
Why Is My Swelling Worse at the End of the Day?
(And what your lymphatic system might be trying to tell you)
Many people notice a pattern with swelling.
In the morning things feel fairly normal.
By late afternoon your rings feel tighter, your legs feel heavier, or your arm feels more swollen than it did earlier in the day.
It’s incredibly common. And for many people it can be worrying.
So let’s look at what might actually be happening inside the body.
Because most of the time, it isn’t random.
Your body is dealing with fluid, gravity, fatigue and the workload of the lymphatic system.
Gravity quietly works against us all day
During the day we spend a lot of time upright.
That means gravity is constantly pulling fluid downwards through the body.
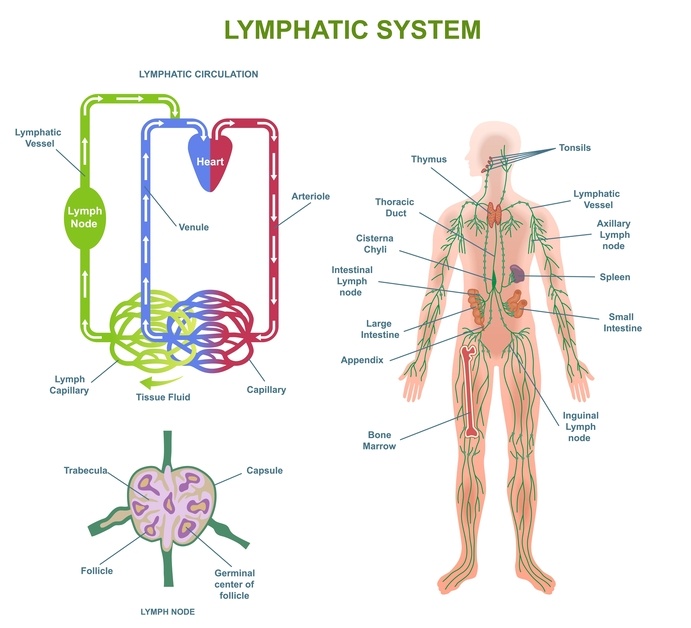
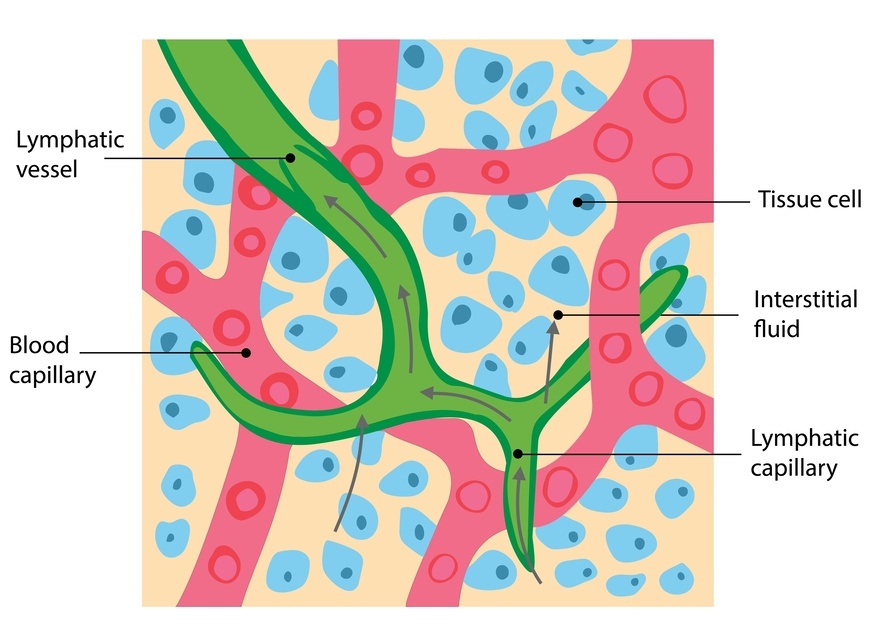
Your circulation system is designed to manage this. Blood vessels push fluid out into tissues to nourish cells, and the lymphatic system helps collect excess fluid and return it back into circulation.
But by the end of the day that system has simply been working for hours.
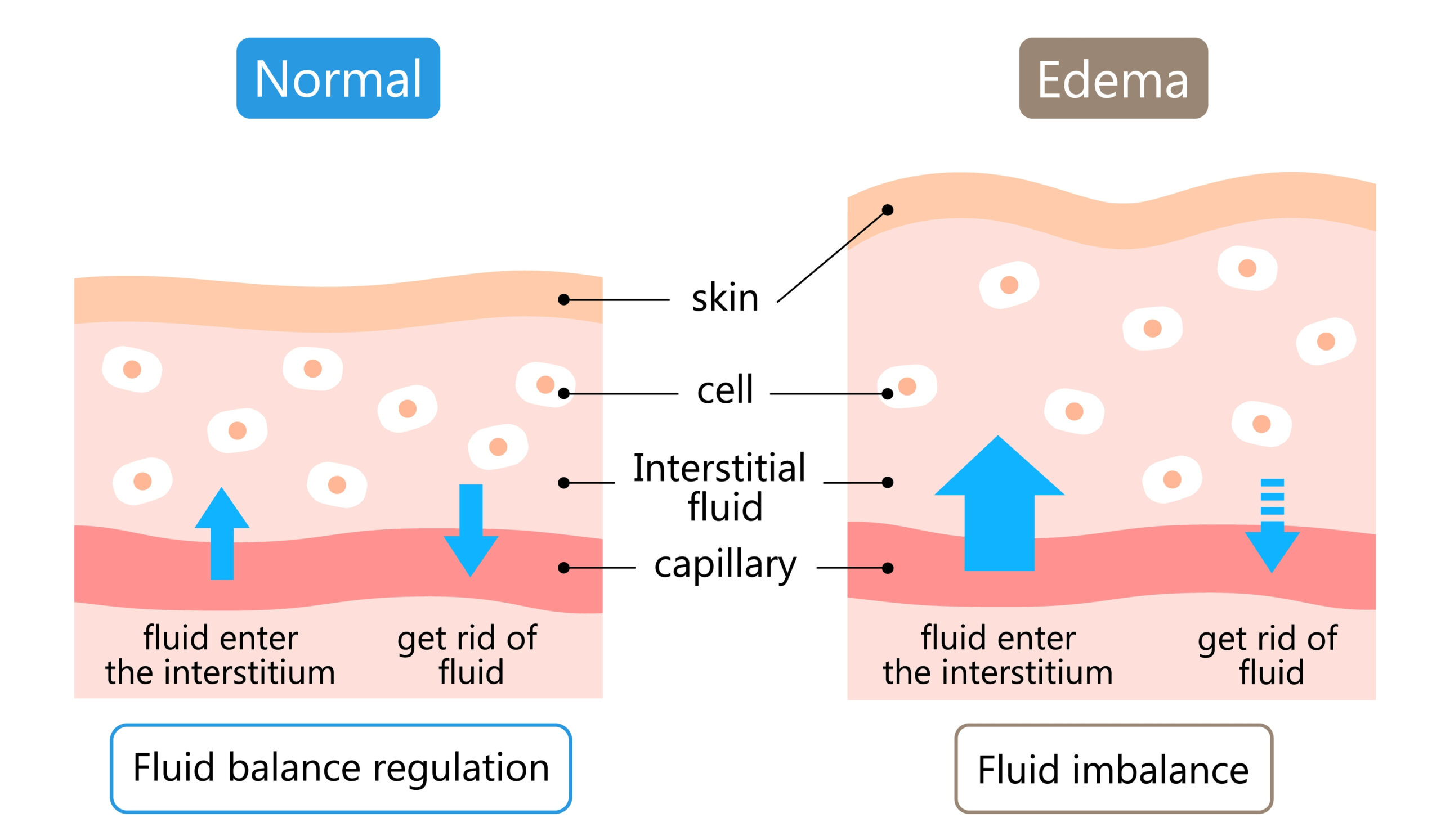
If lymphatic transport is reduced — because of surgery, inflammation, hormonal changes, injury, inactivity or simply the natural ageing process — fluid can slowly accumulate.
Research suggests that up to 20–30% of women treated for breast cancer will develop some level of lymphoedemaduring their lifetime (DiSipio et al., 2013).
For these individuals the system already has less transport capacity, so daily fluid shifts can become more noticeable.
You can find more information here:
Cancer Research UK lymphoedema information
You might experience this as:
• rings becoming tight
• socks leaving marks
• a feeling of heaviness in an arm or leg
• shoes feeling tighter in the evening
The lymphatic system gets tired too
This is something that is rarely explained clearly.
Your lymphatic system doesn’t have a central pump like the heart.
Instead it relies on:
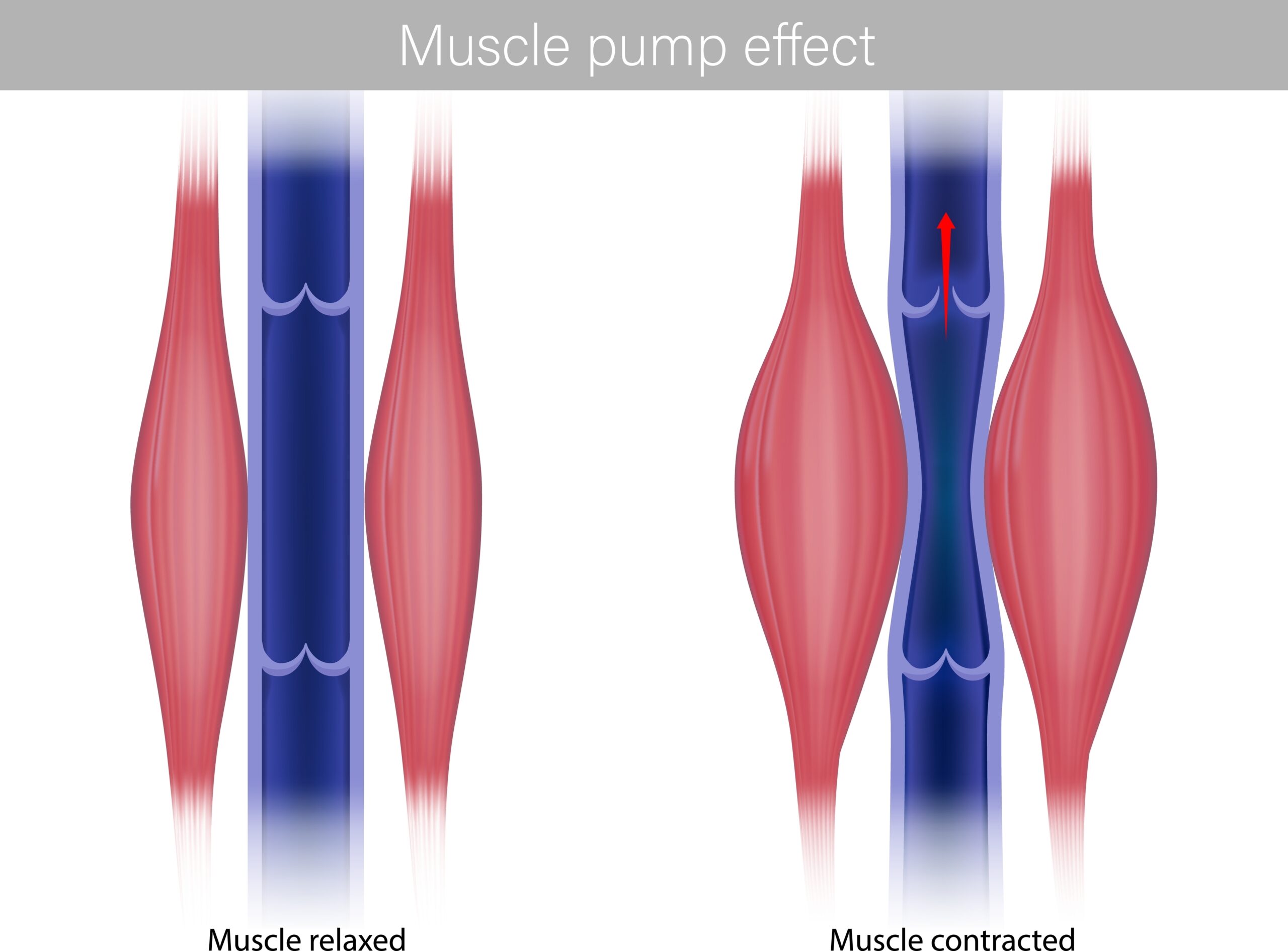
• muscle movement
• breathing pressure changes
• vessel contractions
• connective tissue movement
• joint motion
This means your daily activity patterns matter enormously.
If you’ve had a long day sitting, standing, travelling, or working at a desk, lymphatic flow may simply be slower by the end of the day.
Interestingly, research has shown that gentle movement significantly improves lymphatic flow, because muscle contraction and tissue movement help propel lymph through the vessels (Mortimer & Rockson, 2014).
This is why small habits like walking, stretching or breathing exercises can make such a difference.
Connective tissue plays a bigger role than people realise
This is where my fascial and lymphatic worlds collide a little.
Fluid doesn’t just sit in empty space. It sits within connective tissue.
When tissue becomes stiff, inflamed or fibrotic, it can hold on to fluid more easily.
Over time this can create a cycle where:
protein-rich lymph fluid attracts water →
inflammation increases →
fibroblasts produce more collagen →
tissue becomes stiffer →
fluid drainage becomes more difficult.
This process is well recognised in lymphoedema research, where progressive fibrosis is one of the reasons swelling can become harder to manage over time (Rockson, 2018).
The earlier the lymphatic system is supported, the better.
Fatigue, stress and the nervous system
Another piece of the puzzle is the nervous system.
Many people notice swelling is worse when they are:
• tired
• stressed
• run down
• recovering from illness.
There is increasing research exploring the connection between the autonomic nervous system and lymphatic function.
The lymphatic vessels contain smooth muscle that is partly regulated by nervous system activity. When the body is under prolonged stress, circulation patterns and fluid regulation can shift (Choe et al., 2015).
This is why rest, breathing and pacing activities can sometimes reduce swelling more effectively than pushing through fatigue.
Posture and breathing affect fluid movement
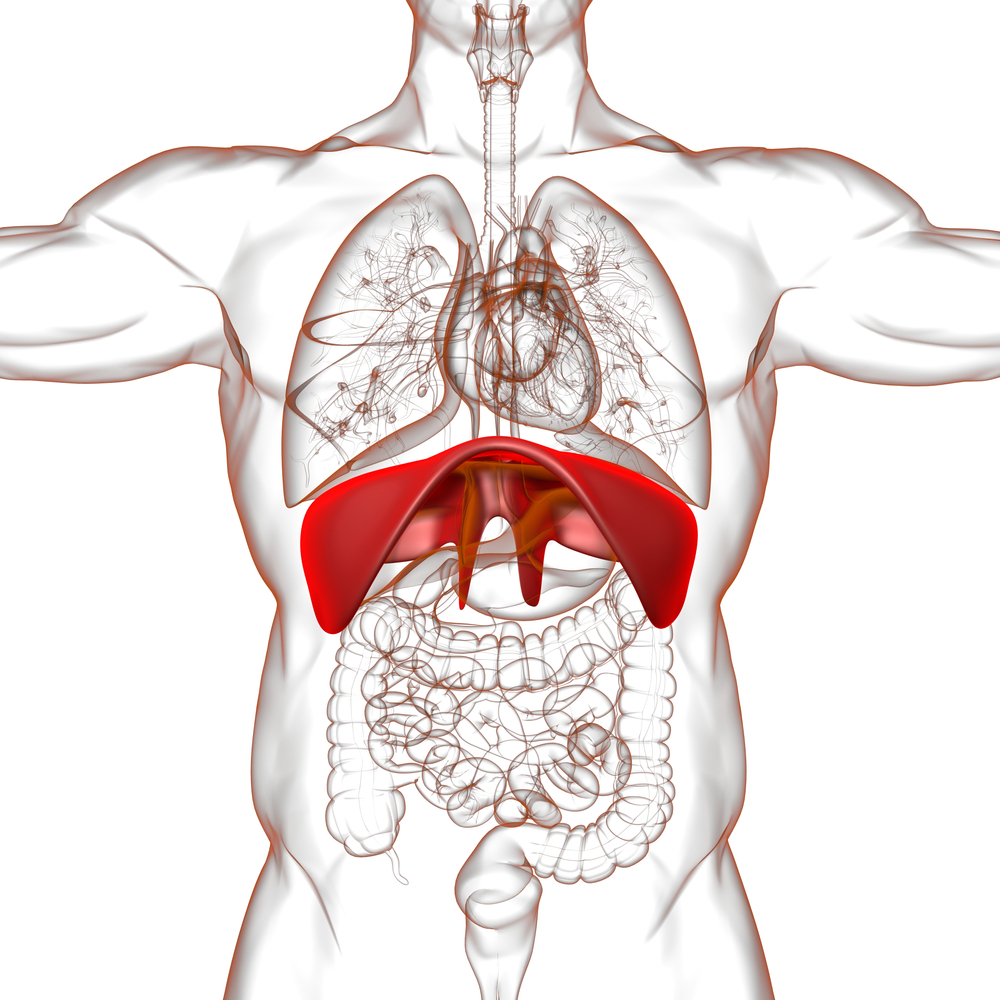
Your diaphragm is one of the most powerful pumps in the lymphatic system.
Every breath creates pressure changes that help move lymph through the thoracic duct and major lymphatic pathways.
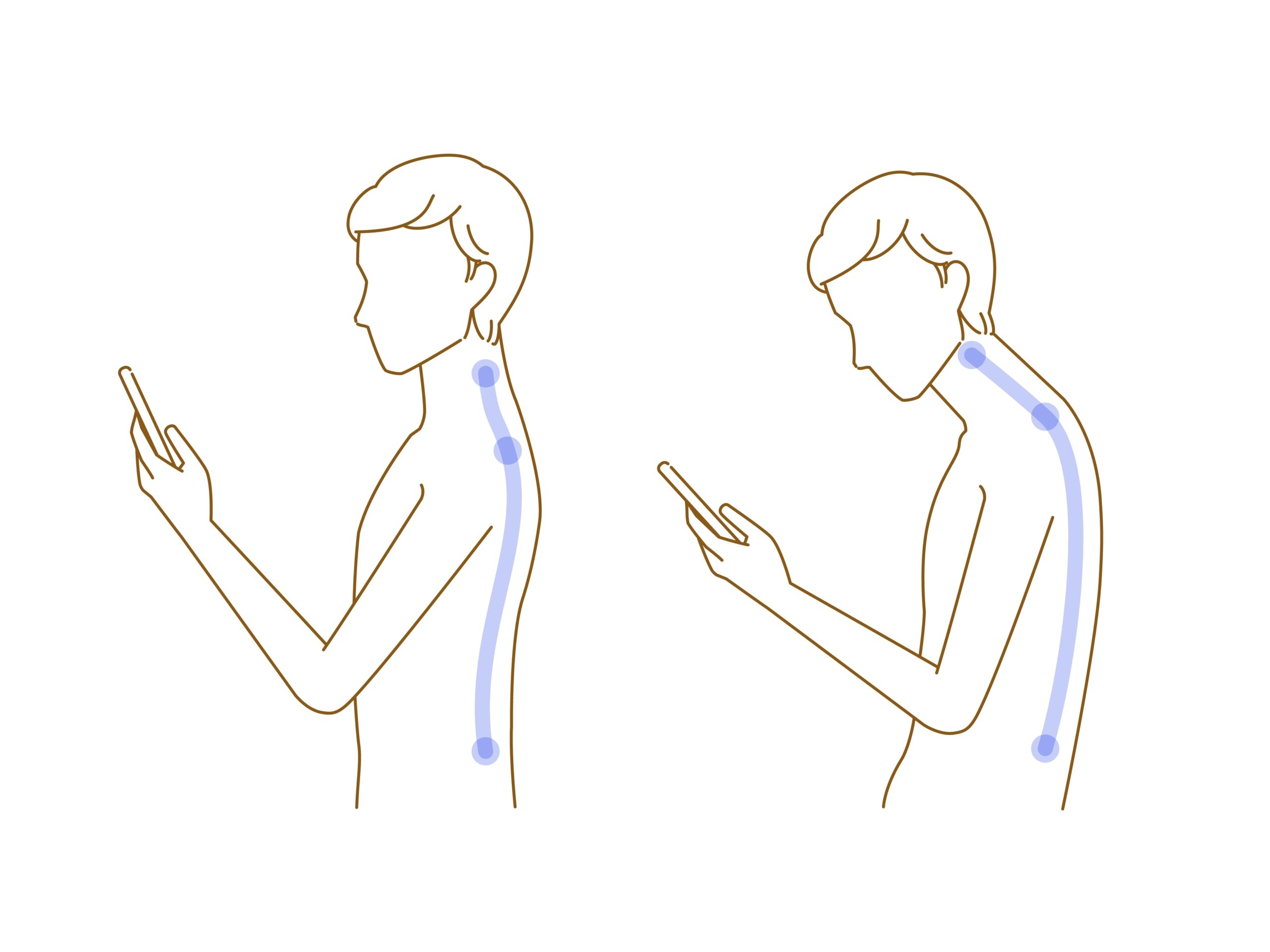
But modern posture often interferes with this.
Forward head posture and slumped sitting can reduce diaphragmatic movement and alter pressure patterns within the chest.
Research has shown that forward head posture significantly alters breathing mechanics and respiratory muscle function (Kang et al., 2018).
Less diaphragmatic movement means less natural lymphatic pumping.
This is one of the reasons breathing exercises often form part of lymphatic therapy and cancer rehabilitation programmes.
Heat, hydration and daily inflammation
Several everyday factors can also influence swelling later in the day:
• warm weather dilates blood vessels
• dehydration thickens fluid transport
• high salt intake alters fluid balance
• long periods of sitting reduce muscle pumping.
Even air travel can temporarily increase swelling because cabin pressure and immobility change fluid dynamics. I wrote about this in more detail here:
When should swelling be checked?
Most daily swelling is harmless and improves overnight.
But persistent or increasing swelling should always be assessed, particularly if you have had:
• cancer treatment
• lymph node removal
• surgery
• infection or injury.
Early advice can make a significant difference.
You can also read more here:

A gentle note if this sounds familiar
If you’re noticing swelling that feels new, confusing or frustrating, you’re not alone.
Often people are told simply to “keep an eye on it”.
But there are ways to support the lymphatic system through movement, breathing, manual lymphatic drainage and simple daily habits.
If you’d like to understand what might be happening in your own body, you’re very welcome to get in touch.
If you are local to Clacton, Essex or Bury St Edmunds and need support with swelling or recovery, I offer treatments in these locations.
Sometimes a short conversation can bring a lot of clarity.
References
DiSipio T et al. (2013) Incidence of unilateral arm lymphoedema after breast cancer: systematic review and meta-analysis.
Lancet Oncology.
Mortimer PS & Rockson SG (2014) New developments in clinical aspects of lymphatic disease.
Journal of Clinical Investigation.
Rockson SG (2018) Lymphatic dysfunction in lymphoedema.
Annals of the New York Academy of Sciences.
Choe K et al. (2015) Neural regulation of lymphatic vessels.
Nature Reviews Immunology.
Kang JH et al. (2018) The effect of forward head posture on respiratory function.
Journal of Physical Therapy Science.
