
Especially for swelling, healing, pain and brain health
We talk a lot about movement.
Exercise.
Hydration.
But sleep?
Sleep is often the first thing people sacrifice when life feels busy, stressful or uncertain. And yet sleep is not just “rest”. It is one of the main times the body repairs, regulates inflammation, processes pain, consolidates memory and clears waste from the brain. The NHS describes sleep as vital for both physical and mental health, and poor sleep is linked with problems concentrating, low mood and difficulty coping day to day.
In the UK, poor sleep is incredibly common. Recent YouGov data found that while 80% of Britons aim for at least eight hours of sleep, only 19% say they achieve that, 41% report sleeping six hours or less, 38% rarely feel well rested, and 14% say they never do. The Sleep Charity also reports that one in three people are experiencing “sleep poverty”, and says 37% of UK adults experience insomnia.
So this is not a small issue.
It is not a “nice if you can get it” part of health.
It matters far more than most people realise.
And one of my favourite ways to explain part of it is this:
Sleep is like an overnight rinse for the brain.
The brain clean-up system most people have never heard of
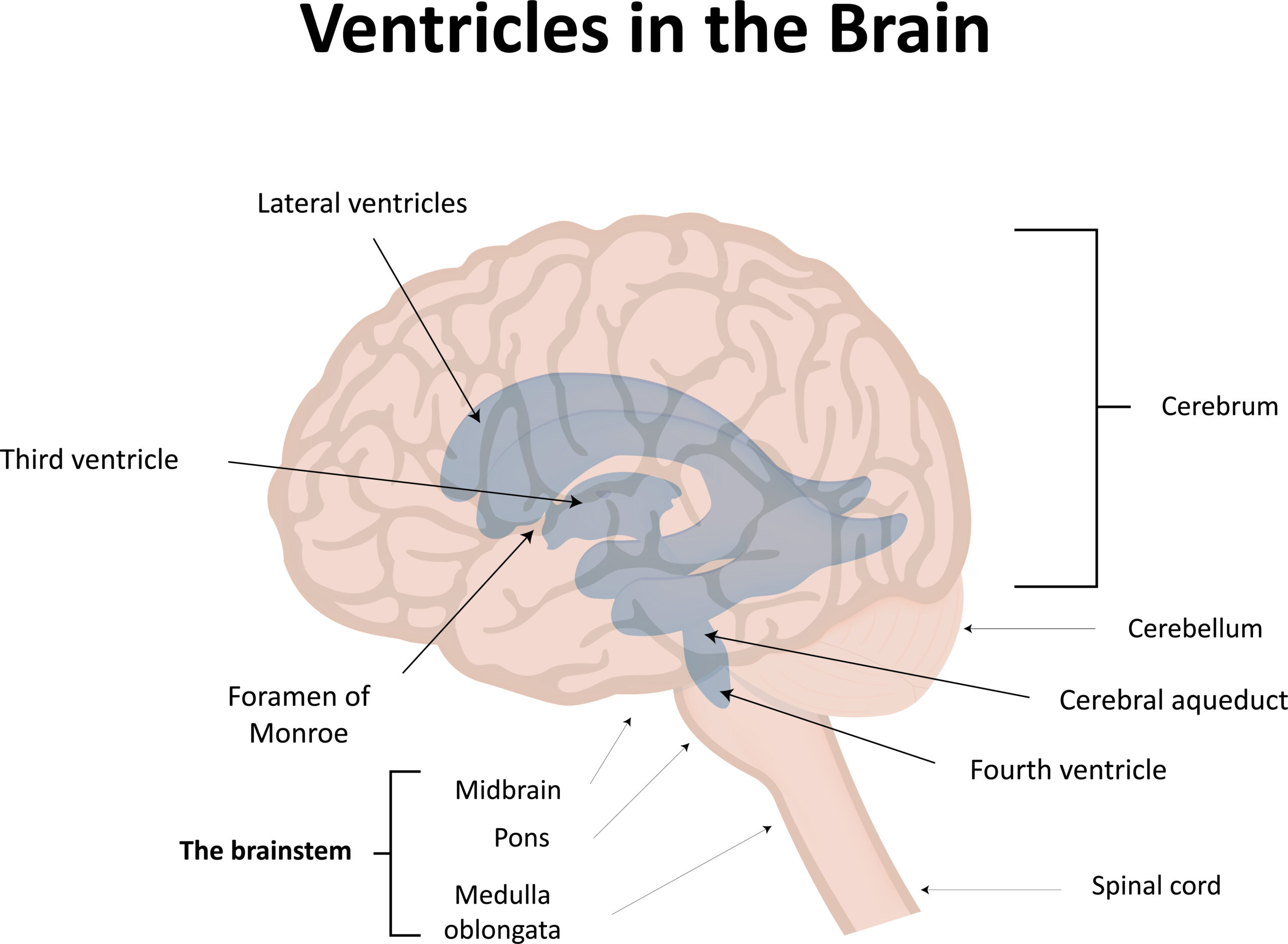
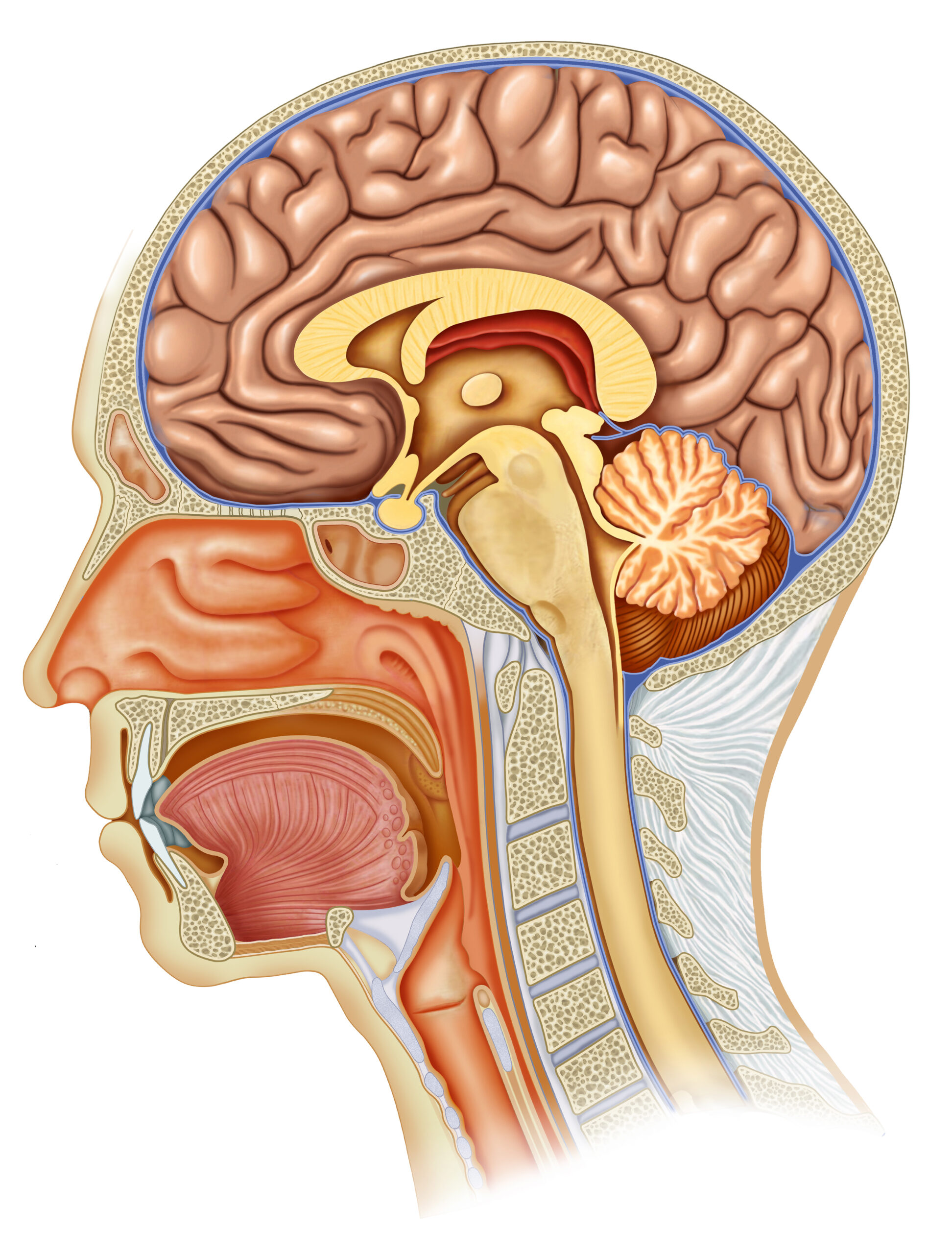
During sleep, the brain activates what is called the glymphatic system — a waste-clearance pathway that helps move cerebrospinal fluid through the brain and clear metabolic by-products. Research has shown that glymphatic activity is much greater during sleep than wakefulness. In the often-cited 2013 study by Xie and colleagues, sleep was associated with a 60% increase in interstitial space in mice, supporting greater fluid exchange and waste clearance. Later reviews have consistently described sleep as a key state for glymphatic function.
That does not mean every poor night’s sleep causes damage. But it does help explain why chronic sleep disruption can leave people feeling foggy, heavy, flat and not quite themselves.
Internal link here: What is the glymphatic system and why does it matter? (future blog if you want a dedicated brain-drainage piece)
Sleep does not just affect tiredness — it affects pain as well
This matters a lot for the people you work with.
Poor sleep and pain have a two-way relationship. Pain can disturb sleep, but research also shows that sleep deprivation can increase pain sensitivity and lower pain thresholds. Recent reviews describe poor sleep as not just something that happens because of pain, but something that can actively worsen it.
That means if somebody is already dealing with swelling, surgical recovery, scar discomfort, persistent tension, aching joints or a nervous system that already feels on edge, poor sleep may make everything feel louder.
Not imagined.
Not weakness.
Not “just in your head”.
The system is simply less buffered.
Sleep also affects concentration, memory and that ‘brain fog’ feeling
The cognitive side is important too, because so many people say things like:
-
“I can’t think straight”
-
“I keep forgetting things”
-
“I feel fuzzy”
-
“I can’t focus on anything”
That fits the research. Sleep loss has been linked with poorer attention, slower reaction time, reduced working memory and reduced executive function. Reviews of sleep deprivation and cognition consistently show that inadequate sleep affects the very things people rely on to plan, cope, concentrate and make decisions. The NHS also lists difficulty concentrating as a common sign of sleep problems.
So when someone is exhausted and overwhelmed, it is not just that they are tired. Their thinking may genuinely be less sharp because the brain has not had what it needs.
Now bring swelling into the conversation
This is where sleep becomes especially relevant to your work.
During the day, gravity is constantly pulling fluid downwards. That is one reason people often notice:
-
heavier legs later in the day
-
tighter rings or sleeves
-
puffier ankles
-
a fuller, more uncomfortable feeling by evening
When the body is recumbent — lying down rather than upright — gravity has less pull on fluid in the limbs, and fluid can redistribute more evenly. That overnight horizontal position gives the venous and lymphatic systems a better chance to catch up. This is one reason many people notice swelling is less marked in the morning and worse by the end of the day. This is a physiologic inference based on how gravity, venous return and lymphatic drainage work, and it fits with what clinicians commonly observe.
Why is my swelling worse at the end of the day?
If someone is not getting that proper overnight reset — because sleep is poor, broken, very short, or they are spending nights upright in a chair — the body loses some of that recumbent recovery time. It is not the only reason swelling happens, but it can absolutely be one piece of the puzzle.
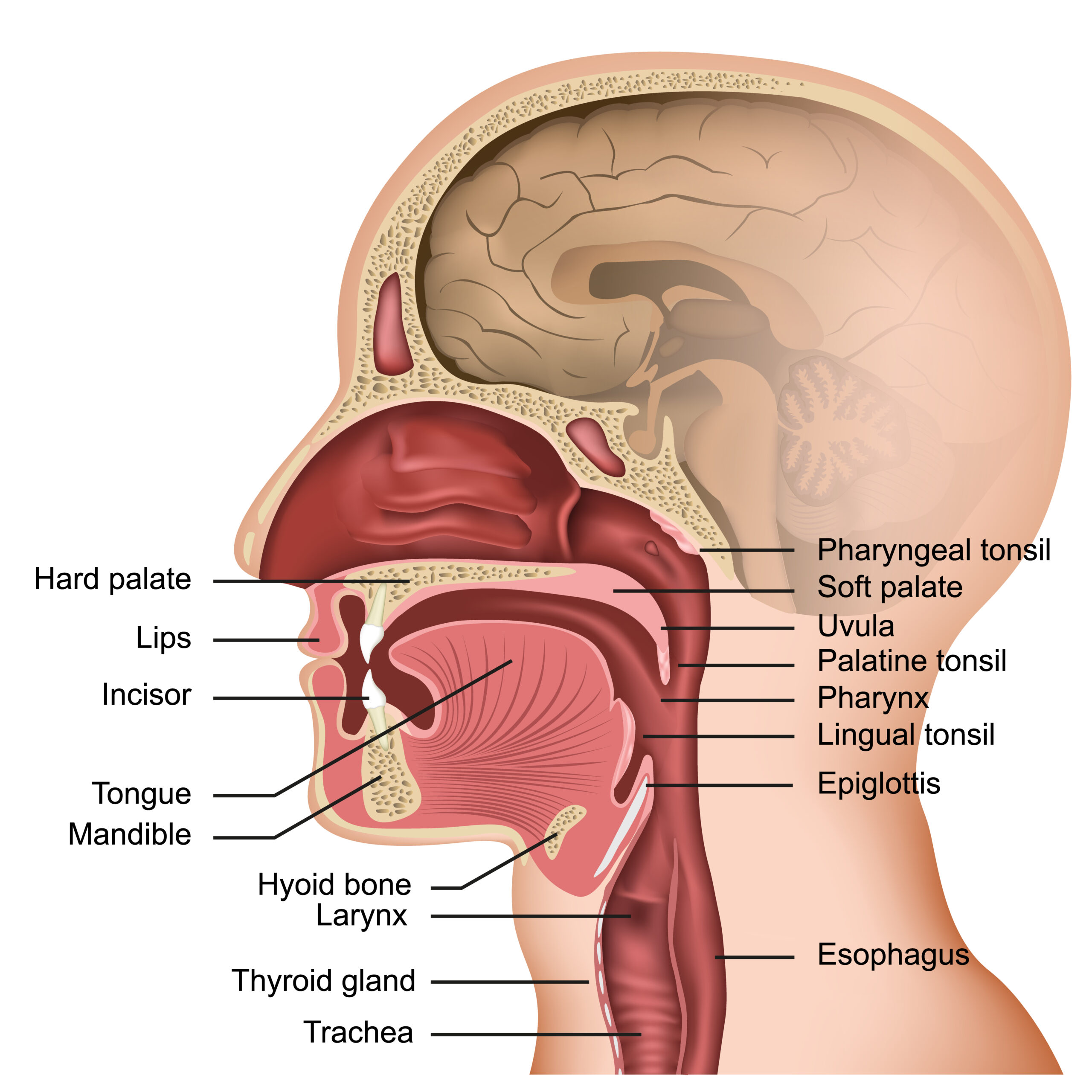
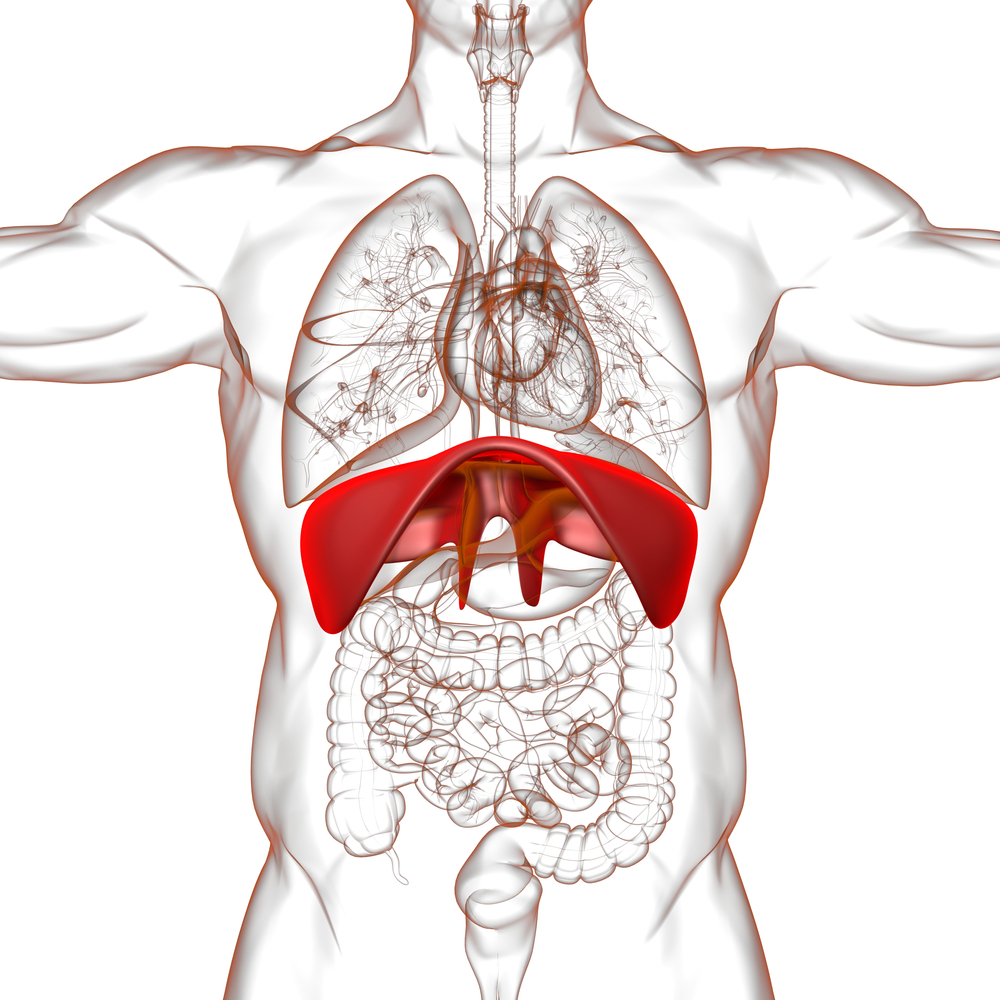
Breath matters here too
Your diaphragm is not just a breathing muscle. Its movement changes pressure through the chest and abdomen, helping venous return and supporting lymphatic flow. Calm, diaphragmatic breathing helps create one of the body’s natural pumping mechanisms for fluid movement. When breathing becomes shallow — because of stress, pain, guarded posture, fatigue or surgery — that support may reduce. This is a functional, body-systems interpretation grounded in cardiorespiratory and lymphatic mechanics.
So now we have a bigger picture:
-
sleep helps the brain clear waste
-
breathing helps support pressure changes and fluid movement
-
lying down reduces the constant downward drag of gravity
-
good sleep may help lower the inflammatory load that makes pain and swelling harder to manage
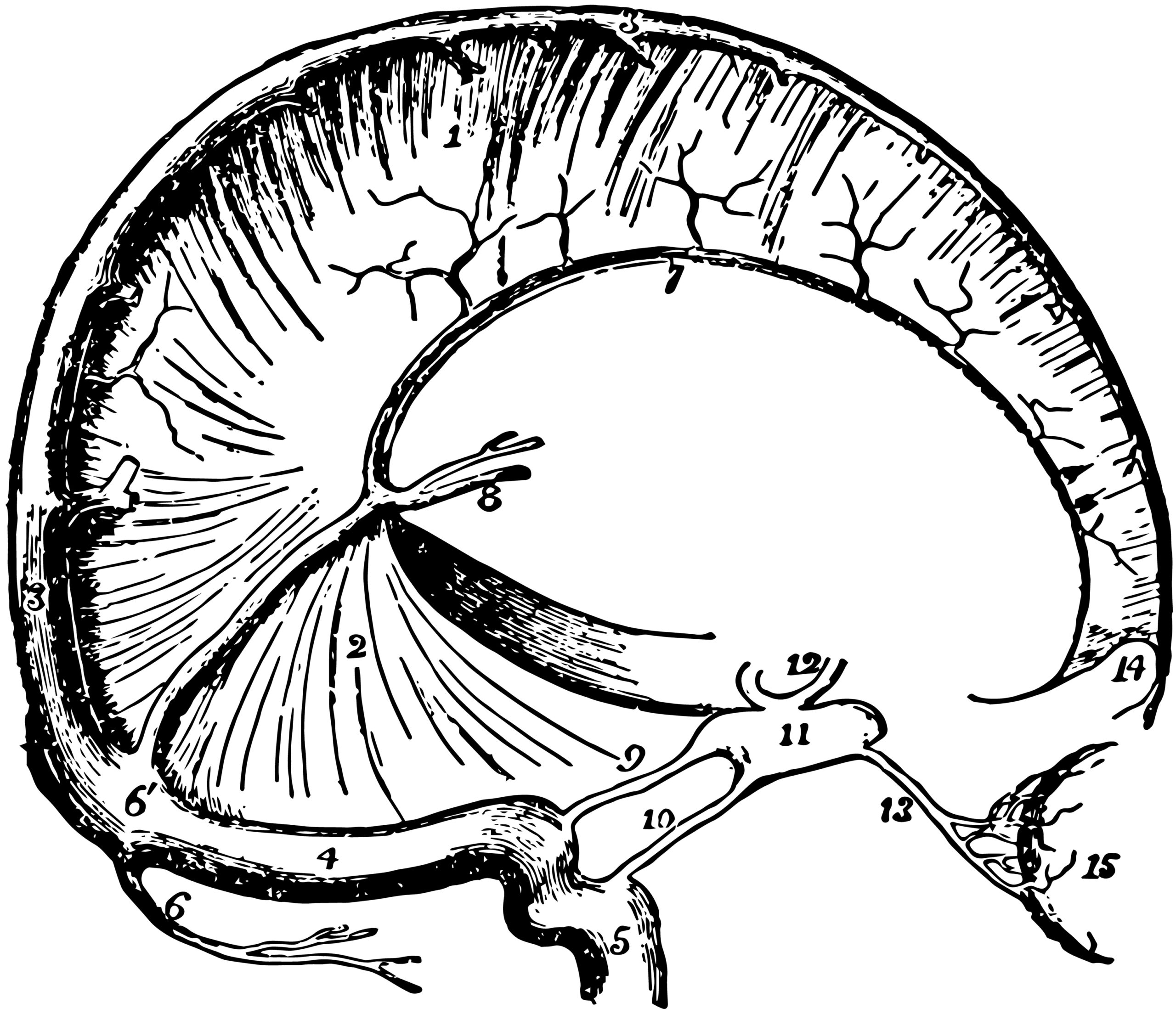
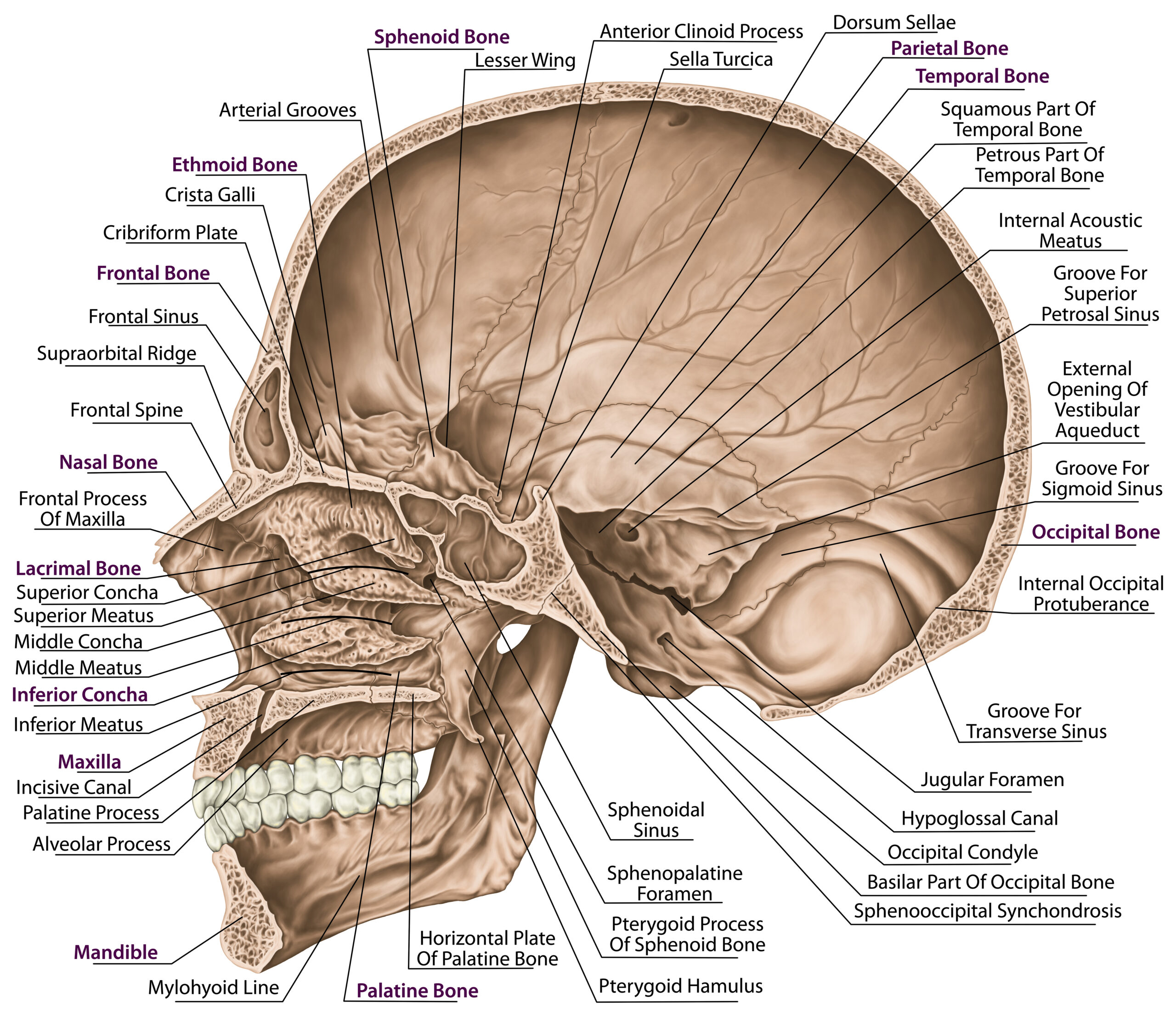
What about the tentorium, sinuses and the brain-fluid connection?
This is the more specialised layer, but it is fascinating.
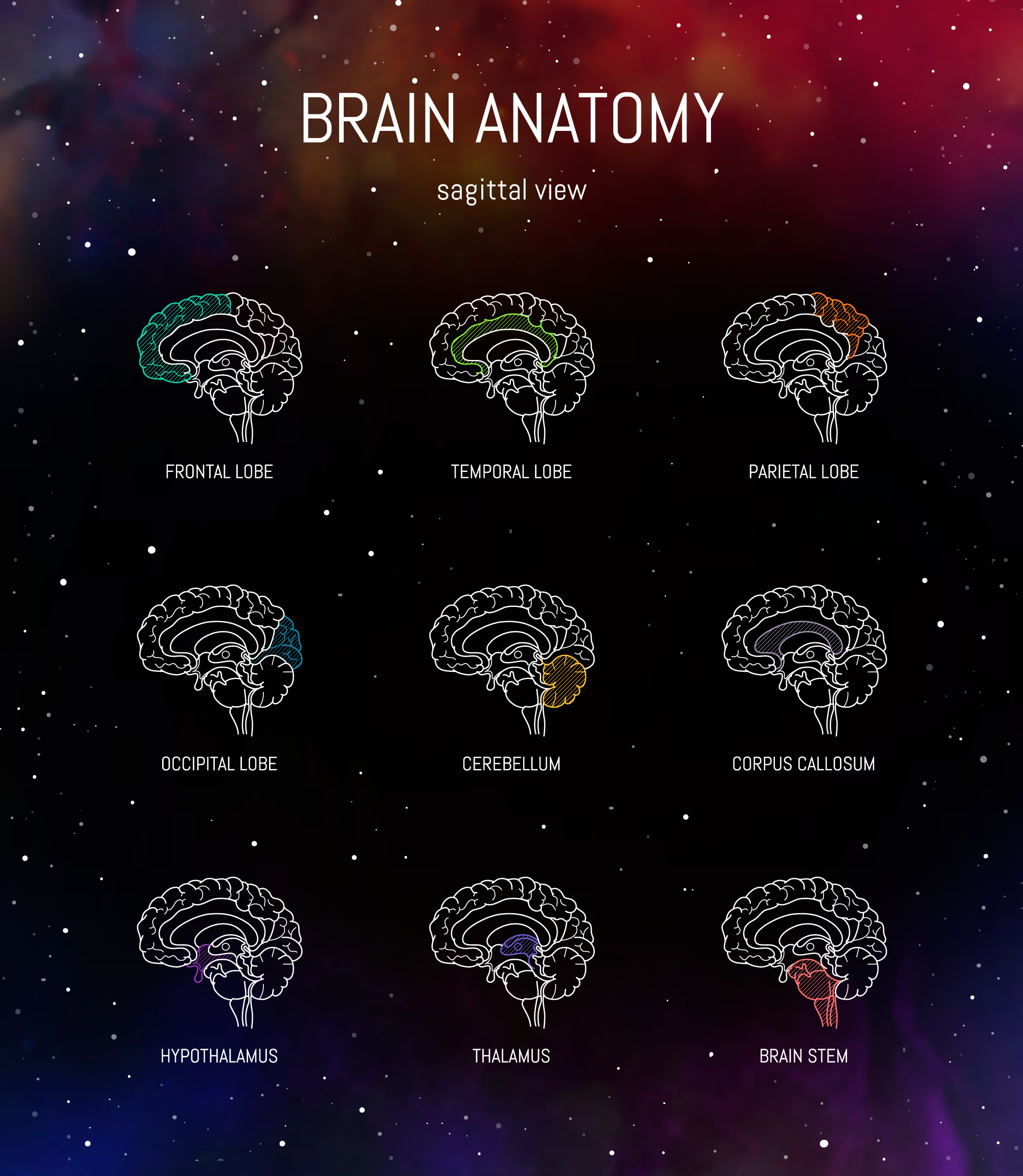
The tentorium cerebelli is a fold of dura mater inside the skull. Anatomical literature describes it as a key structural partition with close relationships to the cranial venous sinuses, including the transverse and straight sinus regions. Separate research on meningeal lymphatics shows that lymphatic elements are present in the dura and around venous sinuses, and newer reviews describe meningeal lymphatic drainage as important for central nervous system fluid balance and immune surveillance.
So while I would be careful not to oversimplify this into one neat mechanism, there is enough emerging anatomy and physiology here to say something important:
The brain, its drainage pathways, its surrounding membranes, venous sinuses, sleep state and fluid regulation are all more connected than we once thought.
That is exactly why this conversation feels so relevant.
Sleep, inflammation and swelling
Poor sleep is also linked with inflammation. Reviews of sleep loss and health describe associations with raised inflammatory signalling, including markers such as IL-6 and C-reactive protein. That matters because inflammation can amplify pain, sensitise tissues and make fluid problems feel worse.
This can create a loop that many people will recognise:
poor sleep → more pain and inflammation → more discomfort and heaviness → even poorer sleep
A simple way to think about it
You do not need to remember all the anatomy.
Just this:
Your body manages fluid better when it has
movement, breath, position and recovery.
And sleep is the one time those things can come together in a quieter, more supported way.
That is why sleep matters for:
-
healing
-
pain
-
concentration
-
inflammation
-
swelling
-
and brain health
Simple, practical support (start here)
This is not about perfect sleep.
Not everyone can lie flat comfortably — breathlessness, pain, reflux or post-surgical positioning all need to be respected.
But small, supportive changes can make a real difference.
You might try:
-
A consistent sleep and wake time (as much as life allows)
-
Lying flat for part of the night, even if not all of it
-
Gentle leg elevation if swelling is an issue
-
Noticing how your body feels morning vs evening
And importantly…
Helping your nervous system settle before sleep
Because if the body stays “on”, sleep often stays light and broken.
Simple ways to support this
-
Slow, diaphragmatic breathing
(this supports both the nervous system and fluid movement) -
Yoga Nidra (guided deep rest)
Often described as “yogic sleep”, this can help the body drop into a deeply relaxed state — even if actual sleep is difficult -
Short guided meditations
Particularly helpful if the mind feels busy or overactive at night -
Simple relaxation practices
Even 5–10 minutes of lying quietly, with no expectation to “sleep”, can help shift the system
Future internal link opportunity:
“Simple breathing and relaxation techniques to support sleep and lymphatic flow”
Sometimes the goal is not to “fix sleep”.
It is to create the conditions where the body feels safe enough to rest.
And that’s often where things begin to change.
Research snapshot
A few strong pieces behind this blog:
-
UK sleep data suggests 41% of Britons sleep six hours or less, 38% rarely feel well rested, and 14% never do.
-
The Sleep Charity reports one in three people experience sleep poverty and 37% of UK adults experience insomnia.
-
Glymphatic activity is strongly linked to sleep, and the original Xie study reported a 60% increase in interstitial space during sleep in mice.
-
Poor sleep is associated with increased pain sensitivity and worse chronic pain patterns.
-
Sleep loss affects attention, working memory, reaction time and executive function.
Sometimes it is not about doing more.
It is about giving the body the conditions it needs to do what it already knows how to do.
And often, sleep is one of the biggest missing pieces.
If sleep, swelling, heaviness or recovery feels confusing, you are not on your own with it.
Sometimes understanding the pattern is the first step. From there, gentle support can make a real difference.
I offer Manual Lymphatic Drainage, Reflexology and movement therapy to support recovery, calm an overwhelmed system and help people feel more comfortable in their bodies.
Clacton-on-Sea, Bury St Edmunds, Essex and Suffolk
