
Emerging Evidence and Clinical Application
Osteoarthritis (OA) has long been described as “degenerative”.
But that word doesn’t tell the whole story.
We now understand osteoarthritis as a whole-joint disease involving:
-
Cartilage breakdown
-
Subchondral bone remodelling
-
Synovial inflammation
-
Capsular thickening
-
Intermittent joint effusion
According to Versus Arthritis, around 10 million people in the UK live with arthritis, and osteoarthritis remains the most common form.
What has shifted in recent years is our understanding of the inflammatory component.
OA is not rheumatoid arthritis.
But it is not purely mechanical either.
Synovial Inflammation and Effusion in OA
• Simple – “Joint effusion in osteoarthritis is a build-up of excess fluid inside the joint, which makes it feel swollen or puffy.”
Research published in journals such as Arthritis Research & Therapy demonstrates that synovitis is present in many patients with knee osteoarthritis — even in early stages.
Imaging studies frequently reveal:
-
Synovial thickening
-
Joint effusion
-
Increased inflammatory mediators within synovial fluid
Effusion increases intra-articular pressure. Elevated pressure has been linked with:
-
Pain
-
Arthrogenic muscle inhibition (particularly quadriceps inhibition)
-
Reduced range of motion
Swelling is not just a side effect.
It actively alters joint mechanics and neuromuscular function.
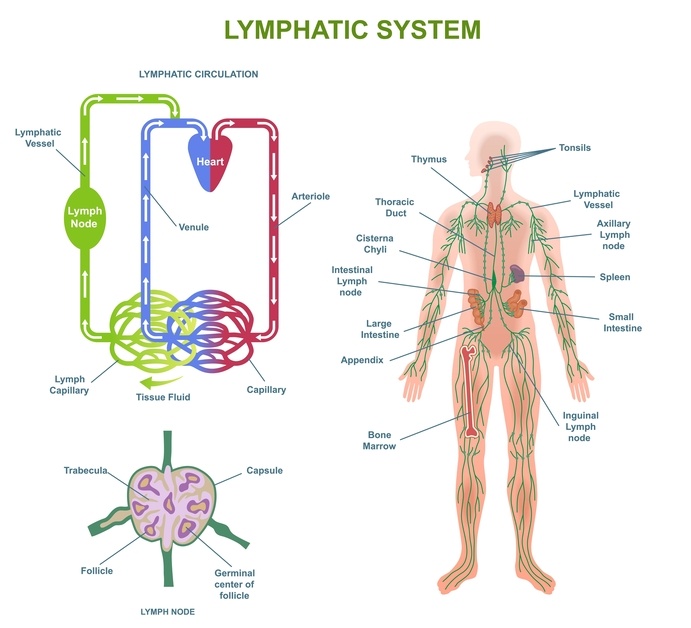
The Lymphatic System and Joint Homeostasis
• Simple– “Homeostasis is the body’s way of keeping it’s internal environment steady – temperature, fluids and chemistry – so everything can work properly.” My recent blog on OA and MLD offers a beginner friendly chat
The lymphatic system is responsible for:
-
Removal of excess interstitial fluid
-
Clearance of proteins from the extracellular space
-
Transport of inflammatory mediators
-
Immune surveillance
Recent research has explored the role of lymphatic dysfunction in chronic inflammatory diseases. Animal models have demonstrated that impaired lymphatic drainage can prolong joint inflammation, while enhanced lymphatic function may reduce inflammatory burden.
Although much of this research is still emerging — and more robust human trials are needed — the biological plausibility is clear.
If inflammatory mediators accumulate within joint tissues, and if lymphatics are responsible for clearance, then impaired drainage may contribute to symptom persistence.
What Is Vodder Manual Lymphatic Drainage?
Emil Vodder developed Manual Lymphatic Drainage (MLD) in the 1930s.
Vodder MLD is:
-
Low pressure (skin-stretch based)
-
Rhythmic
-
Directional
-
Designed to stimulate superficial lymphatic vessels and lymphangion contraction
Unlike deep manual therapy, it does not compress muscle tissue. It works at the level of the superficial lymphatic capillaries.
The goal is to enhance physiological drainage pathways — not to force fluid movement.
You can read more about how I use Manual lymphatic drainage in clinic here
Clinical Evidence for MLD in Osteoarthritis
The evidence base is modest but promising.
A 2013 study in the Journal of Physical Therapy Science demonstrated that patients with knee osteoarthritis who received MLD alongside exercise experienced greater improvements in pain and knee range of motion compared to exercise alone.
Other small-scale studies and clinical observations report:
-
Reduced swelling
-
Improved joint mobility
-
Decreased perceived stiffness
Importantly, MLD is generally well tolerated — particularly in individuals who cannot tolerate deep or forceful manual therapy.
We must be cautious not to overstate findings.
MLD is not disease-modifying.
But it may be symptom-modulating.
Potential Mechanisms of Action
From a clinical reasoning perspective, MLD may influence osteoarthritis symptoms through several pathways:
• Reduction of Periarticular Oedema
Lower tissue pressure reduces mechanical nociception and may improve joint comfort.
• Enhanced Clearance of Inflammatory Mediators
While not directly altering cartilage pathology, improved lymphatic flow may assist regulation of the inflammatory environment.
• Neuromodulation
MLD has demonstrable parasympathetic effects. Reduced sympathetic tone may decrease muscle guarding and central sensitisation components.
• Improved Tissue Mobility
Reduced interstitial congestion enhances fascial glide and movement tolerance.
Osteoarthritis, Menopause and Cancer Treatment
This is particularly relevant in my clinical population.
Hormone therapies used in breast and prostate cancer (such as aromatase inhibitors) are associated with joint pain and stiffness. Reduced oestrogen levels influence joint health and inflammatory processes.
Cancer treatment may also involve:
-
Steroid use
-
Reduced physical activity
-
Sarcopenia
-
Systemic inflammatory stress
Many individuals report new or worsened joint symptoms during or after treatment.
Inflammation and fatigue often sit alongside joint stuffness during or after treatment – read more on fatigue after cancer
In these cases, the line between treatment-induced arthralgia and osteoarthritis is often blurred.
Manual Lymphatic Drainage does not treat hormone-related joint pain directly.
However, by addressing swelling, inflammatory load and nervous system regulation, it may provide supportive relief in a population often unable to tolerate aggressive manual therapy.
You can read more about my integrated approach to inflammatory and cancer recovery care at Pilates Therapy and Bodywork. Strength remains central to managing osteoarthritis long-term.
Where MLD Sits Within Best Practice
NICE guidelines for osteoarthritis emphasise:
-
Strengthening
-
Weight management
-
Education
-
Ongoing activity
MLD should not replace these.
Rather, it may be considered:
-
During inflammatory flares
-
When swelling limits strengthening
-
In early rehabilitation phases
-
Post-surgically
-
In oncology-related joint pain
It becomes an adjunct — not a primary intervention.
Clinical Summary
Osteoarthritis is increasingly recognised as a condition involving inflammatory processes and fluid dynamics, not solely structural degeneration.
While large-scale trials are still needed, emerging research suggests lymphatic function may influence inflammatory joint environments.
Manual Lymphatic Drainage offers:
-
A low-risk
-
Low-load
-
Neurologically calming
-
Physiologically plausible
supportive intervention within a multi-layered rehabilitation model.
It is not dramatic.
It is not curative.
But in the right context, it may be useful.
And sometimes, in chronic conditions, useful is enough.
