
Connective tissue and the lymphatic system
This came up in a cancer support group recently.
Someone mentioned they had a connective tissue disorder (hypermobility & EDS) and asked whether that might be linked to the swelling they were noticing in their leg.
It’s a really good question — and one I don’t think gets asked enough.
Sometimes people notice heaviness, tightness or swelling after surgery or treatment and assume they’ve done something wrong. That they’ve overdone it. Not moved enough. Moved too much. Drunk the wrong thing. Lifted the wrong thing.
But occasionally, there might be something else influencing how their body responds.
Although this conversation took place in a cancer support setting, connective tissue differences can influence how the lymphatic system behaves more broadly — even in people who have not had cancer treatment.
Why Some People Swell More Easily Than Others
One thing many people do not realise is that swelling is not just about how much fluid is in the body — it is also about how efficiently that fluid can move through the tissues and back into circulation.
Our lymphatic system is constantly working to remove excess fluid, proteins and waste products from the spaces between our cells. Sometimes the amount of fluid needing to be cleared (what specialists call lymphatic load) temporarily becomes greater than what the lymphatic system can comfortably transport.
This can happen after surgery, during illness, in hot weather, on long journeys, or even after a very active day. For some people the lymphatic system catches up quickly and the swelling settles. For others — particularly after cancer treatments involving lymph nodes — the system may already be working harder than normal, which can make swelling appear more easily than it does for someone else.
People living with connective tissue disorders such as hypermobility syndromes and Ehlers–Danlos Syndrome (EDS) are not just dealing with “loose joints” — the altered collagen that affects ligaments and fascia can also reduce proprioception (the body’s ability to sense where it is in space).
Research has shown that joint position sense is often impaired in people with hypermobility and EDS, meaning the nervous system receives less accurate feedback about movement and stability (Rombaut et al., 2010; Sahin et al., 2008). This matters when we start talking about swelling, because efficient lymphatic and venous return rely on subtle muscle activity and pressure changes to move fluid through tissues. Strategies such as gentle body brushing can support lymphatic flow and increase sensory awareness of the skin and underlying tissues, while appropriately fitted compression garments may offer a dual role — helping to manage swelling whilst also providing external feedback that improves joint awareness and perceived stability.
Likewise, carefully selected strengthening and stability-focused exercise can enhance neuromuscular control and encourage fluid movement without overloading vulnerable connective tissues.
As always, proper diagnosis and individual guidance are important — because managing hypermobility, swelling and fatigue rarely comes down to a single intervention. It’s often a case of bringing together different supports — movement, garments, hands-on therapies and education — each offering a piece of the puzzle within the wider village of care.
First things first… what is connective tissue?
Connective tissue is the body’s scaffolding.
It includes things like:
-
fascia
-
ligaments
-
tendons
-
skin
-
fat
-
blood vessel walls
-
and the tiny structures that support your lymphatic vessels
It’s made up of cells sitting within a kind of supportive “gel” made from collagen, elastin and ground substance. This gel helps tissues stay hydrated, flexible and able to cope with load.
In simple terms:
It’s what helps hold everything together — and helps fluids move through the body in a controlled way.
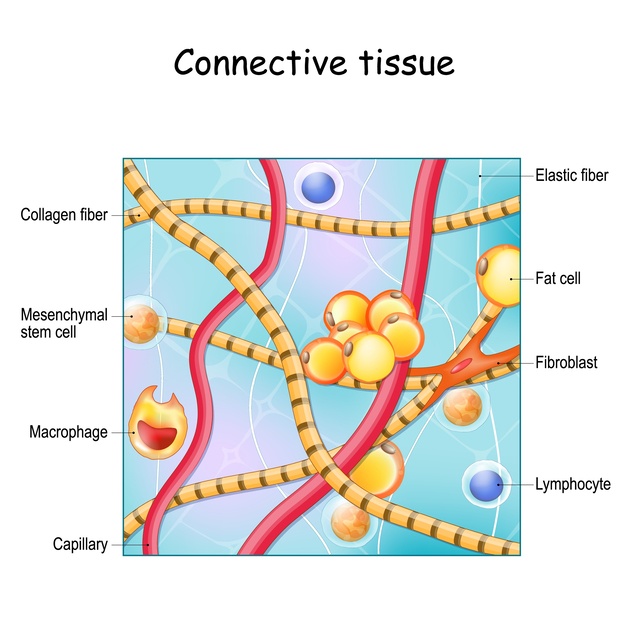
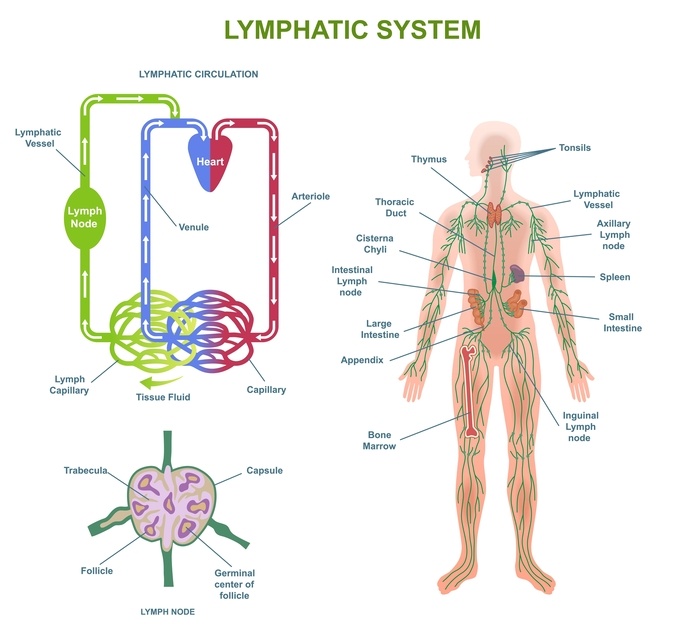
So where do the lymphatics come in?
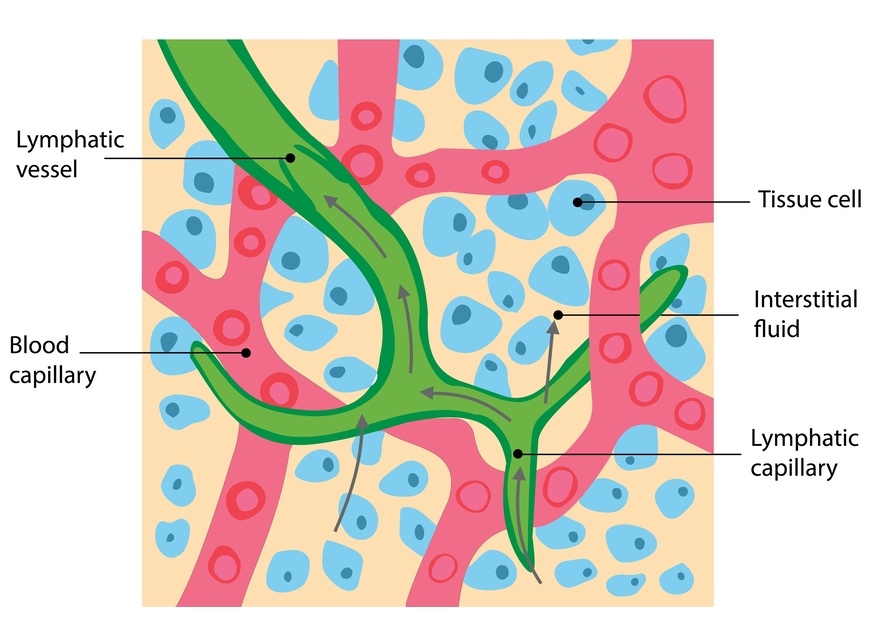
Your lymphatic system sits within this connective tissue network.
Lymphatic capillaries (the very small vessels that collect fluid from your tissues) rely on:
-
surrounding tissue tension
-
anchoring filaments
-
pressure changes in the tissue space
to open and close.
These vessels don’t have a strong muscular wall like arteries do.
Instead, they are supported by the connective tissue around them.
When the tissue moves well, hydrates well and responds to pressure changes appropriately, lymph fluid can enter these vessels more easily.
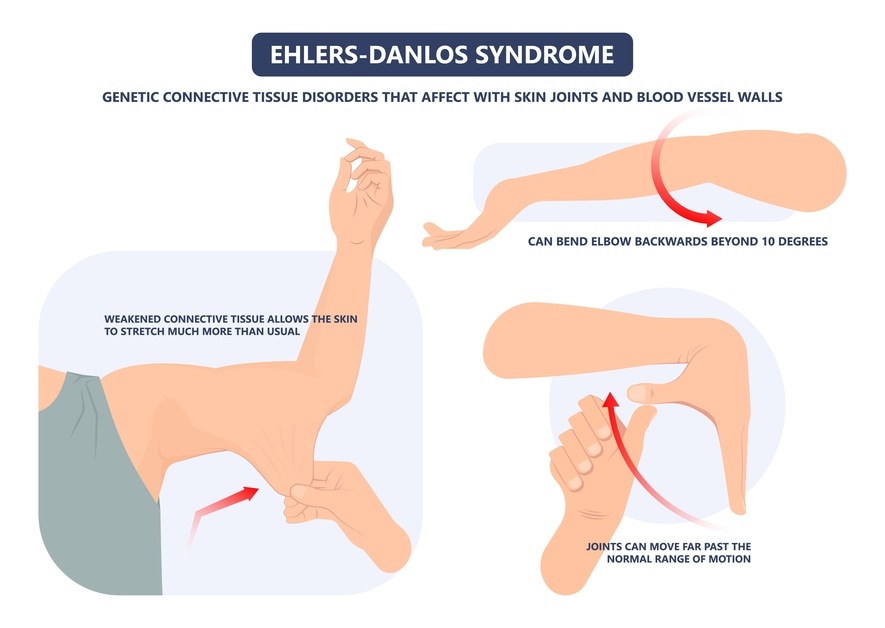
What happens if connective tissue behaves differently?
In some connective tissue disorders (such as hypermobility syndromes or Ehlers-Danlos Syndromes), the collagen and elastin that help provide structural support may behave differently.
This can affect:
-
tissue elasticity
-
vessel integrity
-
pressure relationships in the interstitial space
-
and possibly how well the lymphatic capillaries respond to stretch and recoil
Some people with hypermobility spectrum disorders report:
-
easy bruising
-
limb heaviness
-
slower recovery after activity
-
fluid retention
-
or swelling that takes longer to settle
There is also emerging discussion in the research around altered lymphatic or vascular function in connective tissue conditions — although this is still an area where more research is needed.
A 2020 review in Clinical Rheumatology discussed overlap between joint hypermobility syndromes, fatigue and autonomic dysfunction — all of which may influence vascular tone and fluid regulation.
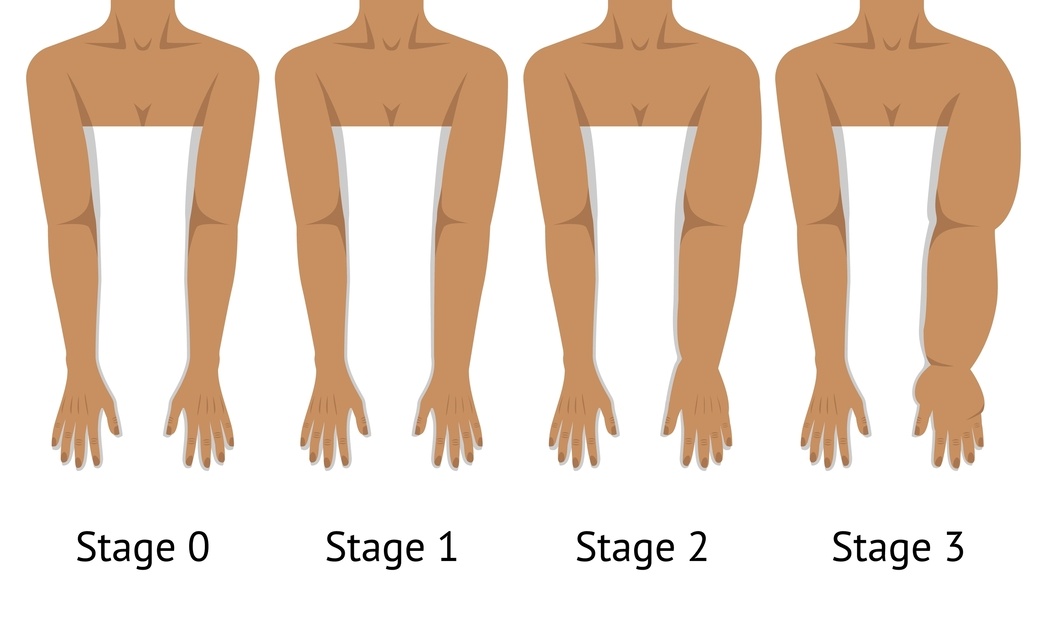
Does this mean I will get lymphoedema?
No — not necessarily.
But it may mean:
-
your tissues respond differently to load
-
you might notice swelling or heaviness more readily
-
recovery from surgery or injury may take longer
Sometimes recovery doesn’t feel straightforward — not because you’re doing anything wrong, but because your connective tissue, joints or vascular system may respond differently to load or fluid shifts.
You can find more information on the lymphatic system here
Understanding this can help you prepare for participation in movement, exercise or manual therapies in a way that feels safer and more supportive.
What might support look like?
Support may include:
-
gentle compression (where appropriate)
-
education around limb care
-
and movement strategies that encourage fluid exchange without overwhelming the tissues
As someone currently following the same medical lymphoedema training pathway as NHS specialists like Kerry, these are the kinds of conversations that are helping shape how I can support people safely in the community — alongside, and in step with, NHS services.
When is it worth seeking specialist advice?
If you notice:
-
persistent swelling
-
a feeling of heaviness
-
tightness in the skin
-
jewellery or clothing leaving marks
-
swelling that doesn’t settle overnight
it may be worth speaking to your GP or a specialist lymphoedema service for assessment.
Where connective tissue differences are involved, a more detailed clinical assessment can sometimes help guide appropriate advice around compression, conservative management or longer-term support.
• New swelling should be investigated -> GP
• Managing long-term -> Specialist exercise and if you have swelling advice from specialist MLD practitioner who will give home care advice alongside treatment
If you are experiencing swelling, heaviness, scar tightness or changes in your body after surgery or cancer treatment, it can be helpful to talk things through with someone who understands how the body heals and adapts.
I work with people navigating these kinds of changes using Manual Lymphatic Drainage, scar therapy and gentle rehabilitation movement.
You are welcome to get in touch if you would like to explore what might help your recovery.
Many people contact me after reading this article because they are unsure whether their swelling or symptoms are normal.
Email Fiona – fi@therapyinmotion.co
or
