
Can Breathing Help Your Lymphatic System?
Posture, Stress and Swelling Explained
Over the last few years, working with people recovering from surgery, cancer treatment and persistent swelling, I’ve noticed something that often gets overlooked.
Breathing matters.
Not just for oxygen, but for how the body moves fluid.
Because when you look closely at the lymphatic system, you realise something quite interesting:
Breathing is one of the body’s natural lymph pumps.
And yet very few people are ever told that.
The Lymphatic System Has No Pump
Most people know the heart pumps blood around the body.
The lymphatic system works differently.
It has no central pump.
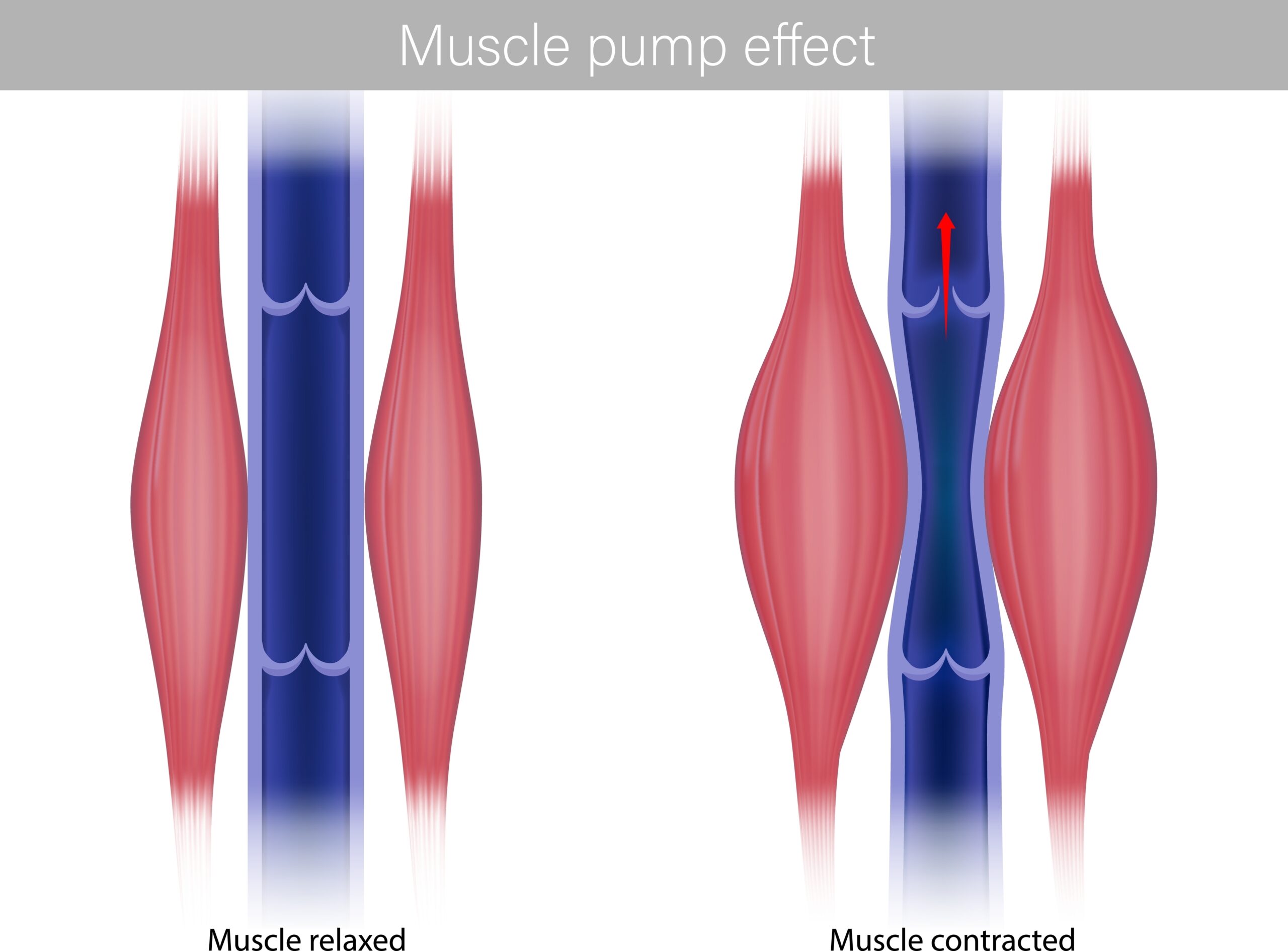
Instead, lymph relies on movement to travel through the body. This includes:
-
muscle contractions
-
joint movement
-
pressure changes inside the body
-
breathing
These pressure changes help push lymph through the lymphatic vessels and towards the venous circulation.
Research describing lymphatic physiology explains that respiratory pressure changes are one of the key mechanisms helping lymph move through the thoracic duct, the largest lymph vessel in the body.
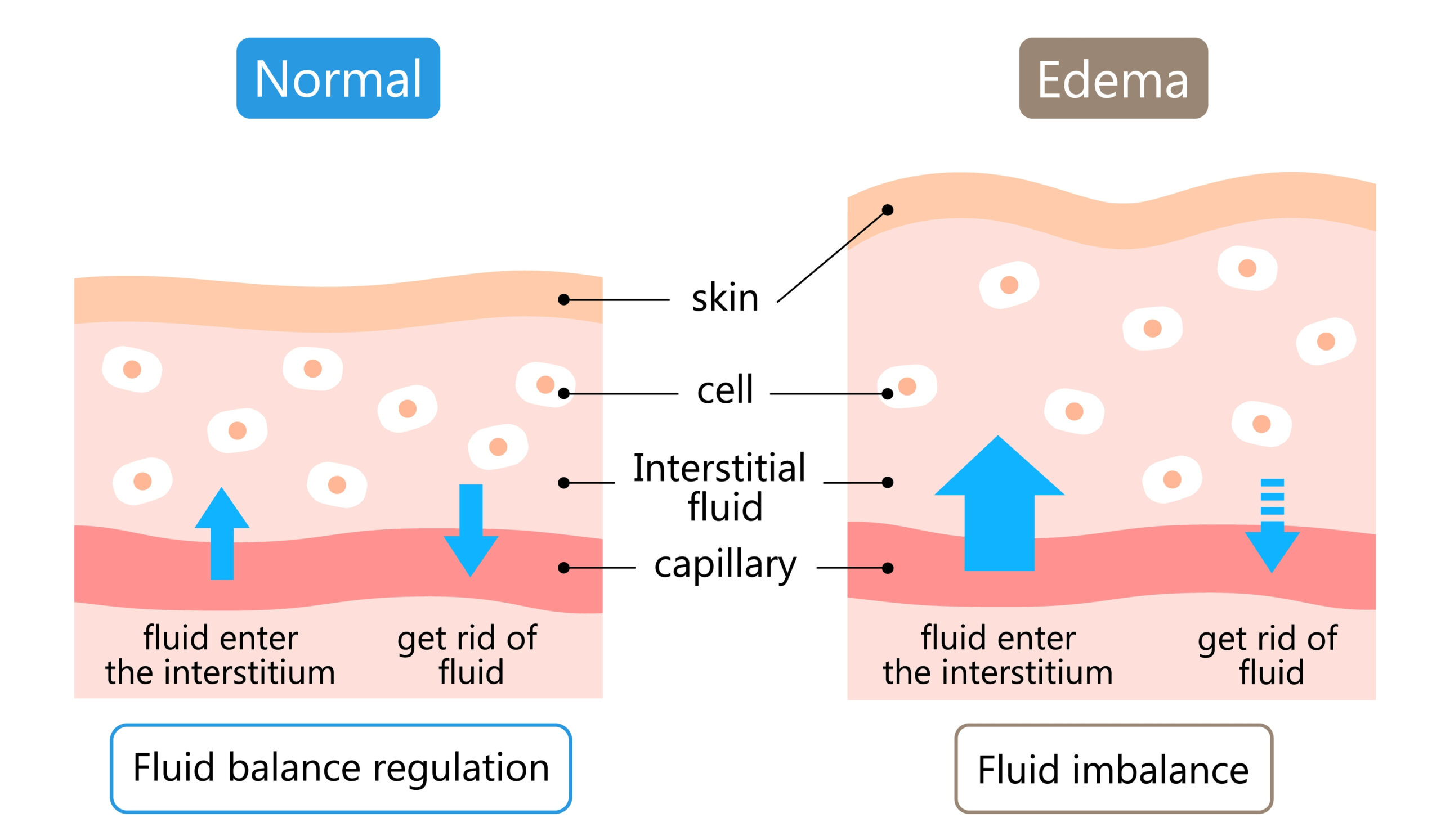
Without movement — after surgery, illness or long periods of sitting — lymph flow can slow down. You can read more about swelling here
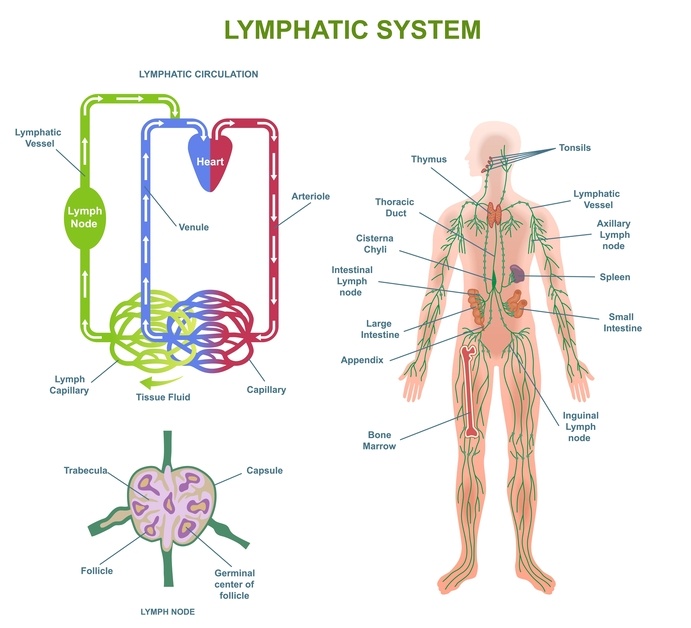
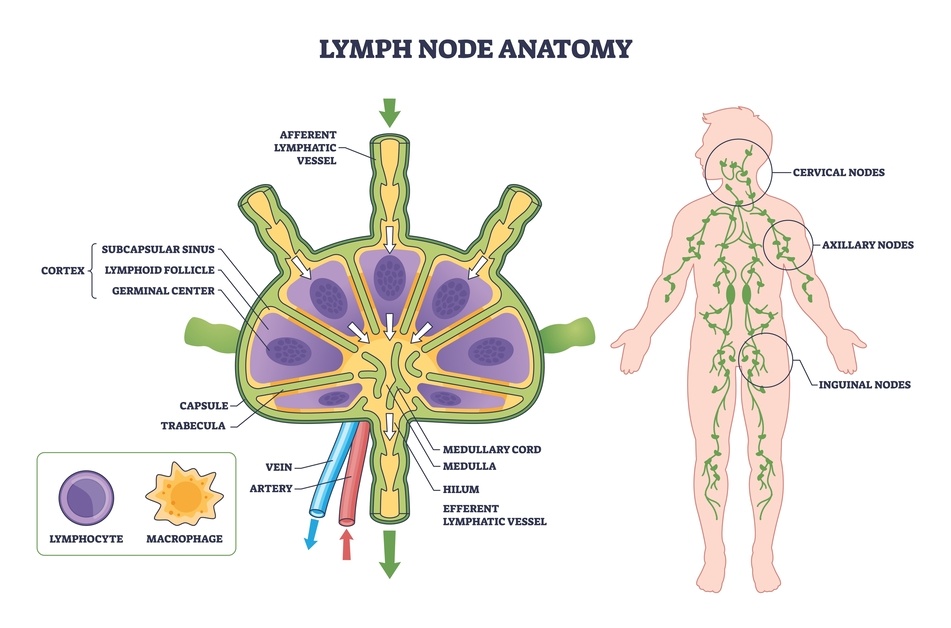
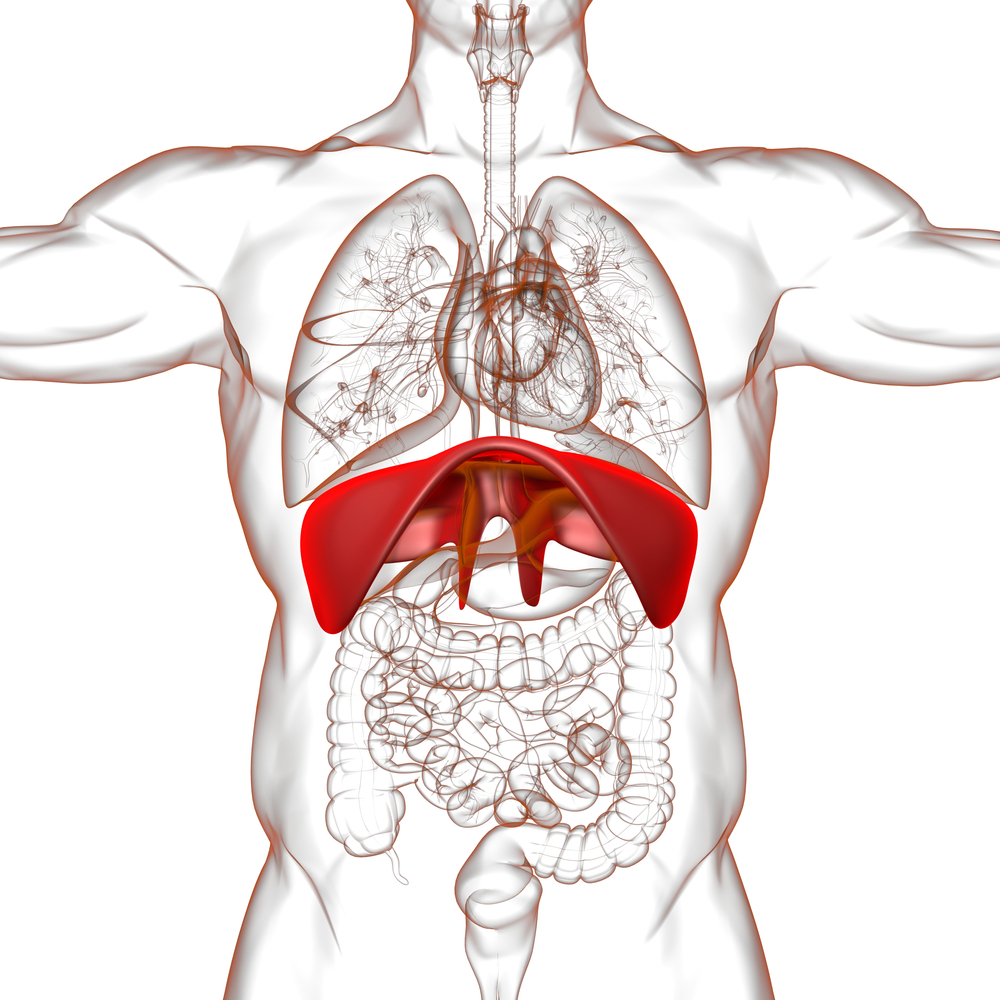
The Diaphragm: Your Built-In Fluid Pump
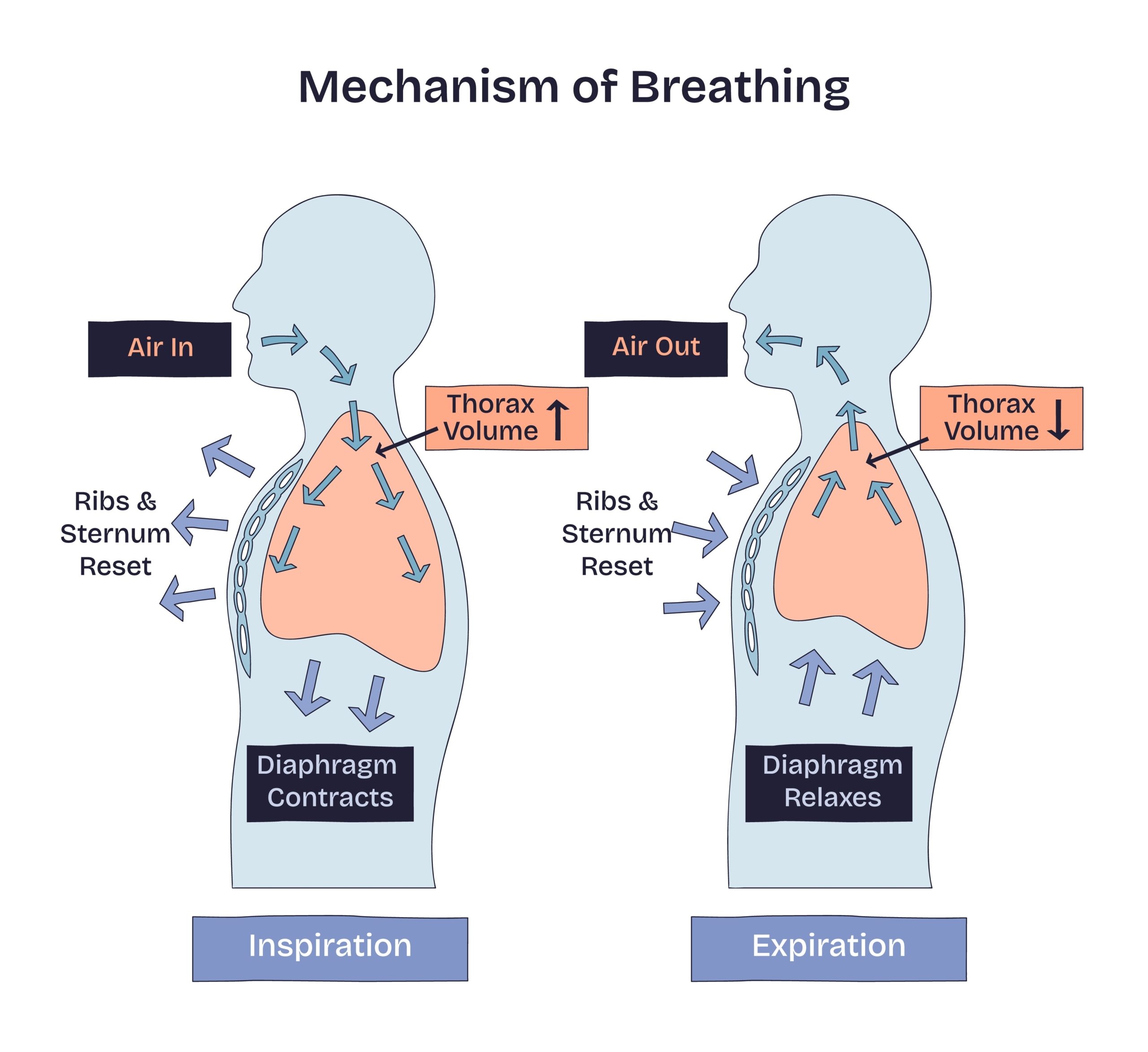
The diaphragm is the large dome-shaped muscle underneath the lungs.
When you breathe in:
• the diaphragm moves downward
• pressure inside the chest decreases
• pressure inside the abdomen increases
These pressure changes help draw lymph upward through the thoracic duct.
This mechanism is sometimes called the thoraco-abdominal pump.
Each breath gently helps move fluid through the lymphatic system.
Scientific studies on lymph transport confirm that respiration plays an important role in driving lymph flow through major lymphatic vessels.
Dysfunctional Breathing Is Surprisingly Common
Breathing is automatic, but that doesn’t mean it always works well.
Research suggests around 9–12% of adults may experience dysfunctional breathing patterns, even when there is no lung disease present.
That means millions of people may be breathing in ways that are less efficient for the body.
Dysfunctional breathing can include:
-
chest breathing rather than diaphragmatic breathing
-
shallow or rapid breathing
-
mouth breathing
-
frequent sighing or air hunger
Clinical research describes breathing pattern disorders as changes in breathing behaviour that cause symptoms such as breathlessness, dizziness or fatigue despite normal lung function.
Stress and Anxiety Change the Way We Breathe
Breathing is closely linked to the nervous system.
When the body is under stress, breathing naturally becomes:
-
faster
-
shallower
-
higher in the chest
This is part of the normal fight-or-flight response.
The problem is that many people now live with long-term stress, meaning breathing patterns never fully settle back down.
Research into breathing pattern disorders shows a strong relationship between anxiety, hyperventilation and dysfunctional breathing.
Over time this can contribute to muscle tension, fatigue and altered breathing mechanics.
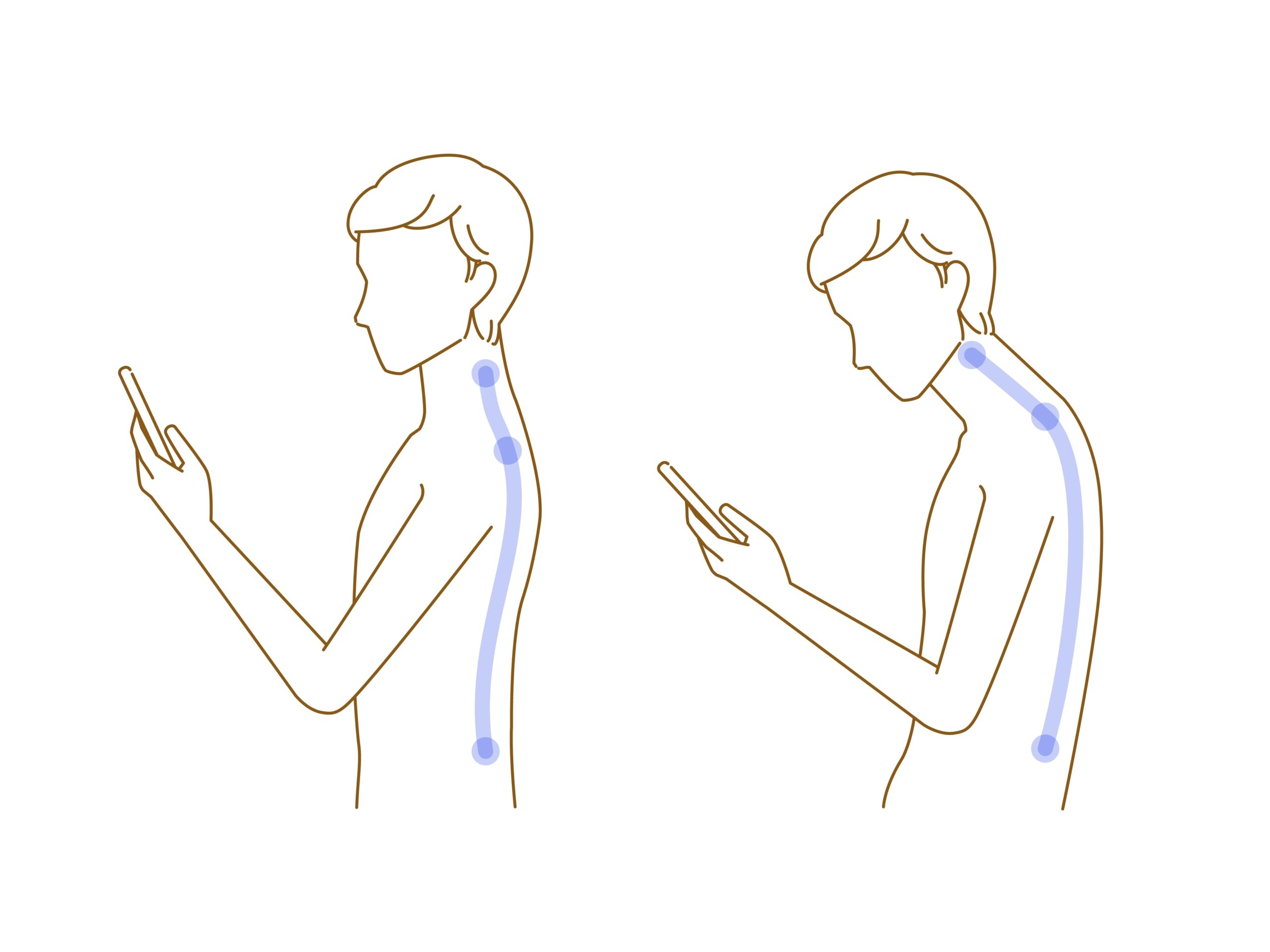
Modern Posture Is Quietly Changing Breathing
Posture is another important piece of the puzzle.
Modern life encourages us to spend long periods sitting, often leaning forward towards screens or looking down at phones.
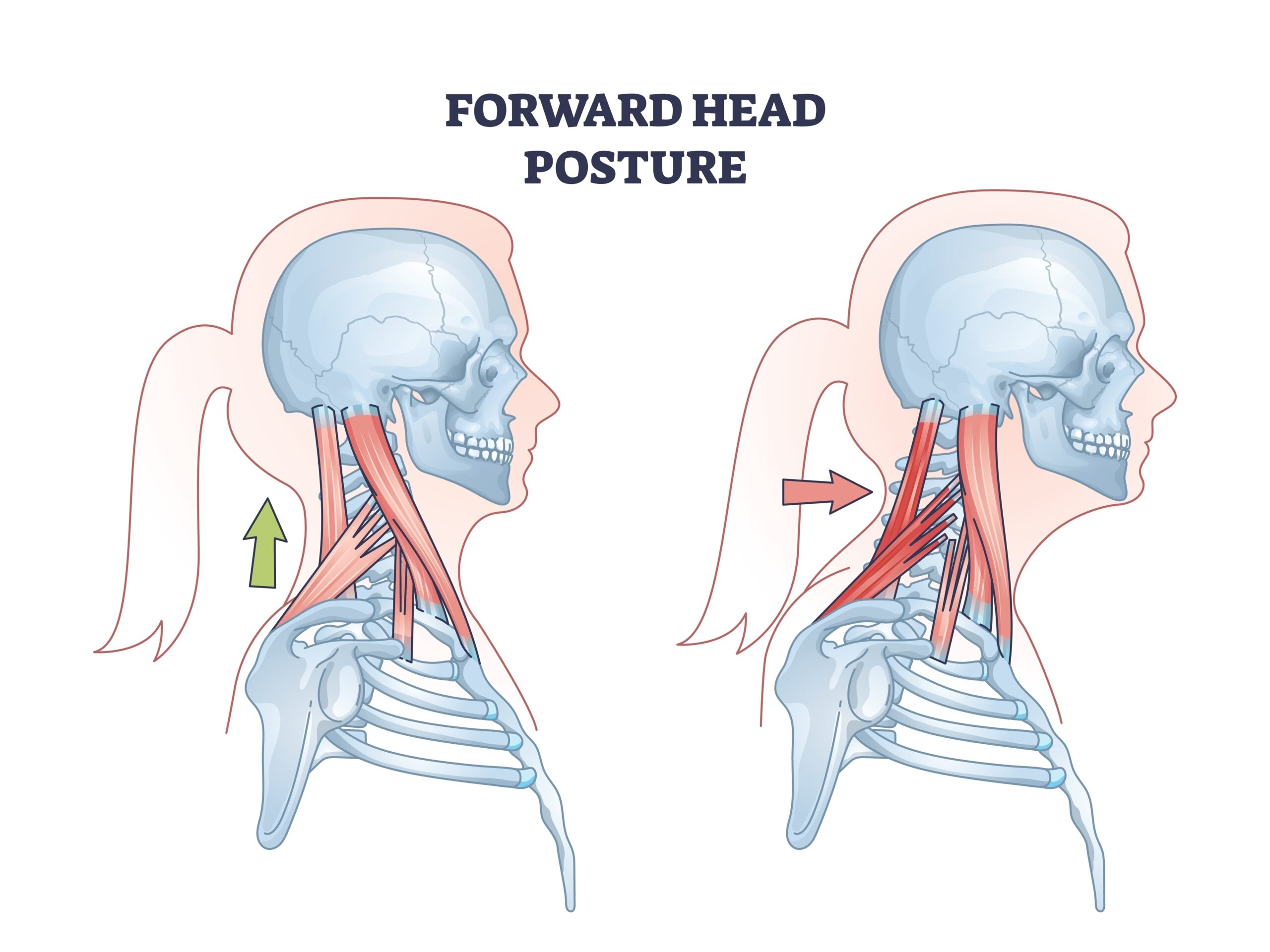
This can lead to forward head posture.
Research investigating forward head posture shows it can:
-
reduce respiratory efficiency
-
restrict lower rib cage movement
-
increase reliance on neck and shoulder muscles for breathing
When this happens the diaphragm becomes less active and breathing shifts towards the upper chest.
Studies examining posture and respiratory function confirm that forward head posture is associated with reduced diaphragm efficiency and altered breathing patterns.
Surgery Can Also Change Breathing Patterns
Another time breathing patterns often change is after surgery.
Pain, fatigue and protective muscle guarding can lead people to breathe more shallowly.
This is particularly common after:
-
abdominal surgery
-
breast surgery
-
cancer treatment
Reduced movement of the diaphragm can influence circulation and fluid movement.
Emerging research is beginning to explore how diaphragmatic breathing combined with movement exercises may improve outcomes in lymphoedema rehabilitation following cancer surgery.
If you are preparing for surgery you may find my recent blog helpful


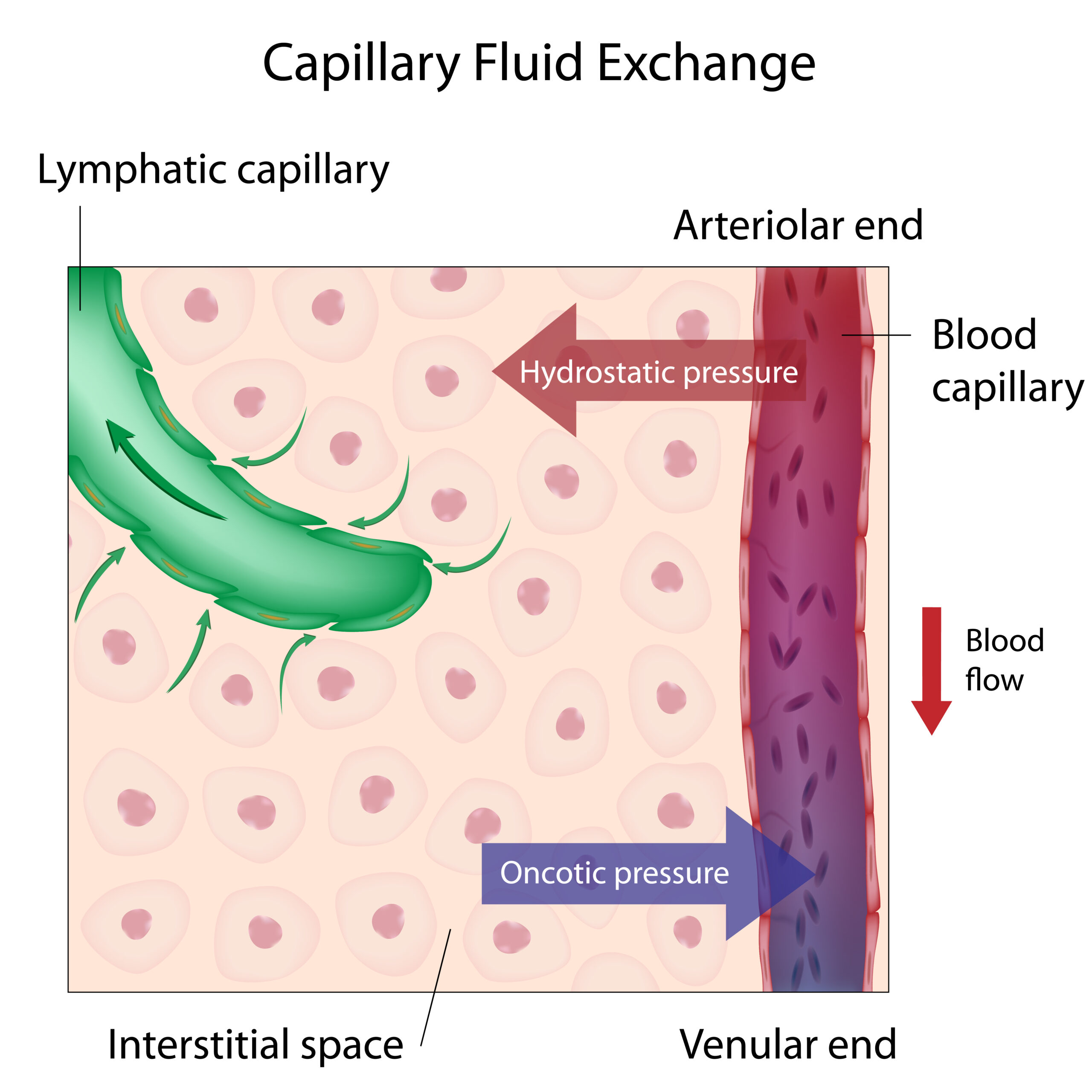
The Body Works as a Pressure System
One way to understand this is to think about the body as a pressure system.
Breathing changes pressure inside the thoracic and abdominal cavities.
These pressure shifts influence:
-
venous return
-
lymph flow
-
organ movement
-
connective tissue tension
Because lymph vessels sit within the connective tissue network, these pressure changes help encourage fluid movement.
When breathing becomes shallow or restricted, this natural pump becomes less effective.
When breathing slows and the diaphragm moves freely again, the system begins working more efficiently.
A Simple Breathing Practice
You don’t need complicated exercises to support breathing.
Try this simple practice:
-
Sit or lie comfortably.
-
Place one hand on your chest and one on your abdomen.
-
Breathe slowly through your nose.
-
Allow your abdomen to gently expand.
-
Exhale slowly and allow your shoulders to relax.
Aim for 5–10 slow breaths.
Many people notice their breathing becomes calmer and their shoulders begin to drop.
Small changes like this can help restore the natural rhythm between breathing, movement and fluid flow.
A Simple Thought That Often Helps My Clients
Sometimes I explain it like this:
“Your lymphatic system doesn’t have a pump like the heart. It relies on movement and pressure changes. Breathing is one of the things that creates those pressure changes.”
When people understand that, they often start to see their breathing differently.
The Bigger Picture
Breathing isn’t a treatment on its own.
But it can be a powerful support tool alongside:
-
compression therapy
-
rehabilitation exercise
Sometimes the simplest things in the body turn out to be the most important.
Breathing is something we do thousands of times every day.
Learning to do it well again can make a surprising difference.
