
Why early understanding matters — and why it’s rarely just one thing
This is something that’s been on my mind more and more as I go deeper into my Vodder MLD training. (If I wake up at 3am, it’s usually worth popping my thoughts on paper!)
Because lip(o)edema isn’t just “a bit of fat” and it isn’t just “swelling”.
It’s often:
-
pain
-
heaviness
-
bruising
-
tenderness
-
body-confidence being quietly eroded
-
and years of being told to “just try harder”
And there’s also growing discussion around lip(o)edema being linked with connective tissue differences — which matters, because connective tissue is the environment your blood vessels and lymphatics live in.
What is lip(o)edema, in normal language?
Lip(o)edema is a long-term condition where there’s disproportionate fat and tissue change (most commonly legs, sometimes arms), often with:
-
pain or tenderness
-
easy bruising
-
heaviness
-
and a very specific “this doesn’t behave like ordinary weight gain” feel
It’s increasingly described as a distinct disease process rather than simply lifestyle-related weight gain.
Some emerging research has also noted overlap between lip(o)edema and hypermobility spectrum disorders — again pointing towards connective tissue behaving differently, which may influence fluid regulation and symptom presentation.
You can read more about Lipoedema research here: Article
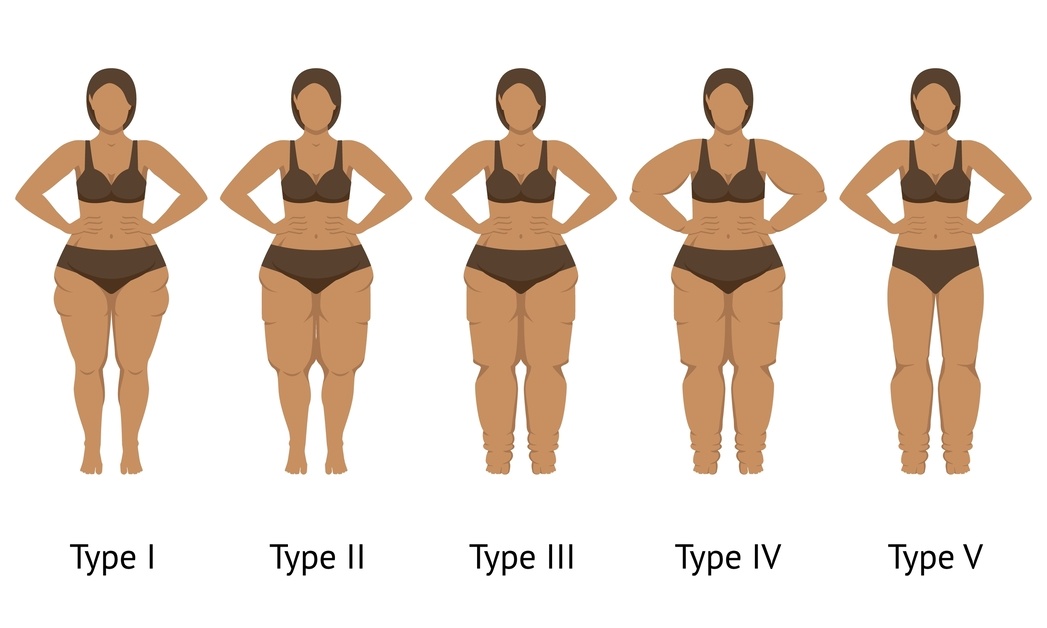
When does lip(o)edema usually begin or change?
One of the patterns often talked about in lip(o)edema is that symptoms tend to appear — or noticeably worsen — at certain points in life.
These often include:
-
Puberty
-
Pregnancy
-
Perimenopause or menopause
-
Sometimes after gynaecological surgery or hormonal change
In many cases, people describe:
-
legs or arms becoming more tender
-
a feeling of heaviness
-
tissue that bruises more easily
-
or changes in shape that don’t seem to respond to diet or exercise
Because these changes can happen around the same time as natural hormonal shifts, they are sometimes dismissed as:
“just weight gain”
“fluid retention”
“getting older”
But for some, this may be the point at which lip(o)edema begins to develop — or when previously manageable symptoms become more noticeable.
Understanding when symptoms first appeared can sometimes help clinicians distinguish between:
-
typical weight-related change
-
lymphatic swelling
-
or tissue changes associated with lip(o)edema
which may influence what kind of support is most helpful going forward.
Where do connective tissue and lymphatics come in?
Your lymphatic system sits within your connective tissue network.
The very small lymphatic capillaries rely on:
-
surrounding tissue tension
-
anchoring filaments
-
and pressure changes in the tissue space
to open and collect fluid.
They don’t have a strong muscular wall like arteries do.
Instead, they are supported by the connective tissue around them.
So if connective tissue behaves differently (as it may in some hypermobility-spectrum presentations), this may influence:
-
tissue elasticity
-
vessel support
-
pressure relationships in the interstitial space
-
and possibly how fluid moves or settles within tissues
For some people, it’s not:
“Why are my legs bigger?”
It’s:
“Why does my tissue behave differently?”
Where do connective tissue and lymphatics come in?
Your lymphatic system sits within your connective tissue network.
The very small lymphatic capillaries rely on:
-
surrounding tissue tension
-
anchoring filaments
-
and pressure changes in the tissue space
to open and collect fluid.
They don’t have a strong muscular wall like arteries do.
Instead, they are supported by the connective tissue around them.
So if connective tissue behaves differently (as it may in some hypermobility-spectrum presentations), this may influence:
-
tissue elasticity
-
vessel support
-
pressure relationships in the interstitial space
-
and possibly how fluid moves or settles within tissues
For some people, it’s not:
“Why are my legs bigger?”
It’s:
“Why does my tissue behave differently?”
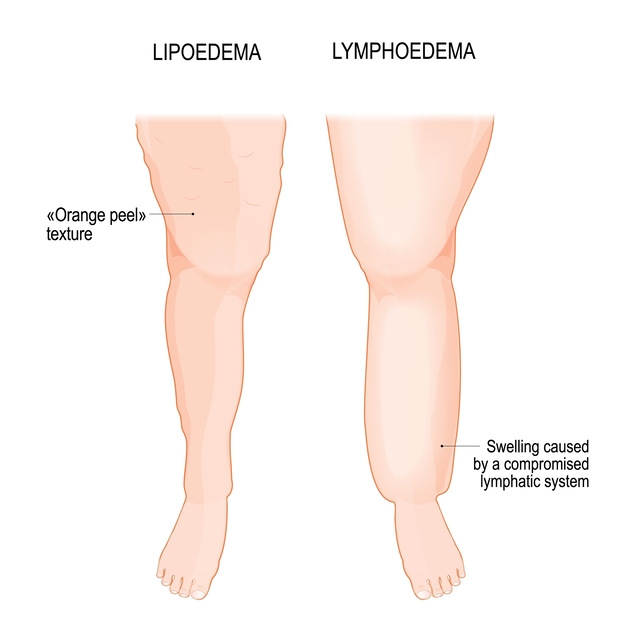
Lip(o)edema vs Lymphoedema — what’s the difference?
These two conditions are sometimes confused because both can involve:
-
heaviness
-
changes in limb shape
-
discomfort
-
or swelling-type symptoms
But they are not the same.
Lip(o)edema:
-
involves disproportionate fat and connective tissue change
-
is often painful or tender
-
bruises easily
-
usually affects both legs (and sometimes arms)
-
often spares the hands and feet
-
tends to be fairly symmetrical
Lymphoedema:
-
is caused by reduced lymphatic transport capacity
-
may affect one limb more than another
-
can involve pitting in earlier stages
-
may affect hands or feet
-
and often develops after surgery, radiotherapy, trauma or infection
Over time, some people with lip(o)edema may develop a secondary lymphatic component — sometimes referred to as lipo-lymphoedema.
Which is why assessment can be helpful if symptoms change.
What does early intervention actually mean?
Early intervention doesn’t mean:
doing everything perfectly
or having a strict regime
It often means:
-
getting a proper assessment
-
understanding what you’re dealing with
-
learning what helps your pain or heaviness
-
building a plan you can actually live with
International consensus statements now support conservative management as a package, including:
-
compression (where appropriate)
-
skin care
-
education and self-management
-
and psychological support where needed
Which is multidisciplinary by definition.
Where does MLD fit?
This is the bit I’ll say carefully and honestly.
MLD is often used within lymphatic care pathways — particularly where a secondary lymphatic component is present.
But it tends to work best as part of a wider plan rather than as a standalone “fix”.
My clinical bias (and it’s a bias, not a promise) is:
MLD can be a supportive piece for some people — especially when it’s paired with:
-
education
-
compression where appropriate
-
pacing
-
and movement that supports fluid exchange
If someone is being sold MLD as a miracle cure while everything else is ignored…
that’s usually a red flag.
A short note on cancer recovery
Lip(o)edema itself is not caused by cancer treatment.
However, the times in life when lip(o)edema tends to appear or progress — such as puberty, pregnancy or menopause — are hormonally driven.
For those living with and beyond cancer, especially where treatment overlaps with menopause or endocrine therapy, it can sometimes be difficult to work out what’s driving symptoms like heaviness, tenderness or limb change.
Understanding that connective tissue and fat distribution may also be part of the picture can help guide more appropriate support — particularly when planning movement, exercise or conservative management.
Not all heaviness is lymphoedema — but changes are worth checking.
