Why tight hips, scars, breathing and posture may all be connected.
When people hear the words pelvic floor, they often think of one thing:
“Do your pelvic floor exercises.”
But in clinic, the story is rarely that simple.
Many people I see are not just dealing with “weak muscles.” They are dealing with a body that has adapted to:
- surgery,
- stress,
- menopause,
- chronic pain,
- cancer treatment,
- scar tissue,
- breath holding,
- postural changes,
- fatigue,
- swelling,
- or years of trying to hold themselves together.
Sometimes the symptoms show up as:
- leaking,
- urgency,
- heaviness,
- pelvic pressure,
- lower back ache,
- constipation,
- painful hips,
- reduced confidence,
- or simply feeling disconnected from the body.
And often, people are surprised when we start talking about:
- breathing,
- rib movement,
- scar tissue,
- connective tissue,
- hips,
- walking,
- or posture.
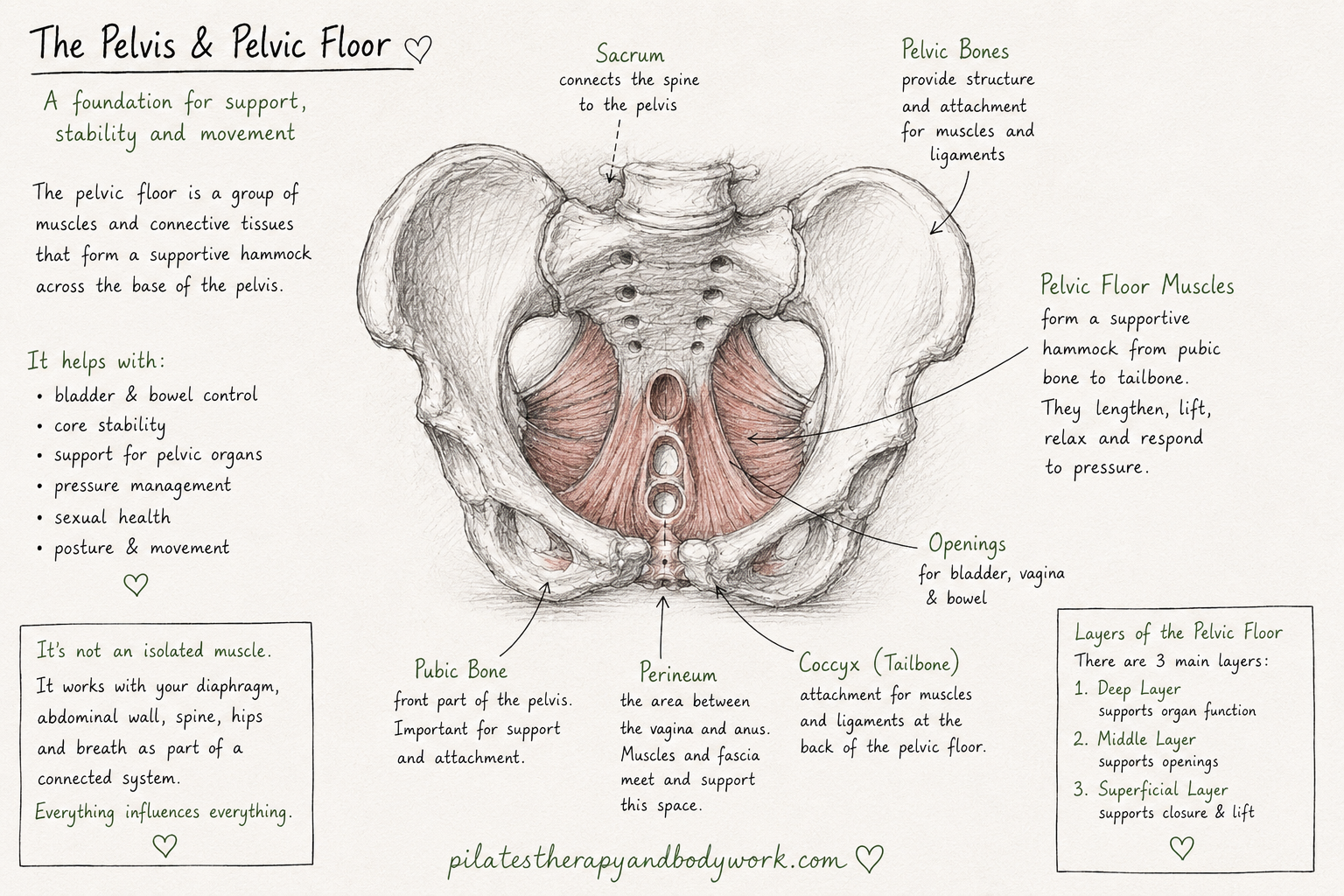
But the pelvic floor is not an isolated muscle.
It is part of a much bigger support and pressure system.
What Is The Pelvic Floor?
The pelvic floor is a group of muscles, connective tissues and supportive layers that sit at the base of the pelvis.
It helps support:
- the bladder,
- bowel,
- and reproductive organs,
while also playing an important role in:
- continence,
- pressure management,
- balance,
- breathing,
- movement,
- and load transfer through the body.
I often describe it less as a “single muscle” and more as part of a connected hammock or support system.
But even that is only part of the picture.
The pelvic floor works closely with:
- the diaphragm (your main breathing muscle),
- the abdominal wall,
- deep spinal support muscles,
- the hips and glutes,
- and the connective tissue systems that link the body together.
Research over the last decade has increasingly explored these fascial and pressure relationships, including papers looking at the continuity between the pelvic floor and lumbar (lower back) region. These studies help explain why people may experience symptoms far away from the pelvis itself.
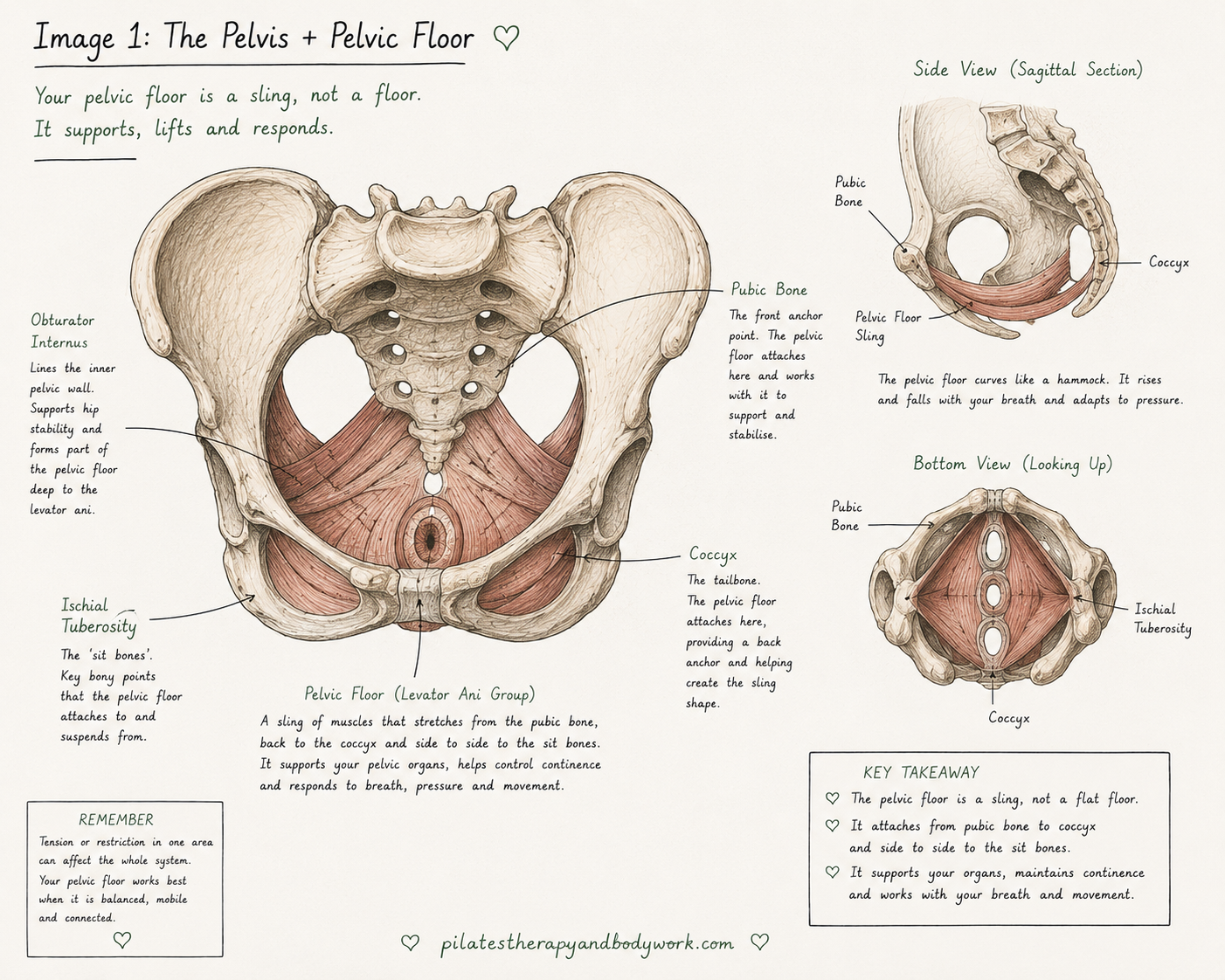
The pressure and support system
Pelvic Floor Problems Are Not Always About Weakness
This is important.
Sometimes muscles do need strengthening. Pelvic floor muscle training has strong evidence behind it for many people with urinary incontinence and pelvic organ support problems.
NICE guidelines recommend supervised pelvic floor muscle training as a first-line treatment for urinary incontinence and prolapse symptoms. Research suggests that many women improve significantly when exercises are taught correctly and practised consistently.
But not everybody has the same presentation.
Some pelvic floors are:
- underactive,
- deconditioned,
- or poorly coordinated.
Others are:
- gripping,
- overworking,
- bracing,
- or unable to relax properly.
And many people are dealing with a mixture of both.
A body that has been through:
- pain,
- surgery,
- trauma,
- stress,
- chronic coughing,
- menopause,
- or abdominal tension,
often develops protective strategies.
Breathing may become shallow.
The ribs may move less.
The abdominal wall may brace.
The hips may stiffen.
Pressure may stop moving efficiently through the body.
Over time, this can change how the pelvic floor behaves.
Tight Hips, Lower Back Tension and The Pelvic Floor
One of the most interesting areas of newer research is the growing understanding of fascial continuity.
In simple terms:
the body is not made from isolated parts.
Connective tissue links:
- hips,
- pelvis,
- lower back,
- diaphragm,
- abdominal wall,
- glutes,
- and pelvic floor.
This helps explain why somebody with:
- tight hips,
- reduced rib movement,
- altered posture,
- persistent lower back tension,
- or abdominal scarring,
may also experience pelvic floor symptoms.
It does not mean that every tight hip causes pelvic floor dysfunction.
But it does remind us that the body works as a connected system rather than separate compartments.
As movement practitioners, bodyworkers and pelvic health professionals, this matters because sometimes the answer is not simply:
“squeeze harder.”
Sometimes the body needs:
- better pressure management,
- more movement variability,
- improved breathing mechanics,
- reduced guarding,
- more confidence,
- and improved load sharing across the whole body.
Breathing matters
Breathing Matters More Than Many People Realise
The diaphragm and pelvic floor normally move together as part of a pressure system.
As we inhale:
- the diaphragm lowers,
- pressure changes through the abdomen,
- and the pelvic floor gently responds.
As we exhale:
- the system recoils and lifts.
But many things can affect this relationship:
- chronic stress,
- breath holding,
- pain,
- surgery,
- postural rigidity,
- fear of movement,
- fatigue,
- or persistent abdominal gripping.
This is one reason why many modern pelvic health approaches now include:
- breathing work,
- posture awareness,
- walking,
- movement coordination,
- and nervous system regulation alongside strengthening.
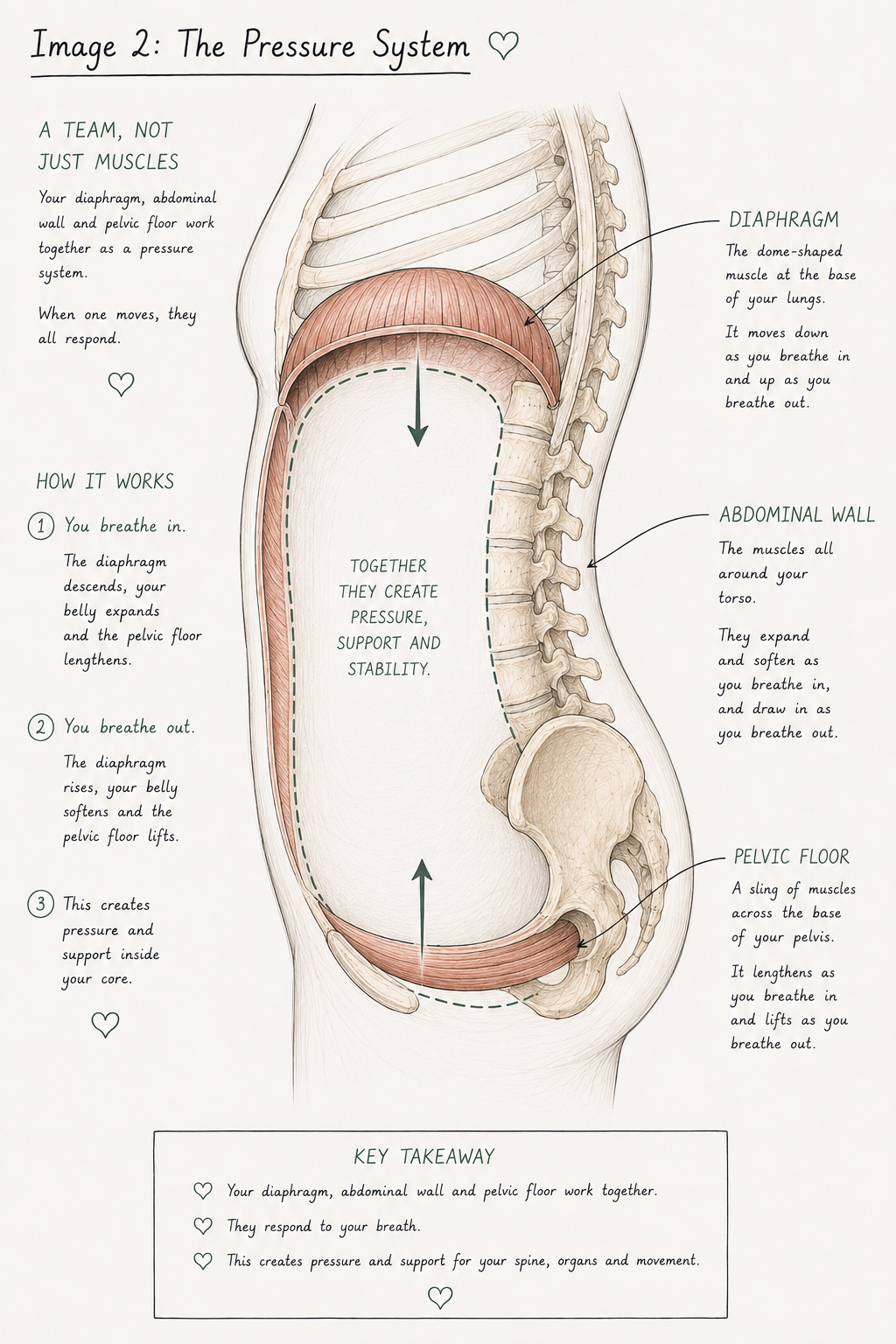
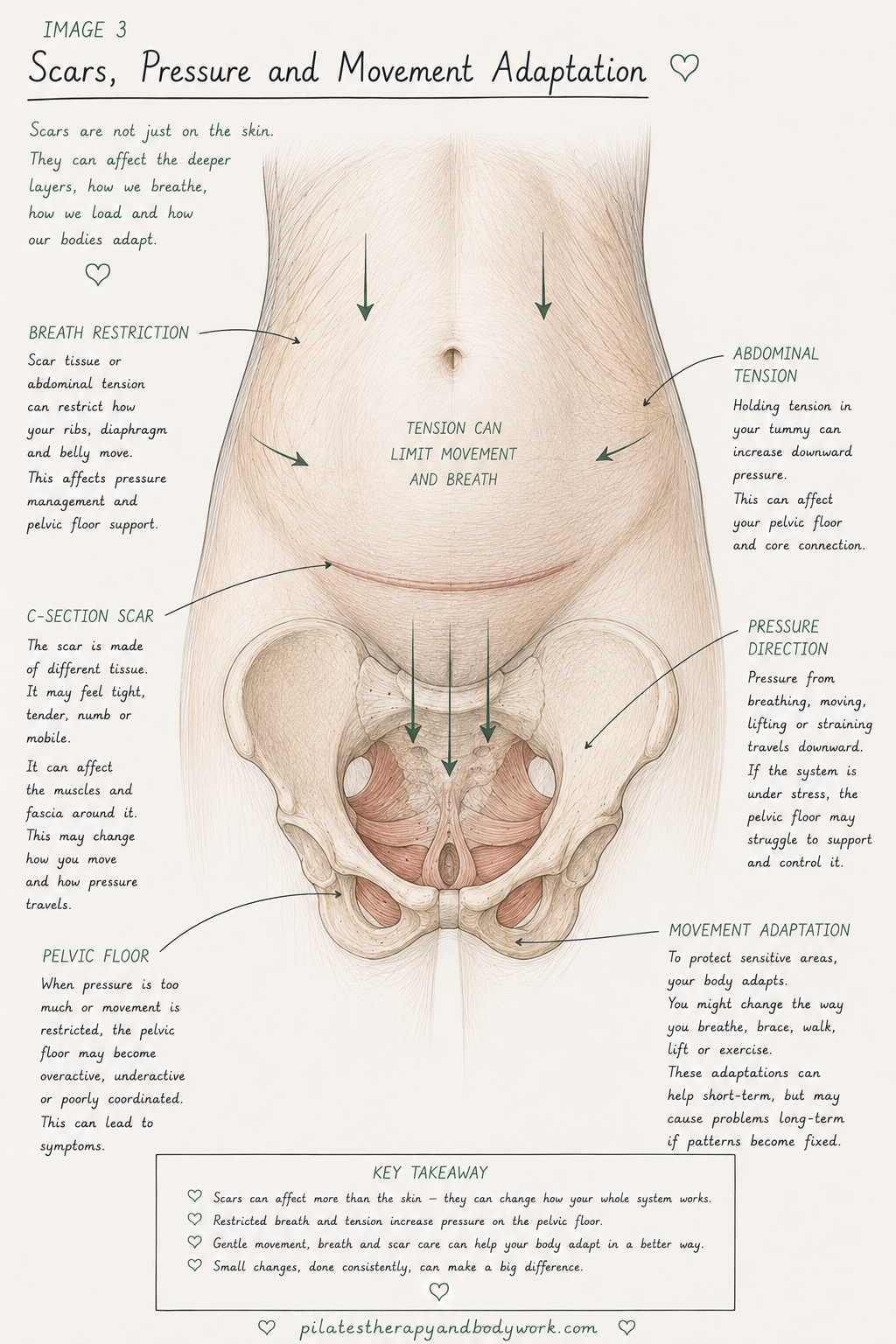
Surgery, Scar Tissue and Swelling
This is an area I feel is still not talked about enough.
After abdominal or pelvic surgery — including:
- C-sections,
- hysterectomy,
- bowel surgery,
- cancer surgery,
- prostate surgery,
- or laparoscopic procedures —
the body may temporarily change how it manages:
- pressure,
- movement,
- tension,
- and fluid balance.
Scars are a normal part of healing.
But sometimes scar tissue can feel:
- tight,
- pulling,
- numb,
- sensitive,
- thickened,
- or disconnected.
Some people also notice:
- abdominal swelling,
- feelings of heaviness,
- reduced abdominal expansion,
- or altered movement confidence.
This does not mean something has “gone wrong.”
But it may mean the body needs time, movement, support and gradual reintroduction to loading and coordination.
Following surgery, the lymphatic and connective tissue systems may also be adapting alongside the muscles themselves.
A scar might be seen in one area, but can affect other areas of the body
Find out more about scar therapy
The Numbers Matter Too
Pelvic floor symptoms are incredibly common in the UK, although many people still feel embarrassed talking about them.
Research and UK statistics suggest:
- around one in three women experience urinary incontinence,
- pelvic organ prolapse may affect up to 50% of women on examination,
- and symptoms increase with factors such as menopause, pregnancy, surgery, chronic coughing and ageing.
Men are affected too, particularly following prostate surgery and some cancer treatments.
And yet many people still assume these symptoms are:
“just part of getting older.”
They are common — but that does not mean support should be dismissed.
What Actually Helps?
This is where nuance matters.
Sometimes pelvic floor strengthening is appropriate.
Sometimes people need:
- breathing work,
- movement confidence,
- scar support,
- hip mobility,
- walking,
- glute strength,
- posture awareness,
- relaxation,
- or help reconnecting with their body after illness or surgery.
Often, it is about helping the whole system coordinate better.
Not forcing.
Not gripping harder.
Not trying to “hold everything in.”
But helping the body become more adaptable, responsive and supported again.
Gentle Support Matters
Many people avoid movement because they are frightened of:
- leaking,
- pressure,
- pain,
- prolapse,
- swelling,
- or making symptoms worse.
But avoiding movement completely can sometimes increase stiffness, deconditioning and fear.
Gentle, adaptable movement — introduced gradually and safely — can help rebuild:
- confidence,
- circulation,
- coordination,
- strength,
- posture,
- breathing patterns,
- and trust in the body again.
And sometimes, just understanding why the body feels the way it does can be hugely reassuring.
Whole Body Support
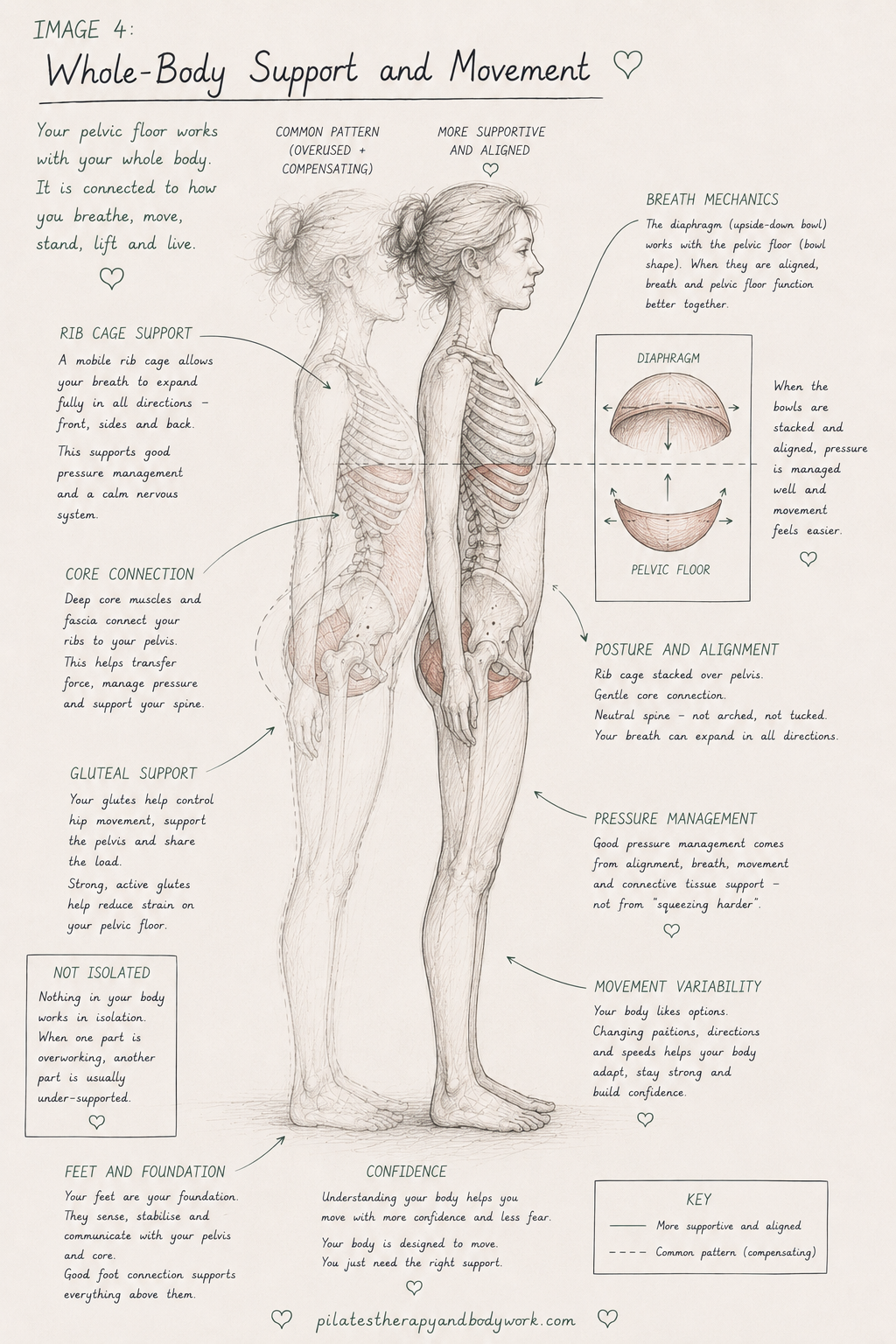
The pelvic floor is not just about squeezing muscles.
It is part of a connected, adaptable and responsive system involving:
- breathing,
- connective tissue,
- posture,
- movement,
- pressure,
- scars,
- nervous system responses,
- and confidence in the body.
Sometimes improving symptoms starts not with “doing more,” but with understanding the body differently.
Support Available
I support people with:
- pelvic health-informed movement,
- post-surgical rehabilitation,
- scar therapy,
- cancer recovery,
- Manual Lymphatic Drainage (MLD),
- gentle movement rehabilitation,
- and connective tissue-focused bodywork.
Clinics available in:
- Clacton-on-Sea,
- Bury St Edmunds,
- Essex,
- and Suffolk.
References
- NICE pelvic floor dysfunction guidance
- RCOG pelvic floor health information
- Continence Foundation resources
- Research paper: Fascial continuity of pelvic floor and lumbar region
A big shout out to my colleague- Julie Hammond
Julie and I founded Balancing the Diaphragms. Although I am very much interested with pelvic floor health, I no longer teach. Julie has taken our workshop and built on it. Julie has also written a book The Pelvic Diaphragm. If you have pelvic floor problems or are a therapist, there is something for everyone. Reading the book might give you some questions to explore with your GP, Womens Health Physio or Practitioner. I have a chapter on self-release.

Can a C-section affect the pelvic floor?
Yes — even though the baby was not delivered vaginally.
Pregnancy itself changes:
- pressure management,
- abdominal wall tension,
- breathing mechanics,
- pelvic support,
- and connective tissue loading.
Then surgery adds another layer:
- scar tissue,
- swelling,
- altered abdominal recruitment,
- guarding,
- and temporary changes in movement confidence.
This does not mean that every C-section scar causes pelvic floor problems.
But some people notice:
- pulling,
- numbness,
- abdominal weakness,
- pelvic heaviness,
- altered posture,
- or difficulty reconnecting with their core after surgery.
There is increasing recognition that pelvic floor rehabilitation after childbirth should include more than isolated exercises alone. NICE guidelines support supervised pelvic floor muscle training and wider pelvic health education following pregnancy and birth.
Sometimes the body simply needs:
- time,
- movement,
- reassurance,
- gradual loading,
- and support reconnecting different areas again.
Can medications affect the pelvic floor or bladder?
Sometimes, yes.
Certain medications may influence:
- bladder urgency,
- constipation,
- tissue hydration,
- muscle tone,
- or bowel function.
Examples can include:
- diuretics,
- some antidepressants,
- antihistamines,
- opioid pain medication,
- some hormone-related medications,
- and treatments affecting fluid balance or nervous system signalling.
Constipation is particularly important because repeated straining can increase downward pressure through the pelvic floor over time.
This is one reason pelvic health conversations should never be reduced to:
“just do exercises.”
The wider picture matters too.
If symptoms suddenly change after starting medication, it is always worth discussing this with a GP, pharmacist or specialist healthcare professional.
Can hip problems affect the pelvic floor?
Absolutely — and this is something I see regularly.
The hips, glutes, pelvis and pelvic floor are designed to work together during:
- walking,
- balance,
- lifting,
- breathing,
- and load transfer.
When somebody has:
- hip arthritis,
- pain,
- reduced mobility,
- stiffness,
- glute weakness,
- or altered gait patterns,
the body often adapts movement strategies.
Over time, this can influence:
- pelvic positioning,
- breathing,
- abdominal tension,
- and pressure distribution.
Research exploring fascial continuity and pressure systems supports the idea that the pelvis does not work in isolation from surrounding structures.
Clinically, this is why some people improve not only with pelvic floor work, but also with:
- walking,
- hip strengthening,
- balance work,
- breathing practice,
- and improving movement confidence.
Can cancer treatment affect the pelvic floor?
Yes — and I think this is still not spoken about enough.
Cancer treatment may affect:
- connective tissue,
- fatigue levels,
- hormone status,
- abdominal pressure systems,
- scar tissue,
- swelling,
- bowel and bladder function,
- and movement confidence.
Pelvic floor symptoms may appear after:
- prostate cancer treatment,
- hysterectomy,
- bowel surgery,
- abdominal surgery,
- radiation therapy,
- medically-induced menopause,
- or periods of inactivity and deconditioning during treatment.
Some people also experience:
- abdominal swelling,
- lymphatic congestion,
- scar tightness,
- altered breathing patterns,
- or fear of movement afterwards.
This does not mean people should avoid activity.
In fact, appropriately adapted movement often helps rebuild:
- confidence,
- circulation,
- coordination,
- breathing,
- posture,
- and body trust again.
Sometimes the first step is simply helping somebody understand:
“Your body has adapted to a lot.”
Does age affect the pelvic floor?
Ageing affects all tissues in the body — not just the pelvic floor.
Muscles, connective tissue, recovery capacity and tissue elasticity naturally change over time.
But pelvic floor symptoms should not simply be dismissed as:
“just part of getting older.”
Many people improve significantly with:
- education,
- movement,
- strength work,
- breathing,
- pelvic floor training,
- lifestyle changes,
- and appropriate support.
NICE recommends pelvic floor muscle training throughout life because long-term training may help prevent or reduce symptoms.
The important thing is that support should adapt to the individual person, their history and their current life stage — not just focus on isolated exercises alone.
