I saw a set of images recently talking about “inflamed vs clogged lymph nodes” — and I’ll be honest… they caught my attention.
Because visually, they tell a really clear story.
But clinically?
It’s a little more nuanced than that.
And if you’re living with swelling, heaviness, or recovering from cancer treatment or surgery — this difference really matters.
First — a quick grounding point
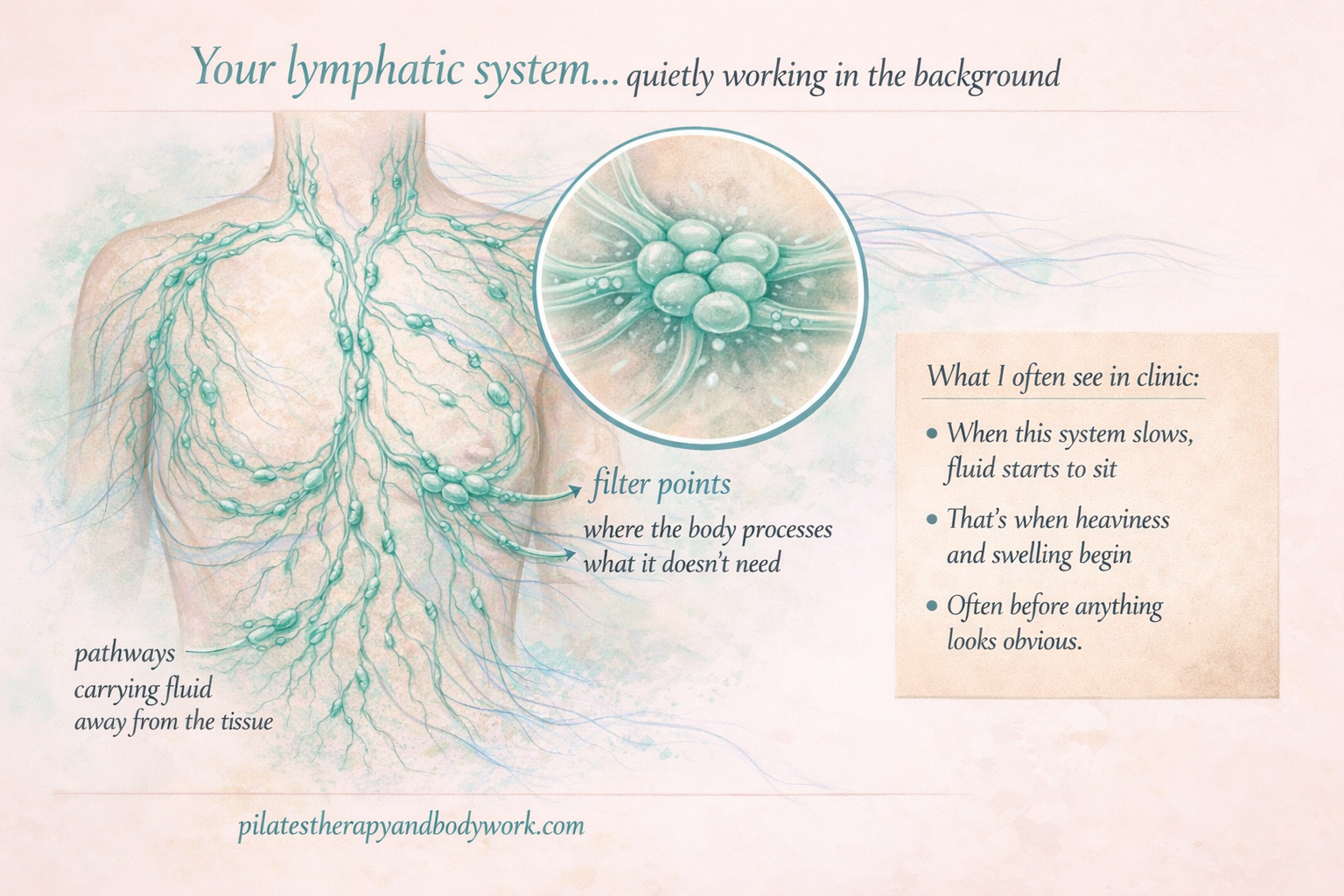
Your lymphatic system isn’t a pipe that gets “blocked” like a drain.
It’s a living, moving system made up of:
- Vessels that contract (lymphangions)
- Nodes that filter and respond
- Fluid that shifts based on pressure, movement, and tissue health
So when something changes…
it’s usually about balance and capacity, not a simple blockage.
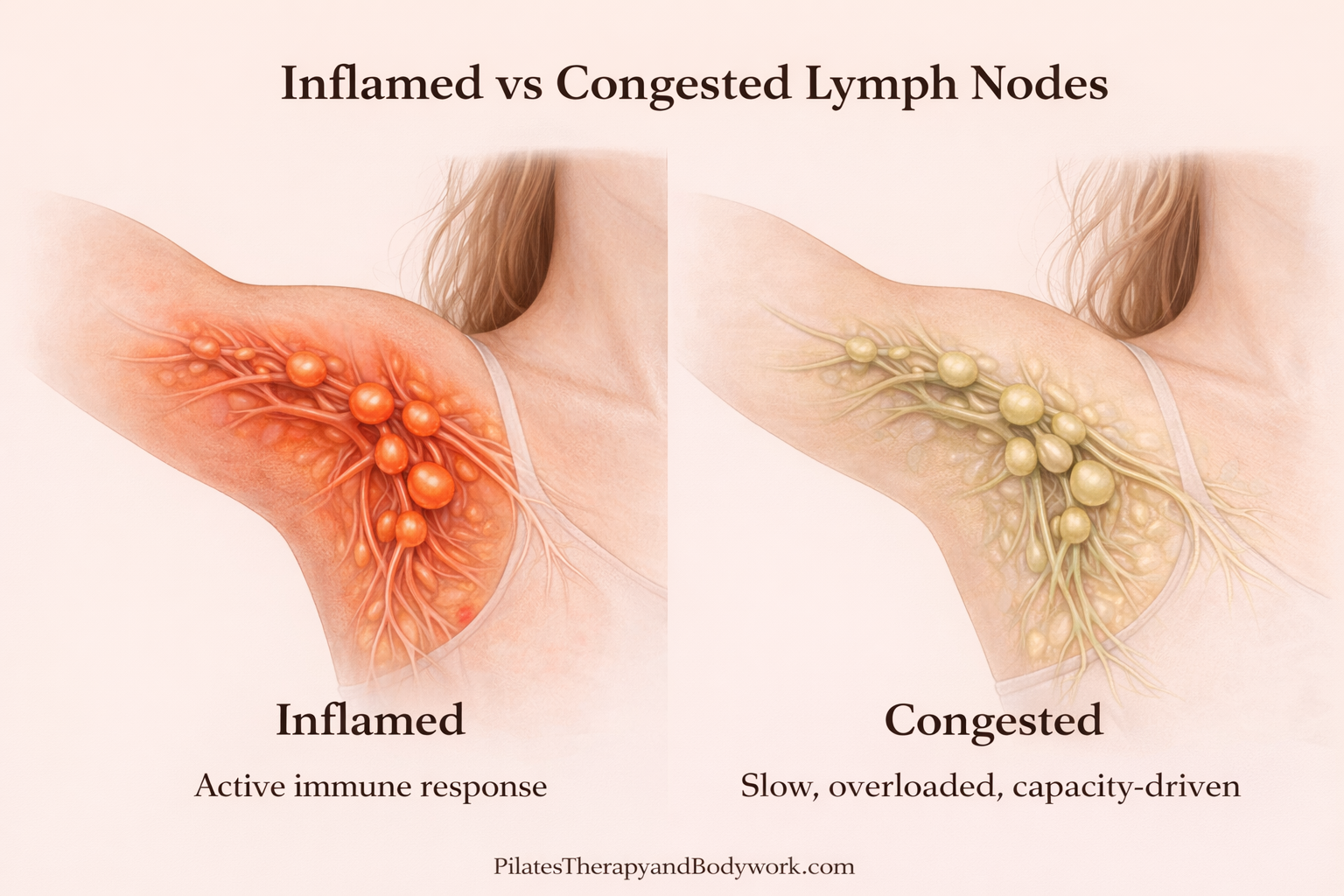
Inflamed lymph nodes — an active process
When lymph nodes are inflamed, they are doing their job.
This is an active immune response.
You might notice:
- Warmth
- Redness
- Tenderness
- Rapid swelling
This often happens with:
- Infection (including cellulitis — important in lymphoedema care)
- Skin irritation
- Post-surgical immune activity
- Illness
A bit of evidence
- Lymph nodes can increase in size due to lymphocyte proliferation during immune response
- Acute inflammation involves increased blood flow and vascular permeability (classic inflammatory cascade)
– This is not something to “drain away aggressively”
It’s something to respect and monitor
“Clogged” lymph nodes — what’s really going on?
This is where language matters.
“Clogged” isn’t a clinical term — but I understand why people use it.
What they’re usually describing is:
Reduced lymphatic transport capacity
In your world (and mine), this is closer to:
- Early swelling
- Fluid retention
- Or lymphoedema
You might feel:
- Heaviness
- Fullness
- Puffiness
- Tight skin
- No heat or redness
What’s actually happening underneath
- Fluid + proteins accumulate in the tissue
- Lymphatic load exceeds transport capacity
- Over time → chronic inflammation + fibrosis risk
Evidence snapshot
- Lymphoedema is estimated to affect up to 1 in 6 people globally in some form
- After breast cancer treatment, risk can range from 20–40% depending on intervention type
– This is not an emergency
But it does need early, consistent support
The key difference (this is the bit most people miss)
- Inflamed = active, immune-driven
- Congested = slow, overloaded, capacity-driven
They can feel similar…
but they need different responses
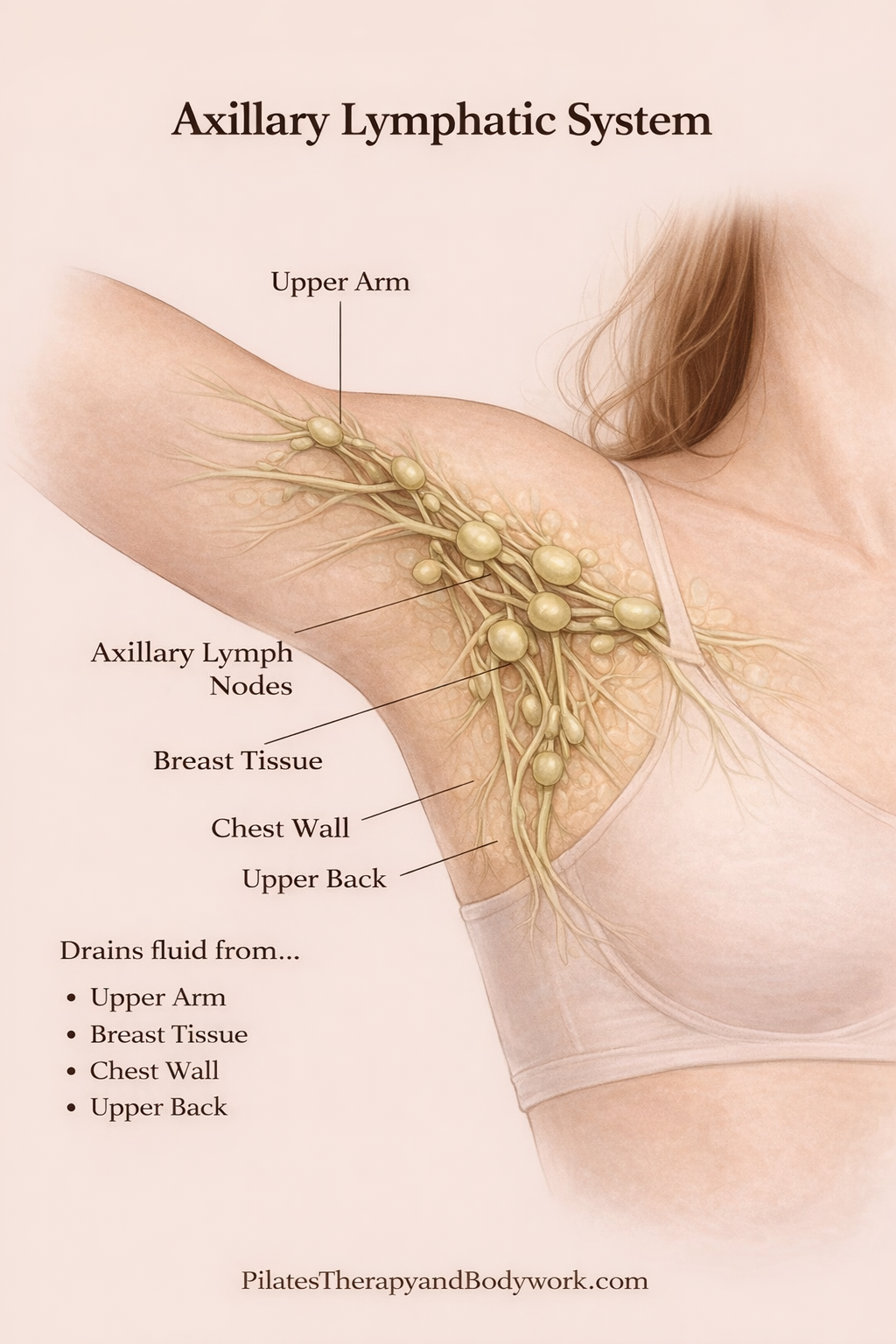
Why the underarm (axilla) matters so much
The axillary lymph nodes are a major drainage hub.
They manage fluid from:
- Arm
- Breast
- Chest wall
- Upper back
So when this area is affected (surgery, radiation, scarring, posture):
– It changes the entire fluid story of the upper body
Movement matters — and this is where WALX fits in
One of the simplest — and most overlooked — ways to support your lymphatic system is how your arms and upper body move throughout the day.
This is where WALX (modified pole walking) becomes incredibly useful.
Not as fitness.
Not as performance.
But as supported, rhythmic movement for flow.
Why the poles make such a difference
In a rehab setting, the poles:
- Support the arm → reducing load through shoulder and chest
- Encourage a natural arm swing → not forced or held movement
- Reduce the need for gripping
- Create a steady rhythm the lymphatic system responds to
– It becomes less about effort, more about fluid movement through tissue
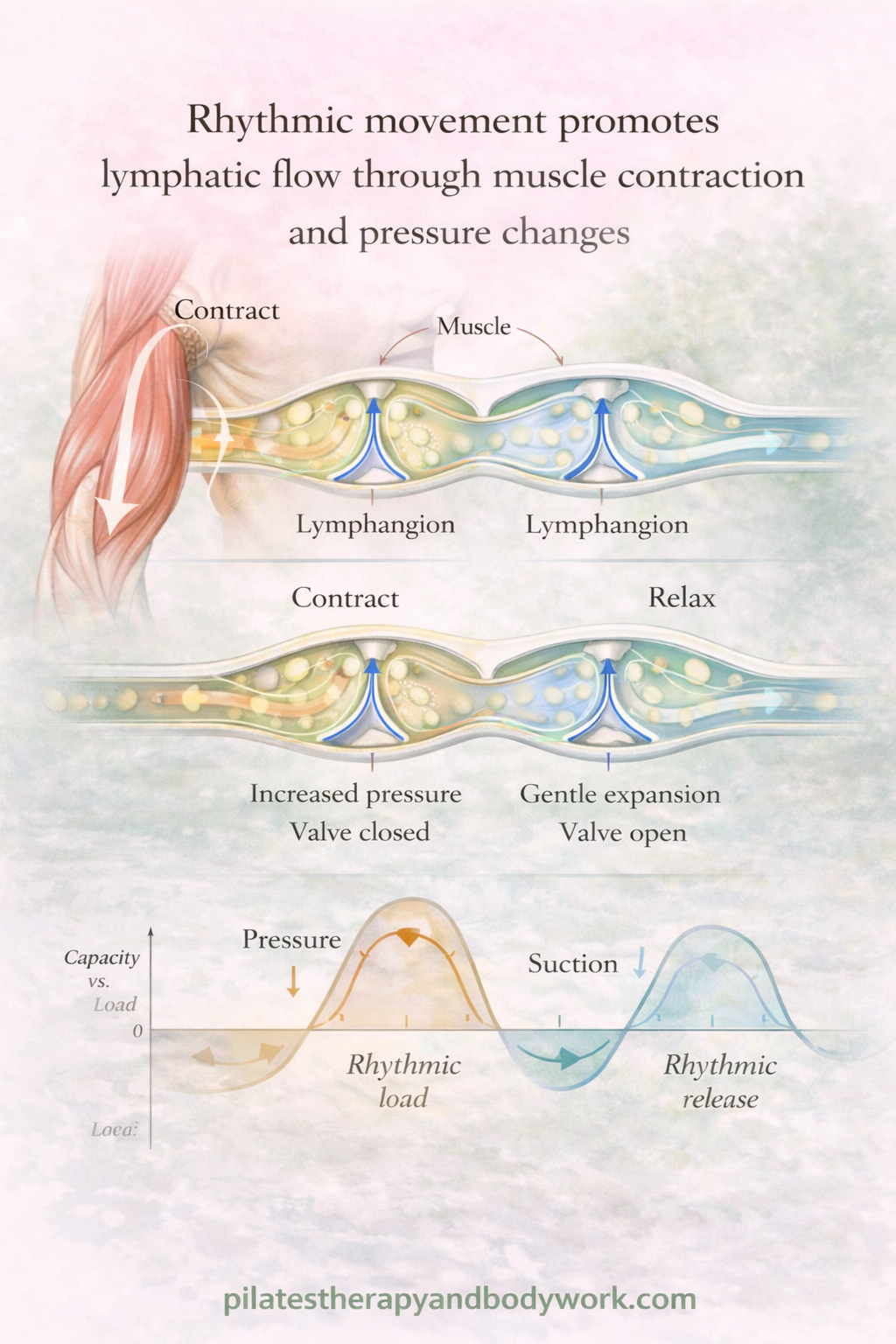
What’s happening in the body
The lymphatic system relies on:
- Muscle contraction
- Breathing
- Pressure changes in tissue
So each step with a gentle arm swing:
- Creates a mechanical push–pull through the tissues
- Supports lymph moving through vessels
- Stimulates lymphangion activity
- Reduces stagnation in areas like the axilla
Why grip matters (and is often missed)
Tension in the hands travels up.
Excess gripping:
- Increases forearm and shoulder tension
- Can reduce fluid movement
- Adds load to sensitive post-surgical areas
With WALX-style technique:
– The hand stays softer, more responsive
Which allows:
- Better circulation
- Less guarding
- More natural movement patterns
What the research supports
- Nordic walking increases upper body muscle activation and circulation compared to normal walking
- Movement-based rehab is associated with improved lymphatic flow and reduced swelling post breast cancer treatment
- Progressive, supported exercise is considered safe and beneficial in lymphoedema risk reduction
– In simple terms:
gentle, repeated movement supports lymph flow better than forceful interventions

A natural next step
If this resonates, you can read more about how I use this approach here:
– WALX Rehabilitation Walking
A layer that’s often missed — these systems overlap
Fluid and inflammation are not separate.
- Fluid stagnation → low-grade inflammation
- Repeated inflammation → reduced lymphatic efficiency
Over time:
– This feeds into the fibrotic cycle
What actually helps (and what doesn’t)
Lymphatic health is not about forcing detox
It’s about:
- Supporting flow and rhythm
- Improving transport capacity
- Reducing load on the system
That might include:
- Manual Lymphatic Drainage
- Breathing
- Gentle movement (like WALX)
- Skin care
- Compression (when appropriate)
A clinical reality (especially after cancer treatment)
If lymph nodes have been removed or affected:
– The system is not blocked — it is adapted
Which means:
- It needs rerouting strategies
- It benefits from early support
- It responds best to informed, gentle input
So… inflamed or “clogged”?
Sometimes one.
Sometimes the other.
Sometimes both.
But the shift is this:
– Not “what’s blocked?”
– But “what does this system need right now?”
If this sounds familiar
If you’re noticing:
- Heaviness in your arm or chest
- Swelling that comes and goes
- Tightness around scars
- Or you’re just not sure what you’re feeling
I work with people across
Clacton-on-Sea, Bury St Edmunds, Essex and Suffolk
Using:
- Manual Lymphatic Drainage
- Scar therapy
- Movement and rehabilitation
Further reading
- NHS lymphoedema guidance
- Macmillan Cancer Support resources
