Fluid Retention vs Lymphoedema: What’s the Difference (and Why It Matters)

Not all swelling is the same
Swelling gets grouped together far too easily.
“Fluid retention.”
“Oedema.”
“Just a bit of swelling.”
But clinically, there’s a difference — and it matters.
Because what’s happening in the tissue, and what your body needs, is not the same.
Fluid retention (oedema) — when the system is under pressure
Fluid retention is usually a temporary imbalance.
It’s often linked to:
-
prolonged sitting or inactivity
-
heat
-
hormonal changes
-
circulation changes
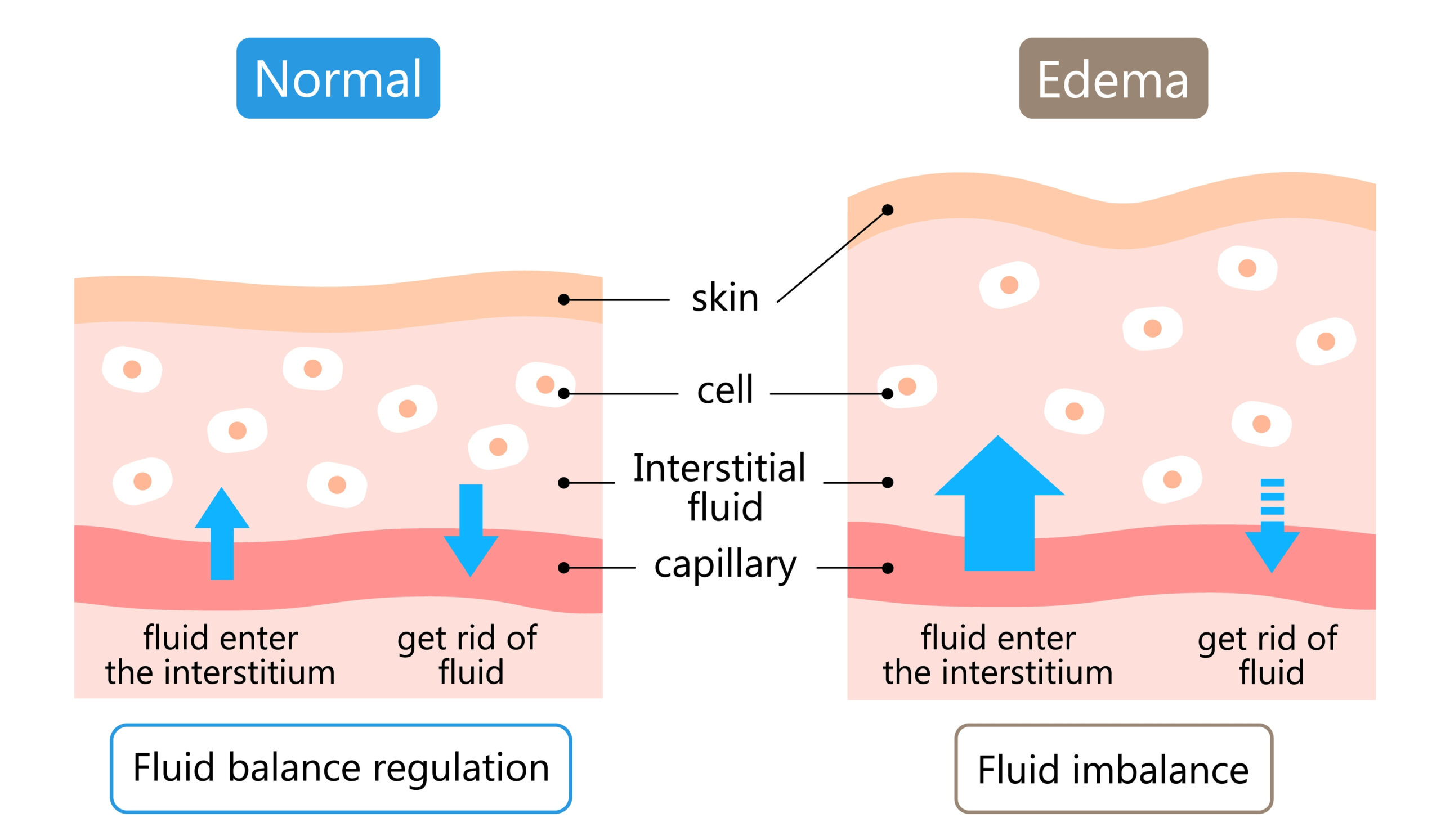
What’s happening here is mainly fluid shifting into the tissues faster than it’s being cleared.
Importantly:
This is typically low-protein fluid
Which means the body can usually reabsorb it and rebalance over time.
Research into peripheral oedema shows this type of swelling is often related to increased capillary filtration rather than lymphatic system failure.
In simple terms:
The system is working — just temporarily overwhelmed.
“If you’re not sure whether what you’re experiencing is ‘just fluid’, you might find this helpful to start with…”

Lymphoedema — when transport capacity is reduced
Lymphoedema is different.
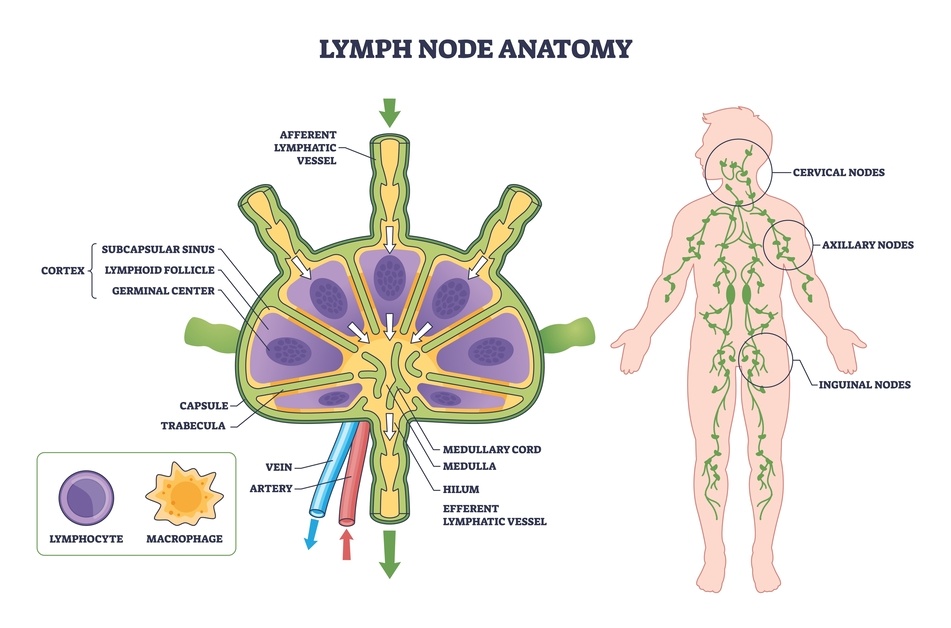
Here, the lymphatic system is not able to transport fluid effectively because its capacity has been reduced.
This may be due to:
-
lymph node removal
-
radiotherapy
-
surgery or trauma
-
or congenital factors
And the key difference:
This is high-protein oedema
That protein content changes everything.
Because it doesn’t just sit passively — it drives a biological response:
-
proteins attract more fluid
-
macrophages are activated
-
fibroblasts are stimulated
-
collagen is deposited
Over time, this leads to fibrosis (tissue thickening and reduced elasticity)
This progression is well documented in lymphoedema management guidelines, including those from the International Society of Lymphology, which emphasise early intervention to prevent long-term tissue changes.
In simple terms:
The system is not coping — and the tissue begins to change.
The key difference (the bit that often gets missed)
This is the simplest way to think about it:
-
Fluid retention → fluid imbalance
-
Lymphoedema → transport problem
Or in everyday language:
-
fluid retention = traffic building up
-
lymphoedema = the road system is damaged
One may settle with time and movement.
The other usually needs ongoing support.
What to look for
There isn’t always a clear line — but there are patterns.
Fluid retention often:
-
fluctuates through the day
-
improves with movement or elevation
-
affects both sides (e.g. both legs)
-
feels soft and pitting
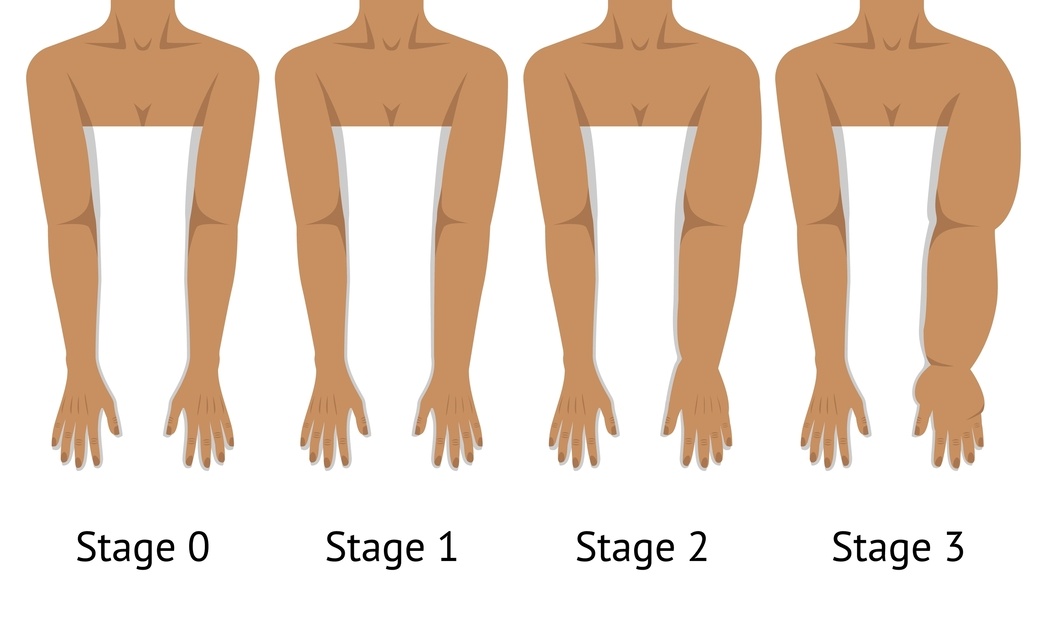
Lymphoedema often:
-
may affect one limb (especially post-surgery)
-
feels heavy, tight, or full
-
does not fully reduce overnight
-
may become firmer over time
-
can involve the hand or foot
Early stages can still be soft and pitting — which is why it’s often missed.
Guidance from the British Lymphology Society highlights that early recognition significantly improves long-term outcomes.
Why this distinction matters
Because being told “it’s just fluid” can delay the right support.
And with lymphoedema, time matters.
The earlier it’s recognised:
-
the easier it is to manage
-
the less tissue change occurs
-
the better the long-term outcome
This isn’t about over-diagnosing.
It’s about not overlooking something that needs a different approach.
Where support fits in
Support doesn’t need to be aggressive.
But it does need to be appropriate.
Depending on what’s going on, this might include:
-
Manual Lymphatic Drainage (MLD)
-
gentle, targeted movement
-
breathing techniques to support pressure changes
-
simple daily positioning strategies
Evidence around MLD shows it can help:
-
stimulate lymphatic flow
-
reduce swelling
-
support tissue health
Particularly in post-surgical and oncology contexts.

You don’t need to work this out alone
This isn’t always easy to identify — even for professionals.
But if swelling is:
-
persistent
-
changing
-
or doesn’t behave the way you expect
…it’s worth getting it looked at properly.
You may find this “pieces of the puzzle” interview with Kerry another local lymphedema specialist interesting.
A gentle next step
If you’re living with swelling, heaviness, or changes in your body — especially after surgery or cancer treatment — you don’t have to navigate it on your own.
I offer specialist, gentle support including Manual Lymphatic Drainage, movement and hands-on therapies in:
Clacton-on-Sea
Bury St Edmunds
Essex & Suffolk
You’re always welcome to get in touch, ask questions, or simply start a conversation.
