One of the most common questions people ask after cancer treatment is:
“Why does my swelling come and go?”
You might notice that some days everything feels normal, and on other days a limb feels heavier, tighter or slightly swollen. This can feel confusing and sometimes worrying.
The reassuring news is that fluctuating swelling is quite common, particularly when the body is still adapting after treatment.
Understanding why this happens can help you feel more confident about what your body is doing.

Your Body Is Always Managing Fluid
Our bodies are constantly moving fluid through the tissues.
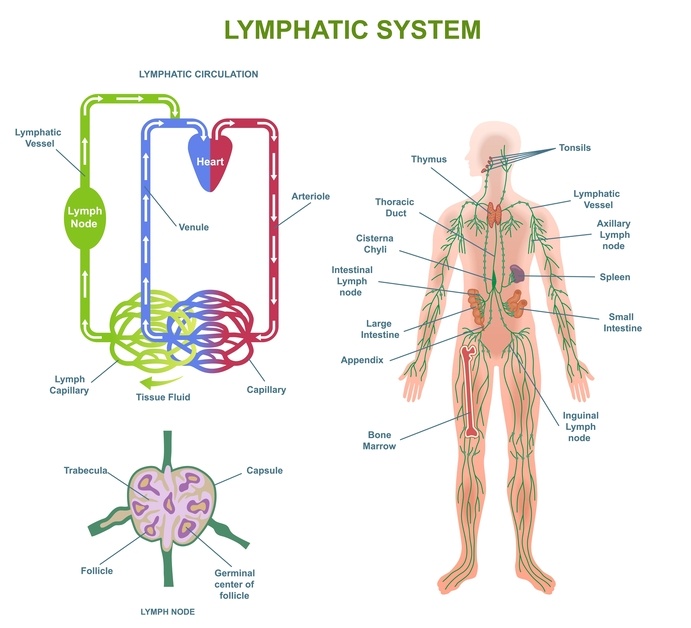
Tiny blood vessels called capillaries allow fluid, nutrients and oxygen to pass into the spaces between our cells. The lymphatic system then collects this fluid and returns it to the circulation.
Most of the time this system works quietly in the background and we do not notice it. Find out more in my Lymphatic system blog.
However, if the amount of fluid entering the tissues temporarily becomes greater than what the lymphatic system can comfortably clear, swelling may appear for a while and then settle again.
Specialists sometimes refer to this as dynamic lymphatic overload.
Cancer Treatment Can Change How the Body Manages Fluid
After cancer treatment, the lymphatic system and surrounding tissues may need to work a little harder than before.
Several factors can influence how easily fluid moves through the body.
Surgery and the Lymphatic System
Surgery can influence fluid movement in a few different ways.
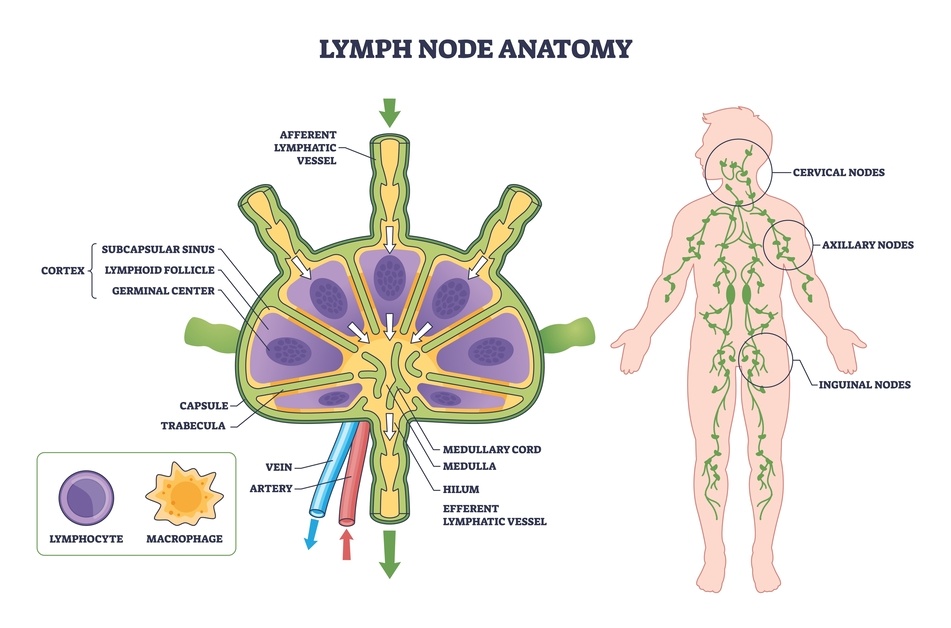
During cancer surgery, lymph nodes are sometimes removed to check whether cancer cells have spread. This can reduce the lymphatic system’s transport capacity, meaning the body may have a slightly reduced ability to move fluid away from the tissues.
Healing tissues also create inflammation, which increases the amount of fluid the body needs to manage.
For most people the body adapts remarkably well, but the lymphatic system may need time to adjust. During this period swelling may appear occasionally as tissues continue healing.
Surgery and the Lymphatic System
Surgery can influence fluid movement in a few different ways.
During cancer surgery, lymph nodes are sometimes removed to check whether cancer cells have spread. This can reduce the lymphatic system’s transport capacity, meaning the body may have a slightly reduced ability to move fluid away from the tissues.
Healing tissues also create inflammation, which increases the amount of fluid the body needs to manage.
For most people the body adapts remarkably well, but the lymphatic system may need time to adjust. During this period swelling may appear occasionally as tissues continue healing.
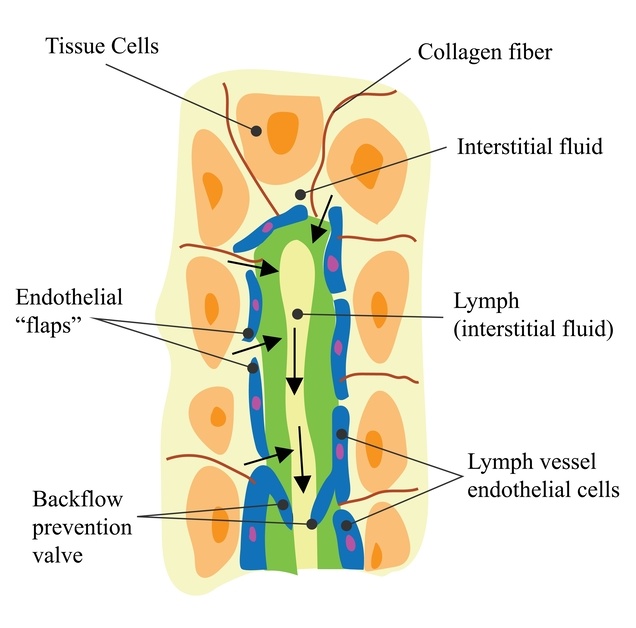
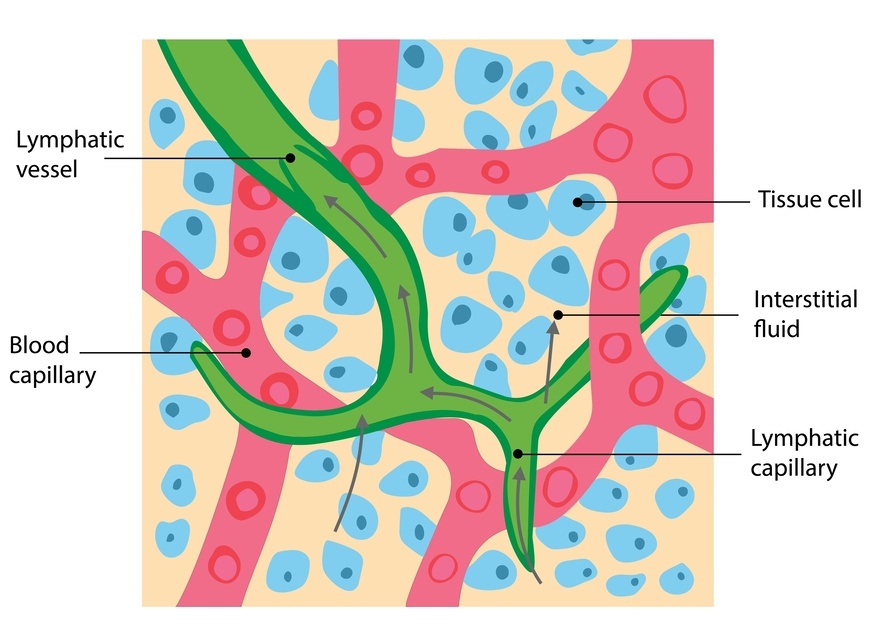
Chemotherapy and Tissue Fluid Changes
Chemotherapy does not only target cancer cells. It can also affect many of the tissues that help regulate fluid balance.
Some treatments can make the tiny capillaries slightly more permeable, meaning a little more fluid moves into the tissues before being cleared by the lymphatic system.
Chemotherapy can also affect how tissues repair and regulate inflammation, which may contribute to temporary swelling in some people.
Fatigue is another common side effect of treatment. When energy levels are low, people naturally move less, and this reduces the gentle pumping effect that muscles normally provide for circulation and lymph flow.
Research consistently shows that fatigue is one of the most common side effects during cancer treatment. Some studies estimate that up to 80% of people receiving chemotherapy experience significant fatigue at some stage of treatment.
External research:
Cancer Research UK – Cancer fatigue
https://www.cancerresearchuk.org
Steroids and Fluid Retention
Steroids are often used alongside cancer treatments to reduce inflammation and help manage side effects such as nausea.
While they are very useful medications, they can sometimes influence how the body regulates water and sodium balance. For some people this can lead to temporary fluid retention, making swelling feel more noticeable.
This type of swelling is usually temporary and often improves once medications are reduced or stopped.
Anaemia and Reduced Oxygen Delivery
Anaemia is another factor that can influence how the body manages energy and fluid during cancer treatment.
Anaemia occurs when there are fewer healthy red blood cells available to carry oxygen around the body. This can lead to fatigue, reduced stamina and a general feeling of weakness.
When energy levels are low, people naturally become less active, which means the body loses some of the gentle muscle pumping that helps support circulation and lymphatic flow.
Anaemia is very common during cancer treatment. The European Cancer Anaemia Survey found that around 39% of cancer patients had anaemia, with higher rates seen during chemotherapy.
As energy levels gradually improve and activity increases again, the body’s natural circulation and lymphatic movement often improve too.
External research:
European Cancer Anaemia Survey
https://www.sciencedirect.com
Changes in Activity Levels
Many people become less active during cancer treatment, which is completely understandable.
Movement plays an important role in helping fluid circulate through the body. Muscles act like small pumps that assist both blood circulation and lymphatic flow.
When activity levels reduce for a period of time, fluid can sometimes linger in the tissues a little longer.
The encouraging news is that gentle movement — even short walks — can help stimulate circulation again as recovery progresses.

Age and Tissue Changes
As we get older, connective tissues naturally change.
Collagen and elastin fibres may become slightly less elastic and circulation can slow a little compared with earlier life. These changes are normal, but they can sometimes influence how fluid moves through the tissues.
Regular movement and strength work can help support tissue health and circulation.
Gut Health and Inflammation
Cancer treatments can also influence the digestive system and the balance of bacteria within the gut.
Researchers are increasingly exploring how gut health influences inflammation, immune function and tissue repair.
Changes in inflammation levels may affect how tissues respond to healing and fluid regulation.
Supporting gut health through balanced nutrition and medical guidance can therefore play a role in recovery.
You can read more on gut health “Gut feelings after cancer”
When Swelling Settles and When to Monitor
Occasional swelling that improves with:
• movement
• elevation
• overnight rest
may simply reflect temporary fluid imbalance.
However swelling that persists, worsens or feels progressively heavier should always be discussed with a healthcare professional.
Early support can make a significant difference and help prevent further strain on the lymphatic system.
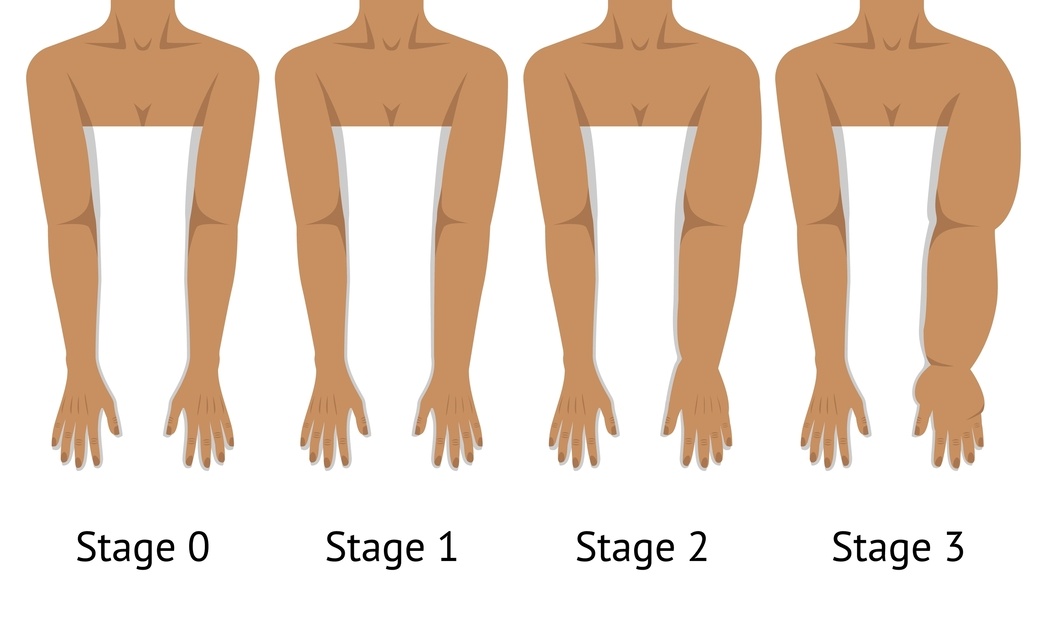
Understanding Your Body After Treatment
Cancer treatment asks a lot of the body, and recovery is often a gradual process. You can read my blog “why does my arm feel heavy?” for information about swelling and lymphoedema
Fluctuating swelling is often a sign that the body is continuing to adapt, repair and rebalance.
Paying attention to these changes, staying gently active and seeking advice when needed can all help support long-term health.
Get In Touch
If you have noticed swelling that comes and goes and would like to better understand what might be happening in your body, exploring reliable information and speaking to experienced practitioners can be helpful.
I regularly share guidance on lymphatic health, recovery after cancer treatment and gentle ways to support the body through movement and bodywork.

