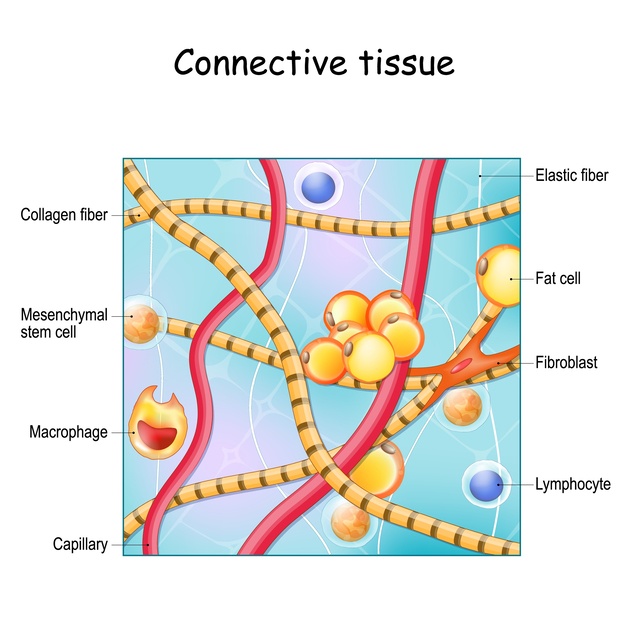
Even when everything goes well, tissues are cut, moved, stretched and stitched back together. Blood vessels, connective tissue and sometimes lymphatic vessels are disrupted as part of the procedure.
So it’s very common to experience swelling, tightness and fluid build-up after surgery.
One of the questions I’m hearing more and more in clinic is:
“Should I have lymphatic drainage after surgery?”
The short answer is that not everyone needs it, but many people benefit from understanding how the lymphatic system supports healing.
Let’s look at what the research tells us.
Surgery and swelling – what actually happens?
Whenever surgery takes place, the body triggers an inflammatory healing response.
This process is essential for repair, but it also causes fluid accumulation in the tissues.
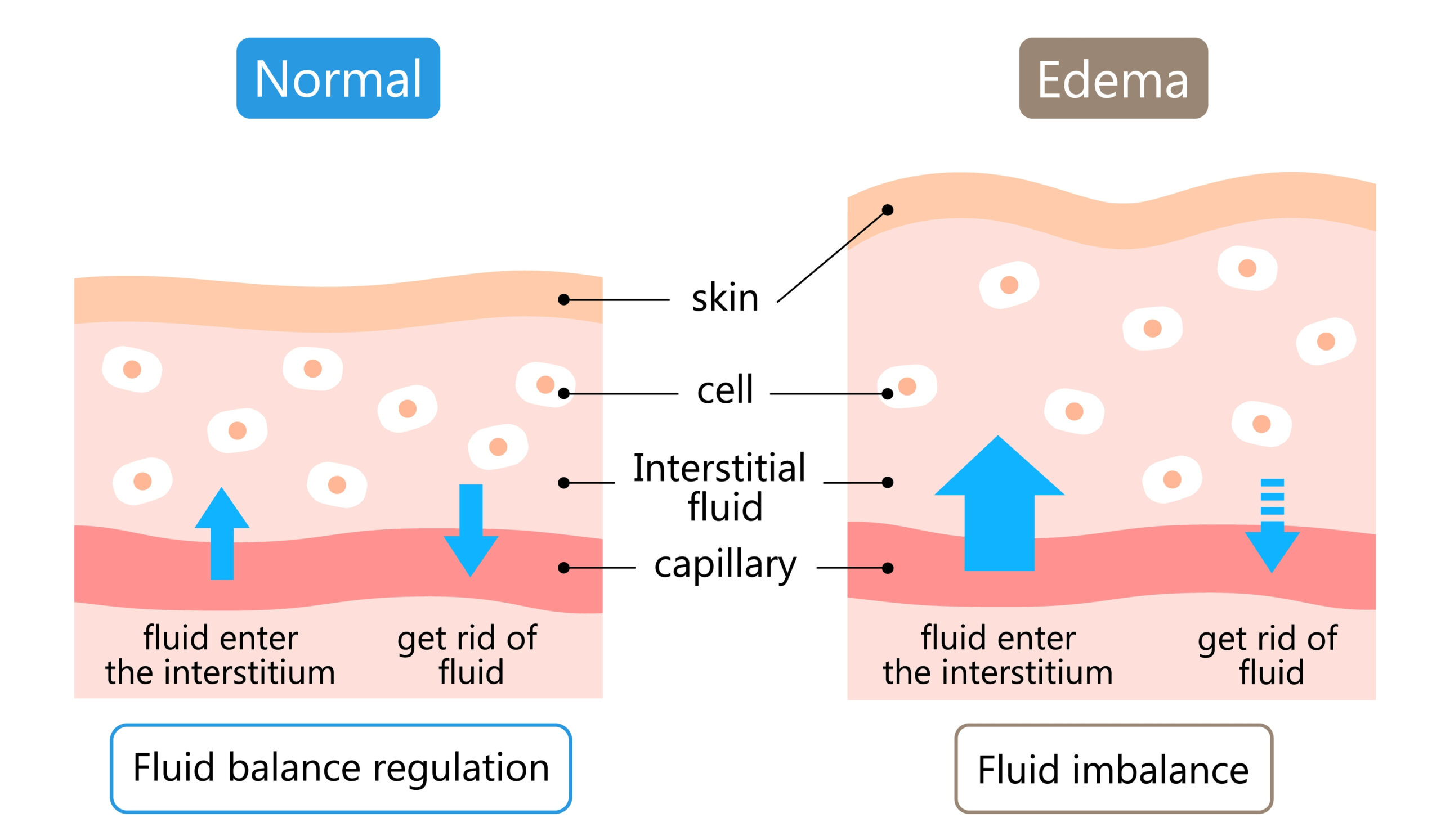
Swelling happens because:
• blood vessels leak fluid into surrounding tissue
• inflammatory chemicals attract immune cells
• damaged lymphatic vessels temporarily reduce fluid transport
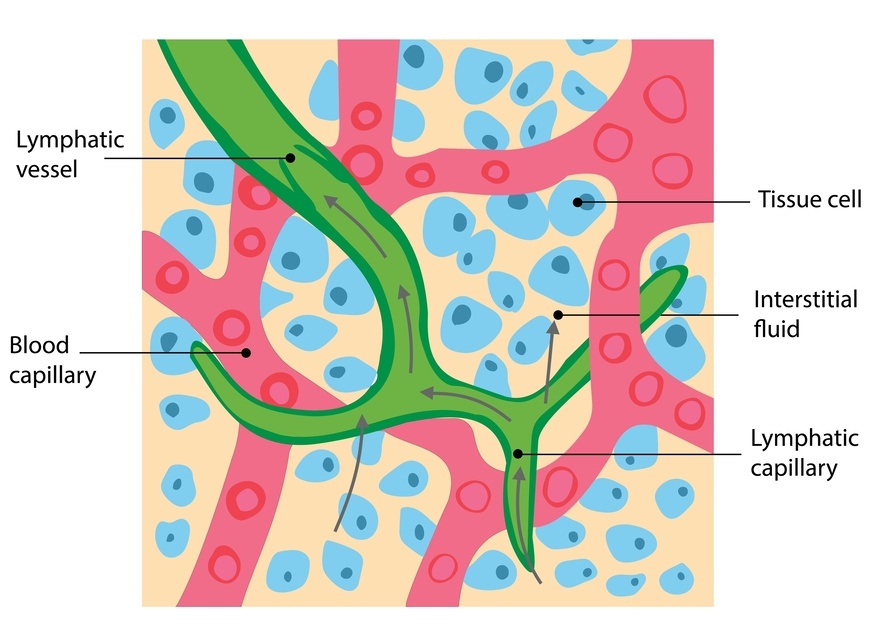
Normally the lymphatic system collects this excess fluid and returns it to circulation. But after surgery the system may simply be overloaded or temporarily disrupted.
That’s why swelling often peaks in the first few days and then gradually reduces.
Research shows that lymphoedema develops in around 15–30% of people after breast cancer surgery, particularly when lymph nodes are removed or treated with radiotherapy.
Even when lymphoedema does not develop, many people experience temporary post-surgical swelling during the healing phase.



What is Manual Lymphatic Drainage?
Manual Lymphatic Drainage (MLD) is a very specific type of gentle therapy developed in the 1930s by Dr Emil Vodder.
It’s not a traditional massage.
The movements are slow, rhythmic and very light, designed to stimulate the skin and encourage lymph fluid to move through functioning lymph vessels and nodes.
In simple terms, it helps the body shift excess fluid and inflammatory waste products away from healing tissues.
Healthcare providers commonly use lymphatic drainage to manage lymphoedema after cancer treatment and other conditions that disrupt lymph flow.
What does research say about lymphatic drainage after surgery?
Evidence is growing across different areas of surgery.
Studies looking at postoperative recovery show that lymphatic drainage may help reduce swelling, discomfort and restricted movement.
For example:
• Research on surgical recovery found that patients receiving lymphatic drainage experienced significantly less swelling and pain compared with control groups in the first week after surgery.
• Systematic reviews also suggest that early lymphatic therapy may help reduce the risk of developing lymphoedema in patients who are already at higher risk following surgery.
Because of these effects, lymphatic drainage is increasingly used in cosmetic, orthopaedic and cancer-related surgery recovery to manage swelling and support healing.
Why swelling can slow healing
Fluid is a normal part of healing, but too much swelling can create problems.
Excess fluid can:
• increase pressure within tissues
• slow circulation
• restrict movement
• increase discomfort
The lymphatic system is responsible for removing this excess fluid and returning proteins, waste products and inflammatory molecules back into circulation.
When lymph flow improves, tissues often feel softer, lighter and less tight, which can help people move more comfortably during recovery.
What about scar healing?
Scar formation is another area where people often ask about support after surgery.
As a wound heals, the body lays down new collagen fibres to repair the tissue. This process is completely normal, but scars can sometimes become:
• tight
• raised
• sensitive
• restricted in movement.
Research suggests that lymphatic drainage may help reduce post-surgical fibrosis and tissue stiffness, both of which are linked with swelling and inflammation in healing tissues.
Scar therapy techniques are usually introduced once the wound has fully healed, helping to restore tissue mobility and comfort.
This is particularly helpful in areas where scars affect movement or posture, such as:
• abdominal surgery
• breast surgery
• caesarean sections
• joint surgery.
When lymphatic drainage may be helpful
You might consider lymphatic drainage after surgery if you notice:
• persistent swelling
• heaviness or tightness around the surgical area
• fluid pockets
• stiffness around scars
• slow recovery of movement.
It can also be helpful if you are at higher risk of lymphatic disruption, such as after lymph node removal during cancer treatment.
In many cases, people simply feel more comfortable once swelling begins to reduce.
A gentle word of caution
Manual lymphatic drainage should always be performed by someone trained in lymphatic therapy.
There are also situations where treatment needs to wait, such as:
• infection
• blood clots
• certain heart or kidney conditions.
A properly trained therapist will always assess whether treatment is appropriate.
Not all “lymphatic drainage” is the same
You may have noticed that many different treatments now use the term lymphatic drainage.
Some are spa treatments designed to promote relaxation or temporary fluid movement. Others are structured medical approaches used in hospitals and lymphoedema clinics.
The technique I use in clinic is based on the Vodder method of Manual Lymphatic Drainage, which is one of the longest-established clinical approaches and is widely used in lymphoedema treatment and cancer recovery.
Vodder-based MLD uses very specific, gentle movements designed to stimulate the lymphatic vessels and encourage fluid to move through functioning lymphatic pathways.
This is particularly important after surgery, when tissues are healing and the lymphatic system may be temporarily disrupted.
In some situations other techniques such as compression therapy, scar therapy or movement rehabilitation may also form part of the recovery process.
The most important thing is that treatment is appropriate for the stage of healing and the individual person.

The bigger picture
Healing after surgery isn’t just about the incision closing.
It’s about how the body restores circulation, fluid balance, tissue movement and confidence in movement again.
The lymphatic system is one of the body’s quiet recovery systems, working in the background to manage fluid, inflammation and immune activity.
Sometimes it just needs a little support.
If you are preparing for surgery or recovering now
If you’re preparing for surgery, you might also find these helpful:
Feel Free To Contact Me With Questions
If you are recovering from surgery and noticing swelling, tightness or discomfort, it can sometimes help to understand what your body is dealing with.
Manual lymphatic drainage, scar therapy and gentle movement are all ways of supporting the body’s natural healing processes.
If you’re local to Clacton-on-Sea, Essex or Bury St Edmunds, Suffolk, you’re always welcome to reach out if you’d like to explore whether this kind of support might help your recovery.
Sometimes a simple conversation can make things much clearer.
