“My leg is still swollen after a flight… is it just travel, or something else?”
I was asked a really common question at 5K Your Way:
“I’ve been on holiday (Norway), did loads of walking, and now my leg is still swollen… weeks later. Is it just that I overdid it?”
And here’s the bit that matters: this lovely lady has had pelvic surgery and lymph nodes removed in the last few years.
So… in her case (and in yours, if this sounds familiar) we don’t just shrug and blame the hills and the hiking boots.
Because sometimes swelling is just swelling… and sometimes swelling is your body quietly saying: “I’m struggling with load.”
Your first port of call is ALWAYS your gp!

First: what can make legs swell on holiday?
Even in people with no cancer history, travel can cause temporary swelling because:
-
you’re sitting still longer than usual (planes, cars, trains)
-
cabin pressure + long periods with legs down
-
heat, salt, alcohol (all the holiday classics)
-
“more walking than normal” (and your muscle pump gets tired or irritated)
-
a knee flare / joint irritation can create a local fluid response
For many people, that settles in a day or two.
When swelling is more of a “pay attention” moment
If you’ve had lymph nodes removed (especially pelvic/groin nodes), radiotherapy, or significant pelvic surgery, your drainage system may have less “spare capacity” than it used to.
So if you add:
-
a flight
-
long travel days
-
lots of walking
-
a cranky knee
…your lymphatic system can get overloaded. Macmillan specifically flags travel as a time to take extra care with movement and positioning for lymphoedema risk.
And a key point: if swelling persists (days → weeks), especially one-sided, it deserves proper medical attention. Not panic. But attention.
The other reason I’m careful: DVT needs ruling out
I’m going to say this plainly, because it’s important and it’s kind:
If you have one-sided leg swelling after travel, your GP (or urgent care) may need to rule out a blood clot (DVT), especially if there’s pain, heat, redness, tenderness, or breathlessness.
Long-haul travel is linked with increased VTE risk. The WHO work cited in BMJ reporting notes risk roughly doubles after flights longer than 4 hours.
Research summaries also estimate the absolute risk for VTE after flights >4 hours at around 1 in ~6,000 travellers (with higher risk if you have additional factors).
So yes: lymphatic overload is on the table.
But DVT must be ruled out first when the picture fits.
Does flying “cause” lymphoedema?
This is where it gets messy online.
Some NHS guidance states there’s no evidence that flying short or long haul increases the risk of lymphoedema, but still recommends common-sense precautions like hydration and movement.
At the same time, many lymphoedema services recommend compression and movement strategies during flights for people who already have lymphoedema or are at higher risk.
So my honest take is:
Flying may not be the “cause”, but travel is a stress test.
If your lymph system is already working with fewer lymph nodes (or scarred pathways), it might cope fine… or it might show you where the limit is.
What to do if your leg stays swollen after a flight
If this is you, here’s the calm checklist.
• Get the “serious stuff” checked
Contact your GP/111 if you have:
-
one-sided swelling that persists or is getting worse
-
pain in the calf/thigh
-
heat/redness
-
sudden breathlessness or chest pain (urgent)
• Track it (because memory is rubbish when we’re worried)
-
Take a photo morning/evening for 3 days
-
Notice if it softens overnight or stays “stuck”
-
If you have a tape measure: pick 2–3 consistent landmarks and record
This helps the GP and helps you.
• Move like you mean it (but gently)
Macmillan and Cancer Research UK both recommend avoiding long periods in one position and doing gentle movement while travelling.
Even now, post-holiday, your basics are:
-
ankle pumps
-
calf raises
-
short walks little and often (not one heroic march)
-
elevation breaks (leg up, breathe, soften your belly)
• Compression: only if it’s appropriate for you
Compression can be brilliant — but it needs to be the right level and fit, especially with thigh swelling.
Cancer Research UK advises wearing compression if your specialist has suggested it, and that you should be measured properly.
If you already have hosiery from lymphoedema clinic, many NHS leaflets advise wearing it for flights and around travel time.
If you don’t have compression yet, don’t self-prescribe something random online and hope for the best. Get guidance.
• Think “load management”, not “rest forever”
If a knee has flared, your gait changes, the thigh works harder, and fluid can hang around.
So it’s not always “more exercise”. Sometimes it’s:
-
better pacing
-
better alignment
-
rebuild the muscle pump gradually
-
calm the inflammation
This is where rehab movement is genuinely useful.
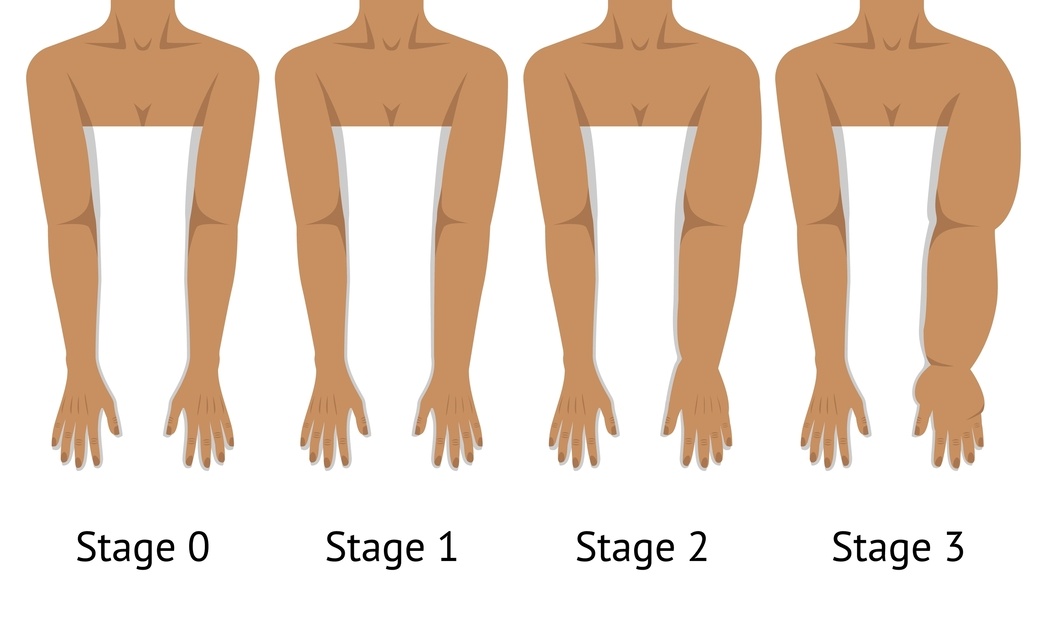
A note from me (because this matters)
Sometimes you can just feel something different: trouser leg feeling a little different one side, heaviness, less ability to bend or straigthen a leg.
If you’ve had lymph nodes removed, you are not being dramatic by asking about swelling. You’re being sensible.
And if you’re sitting there thinking, “I don’t want to bother the GP”…
Please don’t do that thing we all do.
Persistent one-sided swelling after travel is a “get checked” situation — especially with your history.
If you’re local (Clacton / Bury St Edmunds) and you’re dealing with ongoing swelling after surgery or travel, I can help you:
-
make sense of what your body is doing
-
work alongside your medical team
-
build a safe movement plan that supports drainage and confidence
Clacton Clinic – Tuesday and alternate Thursdays
Bury St Edmunds Clinic monthly
Call me to book your appointment 07767 384983
