“Something just doesn’t feel right…”
One of the most common things I hear in clinic is:
“I can’t quite explain it… it just feels different.”
Not always pain.
Not always swelling.
Just… unfamiliar.
After surgery — especially when lymph nodes are involved — your body is adjusting to a new normal. And sometimes that shows up in ways that are confusing, frustrating, or even a bit worrying.
Three of the most common things I see are:
- Tight, pulling sensations (cording)
- Heaviness or swelling (lymphatic changes)
- Tingling, burning, or odd sensations (nerve-related)
They can overlap.
They can come and go.
And they don’t always get explained very clearly.
Let’s slow it down.
11. When it feels tight and won’t stretch out — Cording (Axillary Web Syndrome)
Cording (also called Axillary Web Syndrome) often shows up as:
- Tight, pulling bands under the skin
- Discomfort when reaching or stretching
- A feeling of restriction through the arm, armpit, or even into the chest
Sometimes you can see or feel a thin “cord-like” line.
Sometimes you just feel the pull.

What’s actually happening?
We don’t have one single explanation, but current understanding suggests:
- It may involve lymphatic vessels and surrounding connective tissue
- There can be inflammation, tightening, and reduced glide through the tissues
- The body is healing… but the tissues aren’t moving as freely yet
How common is it?
Research suggests cording can affect:
- Around 20–30% of people after breast cancer surgery
- Some studies report higher rates (up to 50–70%) depending on the type of surgery and number of lymph nodes removed
(Koehler et al., 2015; Yeung et al., 2020)
Why movement matters here
Without gentle movement:
- The pulling sensation can feel worse
- Range of motion can reduce
- People often avoid using the arm → which reinforces the restriction
With the right movement:
- Tissue glide improves
- Confidence returns
- Function comes back more naturally
Not forcing.
Not pushing through pain.
But supported, progressive movement.
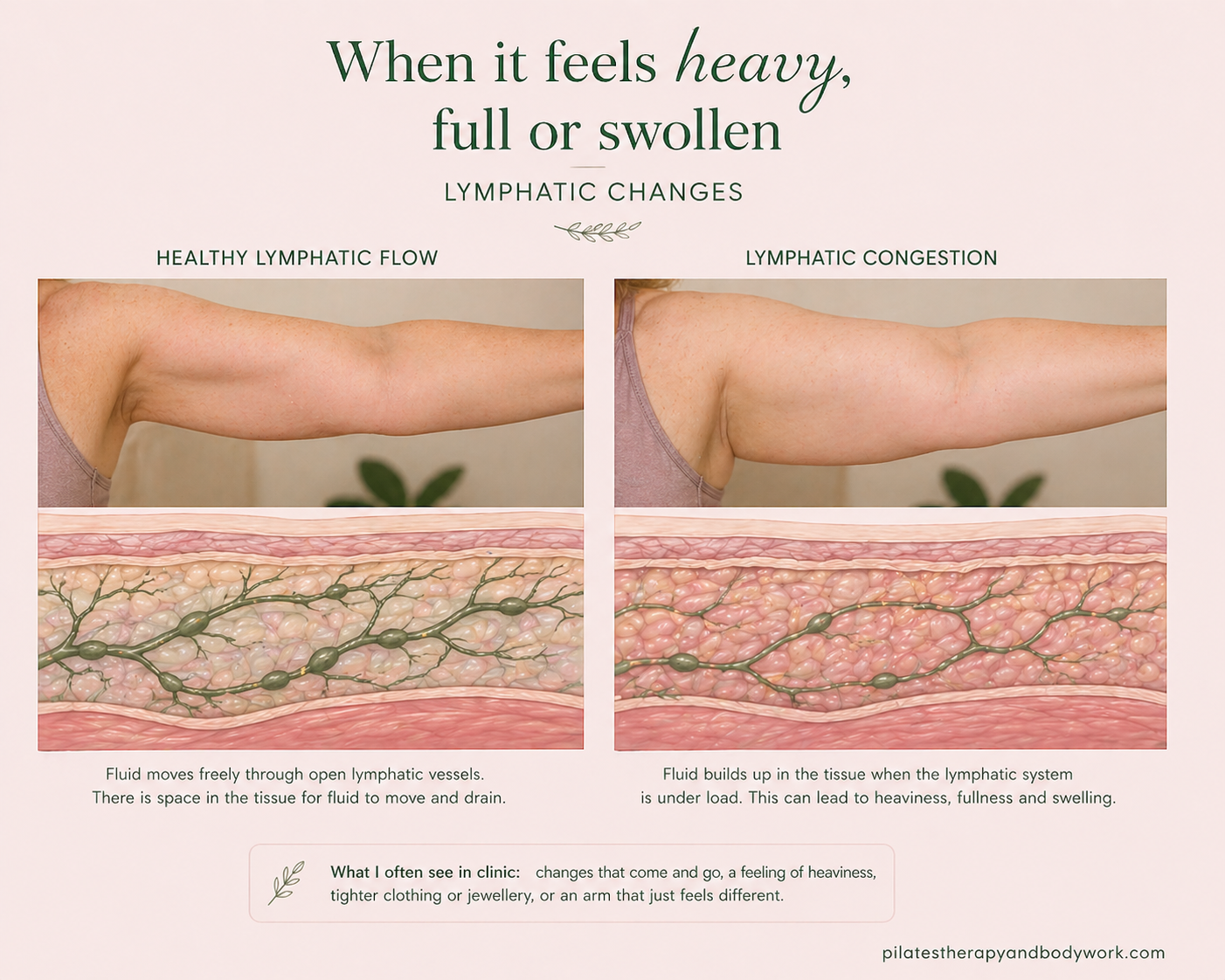
2. When it feels heavy, full, or swollen — Lymphatic changes (including lymphoedema)
This is where things often get misunderstood.
People expect swelling to be obvious.
But early on, it often isn’t.
Instead, you might notice:
- A feeling of heaviness or fullness
- Jewellery or clothing feeling tighter
- Changes that come and go
- A sense that the arm just feels… different
What’s happening underneath?
Your lymphatic system helps:
- Move fluid
- Clear waste
- Support immune function
After surgery or lymph node removal:
- The transport capacity can be reduced
- Fluid load may exceed what the system can comfortably move
- The space between tissues becomes more “crowded”
And this isn’t just water.
It’s:
- Fluid
- Proteins
- Cellular activity
Which is why, if left unmanaged, it can lead to longer-term tissue changes.
How common is lymphoedema?
Estimates vary, but:
- Around 20–40% of people after breast cancer treatment may develop lymphoedema
- Risk increases with:
- More lymph nodes removed
- Radiotherapy
- Infection or injury
(NHS; Macmillan Cancer Support)
3. When it burns, tingles, or feels strange — Post Mastectomy Pain Syndrome (PMPS)
This is the one that often worries people the most.
Because it doesn’t always behave like “normal pain”.
You might feel:
- Burning
- Tingling
- Sharp or “electric” sensations
- Numbness or altered sensitivity
- A strange mix of all of the above
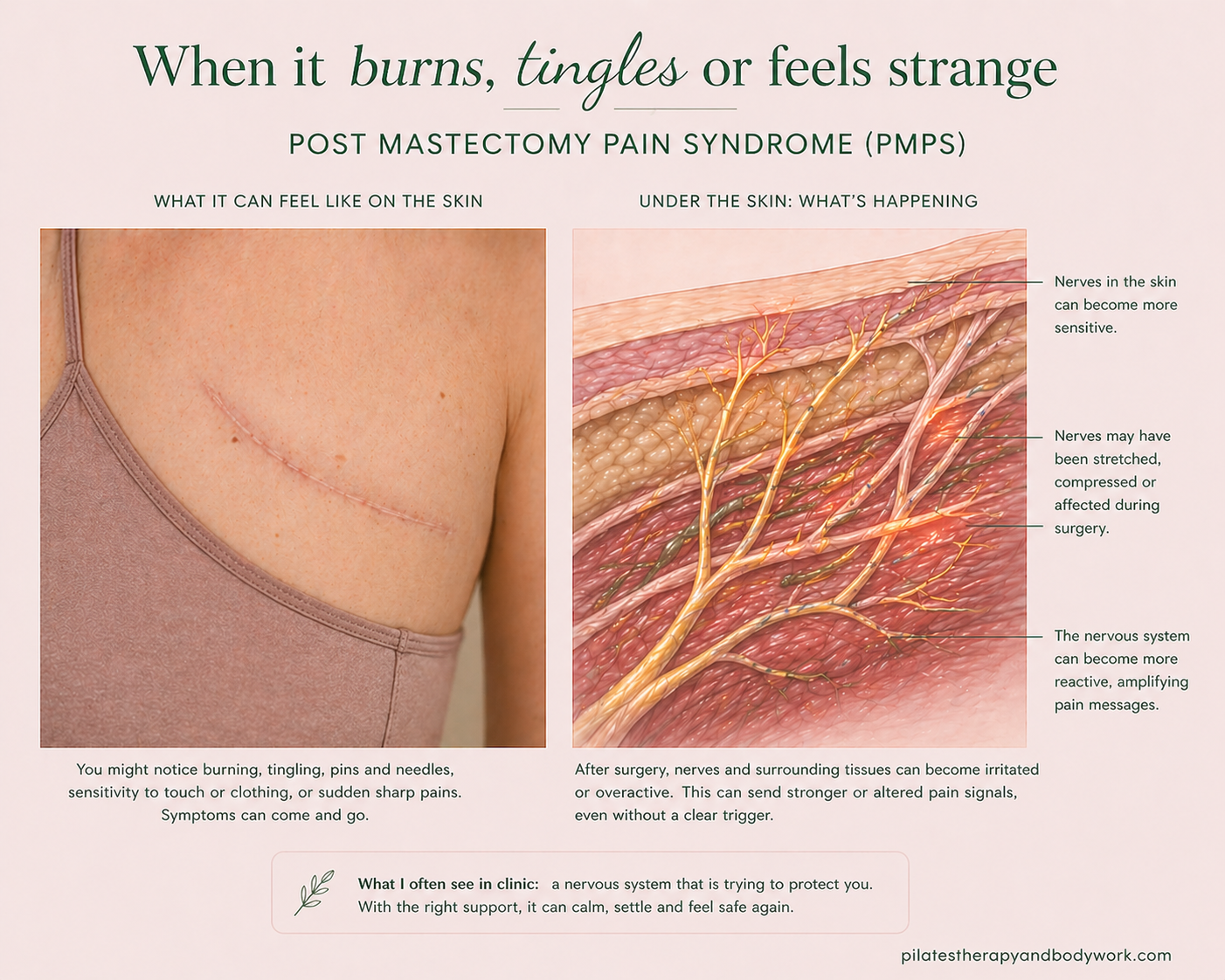
What’s going on?
This is usually linked to the nervous system adapting after surgery.
- Small nerves may have been affected
- The brain is still interpreting signals from the area
- The system can become more sensitive for a while
How common is it?
PMPS is more common than many people realise:
- Estimates range from 20–50% of patients after breast surgery
(Vilholm et al., 2008 and later reviews)
A quick word on fear, restrictions, and “what you should avoid”
You may have been told:
- Don’t lift
- Don’t use your arm too much
- Be careful with everything
And while caution has its place, current evidence supports something more balanced:
• Gradual, supported movement is safe and beneficial
Research shows:
- Exercise does not increase risk of lymphoedema when progressed appropriately
- Movement improves lymphatic flow, strength, and function
- Avoidance can actually delay recovery
(Schmitz et al., 2010; American College of Sports Medicine guidelines)
So what actually helps?
This is where support becomes individual.
But in general:
Gentle, guided movement
- Restores range
- Supports lymphatic flow
- Rebuilds confidence
Manual Lymphatic Drainage (MLD)
- Supports fluid movement
- Encourages lymphangiomotoricity
- Helps the system work more efficiently
Scar and soft tissue work
- Improves tissue glide
- Reduces restriction
- Supports overall function
Breath and posture
- The diaphragm plays a key role in lymphatic movement
- Small changes can make a big difference
Education
- Understanding reduces fear
- Fear reduces movement
- Movement supports recovery
Going along to your local cancer support groups can help reduce your fears. Peer support has been shown to improve quality of life and you will get lots of tips from real life lived experiences. And please don’t forget how valuable your support might be be to somone else.
Local to me- These sessions are held monthly, weekly or every other month.
Frinton – Breast Cancer Support
Touched by Cancer Frinton – email tbc.coffeedownload@gmail.com
Harwich Cancer Support – call Kelly 07585 559761
Sips of Support – Clacton – Call Holly 07362 470273
Lymphoedema Support group – Contact Lorna 07887925252
What support can look like (in real life)
In clinic, support often isn’t one single thing.
It might look like:
- Gentle Manual Lymphatic Drainage (MLD) to support fluid movement and reduce that heavy feeling
- Simple, guided movement sessions to restore confidence and range
- Scar and soft tissue work to help things move more freely again
- Or sometimes just a conversation that helps you understand what your body is doing
For some people, it starts on the treatment couch.
For others, it’s about building confidence to move again.
Movement beyond the clinic
This is also where something like WALX (supported pole walking) can be really helpful.
Not as fitness.
Not as performance.
But as rhythmic, supported movement:
- Encouraging natural arm swing
- Supporting posture
- Helping the lymphatic system through gentle, repeated motion
It’s one of the simplest ways to rebuild confidence in your body again — especially if things have felt uncertain.
For those who want a bit more structure, I also offer specialist cancer rehab sessions, where we build things back up gradually — at your pace.

And sometimes… it’s simpler than all of that
A walk.
A conversation.
A bit of fresh air with people who get it.
I’m part of the 5K Your Way Move Against Cancer group in Clacton, where people walk, jog, or just turn up — all at their own pace.
No pressure.
Just connection and gentle movement.
We meet on the last Saturday of the month at 8.45am – email clactonseafrontgroup@5kyourway.org or follow us on Facebook 5kyw Clacton Seafront – 5kyw Move Against Cancer
What I see in clinic
Very rarely is it just one thing.
It’s usually a combination of:
- A bit of cording
- A bit of lymphatic load
- A nervous system that’s trying to catch up
And when we work with the whole picture — gently, progressively — things tend to shift.
If your arm feels different after surgery…
that doesn’t mean something has gone wrong.
It usually means:
• your body is adapting
• your system needs support
• and you haven’t been given the full picture yet

If you’re noticing changes like this and not sure what’s normal, you’re not alone.
I support clients in Clacton-on-Sea and Bury St Edmunds (Essex & Suffolk) with:
- Manual Lymphatic Drainage
- Scar therapy
- Reflexology
- Gentle movement and rehabilitation
There are also options to move more gradually, whether that’s through 1:1 sessions, small rehab groups, WALX, or joining us at 5K Your Way in Clacton.
You don’t have to push through it or ignore it.
There are ways to work with your body.
